“The first time, it’ll ring interminably. Next time, it’ll go to a voicemail that just hangs up on you,” said the 48-year-old, who lives in Delaware. “Sometimes you’ll get a person who says they’re not the right one. They transfer you, and it hangs up. Sometimes, it picks up and there’s just nobody on the line.”
She spent months trying to figure out whether her Medicaid coverage had been renewed. As of late March, she hadn’t been reapproved for the year for the state-federal program, which provides health insurance for people with low incomes and disabilities.
Crouch, who suffered a debilitating brain aneurysm a decade ago, also has Medicare, which covers people who are 65 or older or have disabilities. Medicaid had been paying her monthly Medicare deductibles of $200, but she’d been on the hook for them for the past three months, straining her family’s fixed income, she said.
Crouch’s challenges with Delaware’s Medicaid call center aren’t unique. State Medicaid agencies can struggle to keep enough staff to help people sign up for benefits and field calls from enrollees with questions. A shortage of such workers can keep people from fully using their benefits, health policy researchers said.
Now, congressional Republicans’ One Big Beautiful Bill Act, which President Donald Trump signed into law last summer, will soon demand more from staff at state agencies in places where lawmakers expanded Medicaid to more low-income adults — nearly all states and the District of Columbia.
Under the law, which is expected to reduce Medicaid spending by almost $1 trillion over the next eight years, these staffers will have to not only determine whether millions of enrollees meet the program’s new work requirements but also verify more frequently that they qualify for the program — every six months instead of yearly.
—ÓĻůŚķīę√Ĺ“ēÓl Health News reached out to agencies that will need to stand up the work rules, and many said they’ll need additional staff.
The mandates will put extra strain on an already-stressed workforce, potentially making it harder for enrollees like Crouch to get basic customer service. And many could lose access to benefits they’re legally entitled to, said consumer advocates and health policy researchers, some of them with direct experience working at state agencies.
States are already “struggling significantly,” said Jennifer Wagner, the director of Medicaid eligibility and enrollment at the Center on Budget and Policy Priorities and a former associate director of the Illinois Department of Human Services. “There will be significant additional challenges caused by these changes.”
Long Wait Times for Help
Republicans argue the Medicaid changes, which will take effect Jan. 1, 2027, in most states, will encourage enrollees to find jobs. Research on other Medicaid work requirement programs has found little evidence they increase employment.
The Congressional Budget Office would cause more people to lose health coverage by 2034 than any other part of the GOP budget law. It said last year more than 5 million people could be affected.
Many states don’t have the staff to process Medicaid applications or renewals quickly, said consumer advocates and researchers.
The Centers for Medicare & Medicaid Services tracks whether states can handle the most common type of benefit application within a 45-day window.
In December, about 30% of all Medicaid and Children’s Health Insurance Program, or CHIP, applications in Washington, D.C., and Georgia to process. More than a quarter took that long in Wyoming. In Maine, 1 in 5 applications missed that deadline.
CMS began publicly sharing state Medicaid call center data in 2023, revealing a taxed system, researchers and consumer advocates said.
In Hawaii, people waited on the phone for more than three hours in December. They waited for nearly an hour in Oklahoma, and more than an hour in Nevada.
In 2023, state Medicaid agencies began making sure enrollees who were protected from being dropped from the program during the covid pandemic still qualified for coverage. That Medicaid unwinding process didn’t go well in many states, and lost their benefits.
Health policy researchers and consumer advocates say rolling out the new Medicaid rules will be a bigger challenge. The Medicaid work rules will require extensive IT system changes and training for workers verifying eligibility on a tight timeline.
“It is a much larger scale of administrative complexity,” said Sophia Tripoli, senior director of policy at Families USA, a health care consumer advocacy organization.
After months of trying to get someone on the phone, Crouch said, she finally got answers to questions about her Medicaid benefits after writing to the office of U.S. Rep. Sarah McBride (D-Del.). McBride’s office contacted the state’s Medicaid agency, which eventually called with an update, Crouch said.
Crouch didn’t qualify for Medicaid after all. She said that had never come up in two years of interactions with the state.
“It makes absolutely no sense” that the state never realized she shouldn’t have been on the program, Crouch said.
Delaware’s Medicaid agency didn’t respond to requests for comment on Crouch’s situation.
States Short-Staffed for Medicaid
Some states told —ÓĻůŚķīę√Ĺ“ēÓl Health News in late March that they’ll need more staff to roll out the work rules effectively.
Idaho said it has 40 eligibility worker vacancies. New York estimated it will need 80 new employees to handle the additional administrative work, at a cost of $6.2 million. Pennsylvania said it has nearly 400 open positions in county human services offices in the state. Indiana’s Medicaid agency has 94 open positions. Maine wants to hire 90 additional staffers, and Massachusetts wants to hire 70 more.
As of early March, Montana had filled 39 of 59 positions state officials projected it would need. The state still plans to roll out the rules early, starting July 1, despite its long struggle with system backlogs that applicants said have delayed benefits.
Missouri’s social services agency has been cutting staff and has 1,000 fewer front-line workers than it did roughly a decade ago — with more than double the number of enrollees in Medicaid and the Supplemental Nutrition Assistance Program, or SNAP, according to comments Jessica Bax, the agency director, made in November.
“The department thought that there would be a gain in efficiency due to eligibility system upgrades,” Bax said. “Many of those did not come to fruition.”
States could have a hard time finding people interested in taking those jobs, which require months-long training, can be emotionally challenging, and generally offer low pay, said Tricia Brooks, a researcher at the Georgetown University Center for Children and Families.
“They get yelled at a lot,” said Brooks, who formerly ran New Hampshire’s Medicaid and CHIP customer service program. “People are frustrated. They’re crying. They’re concerned. They’re losing access to health care, and so sometimes it’s not an easy job to take if it’s hard to help someone.”
States are paying government contractors millions of dollars to help them comply with the new federal law.
Maximus, a government services contractor, provides eligibility support, such as running call centers, in 17 states that expanded Medicaid and interacts with nearly 3 in 5 people enrolled in the program nationally, according to the company.
During a February earnings call, company leadership said Maximus can charge based on the number of transactions it completes for enrollees, independent of how many people are enrolled in a state’s Medicaid program.
Maximus has “no one-size-fits-all approach” to the services it offers or the way it charges for those services, spokesperson Marci Goldstein told —ÓĻůŚķīę√Ĺ“ēÓl Health News.
The company, which reported bringing in $1.76 billion in 2025 from the part of its business that includes Medicaid work, expects that revenue to continue to grow, even as people fall off the Medicaid rolls, “because of the additional transactions that will need to take place,” David Mutryn, Maximus’ chief financial officer and treasurer, said during the earnings call.
Losing Medicaid health coverage isn’t just an inconvenience, since many people enrolled in the program probably don’t make enough money to pay for health care on their own and may not qualify for financial help for Affordable Care Act coverage, said Elizabeth Edwards, a senior attorney with the National Health Law Program.
People could be unable to afford medications or get essential care, which could lead to “devastating” health impacts, she said.
“The human stakes of this are people’s lives,” she said.
—ÓĻůŚķīę√Ĺ“ēÓl Health News correspondents Katheryn Houghton and Samantha Liss contributed to this report.
—ÓĻůŚķīę√Ĺ“ēÓl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚ÄĒan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/medicaid/medicaid-cuts-work-requirements-state-staff-shortages/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2178951&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>He was already thinking about delaying it ‚ÄĒ then his monthly Obamacare insurance premium payment tripled this year to $2,460, about a third of his income, he said. And with a $2,700 deductible, he’d be on the hook for most of the diagnostic exam, a financial hit he said he couldn’t stomach.
“It was going to cost close to $3,000,” said Galvin, who lives in North Kingstown, Rhode Island, and recently retired as director of a durable medical equipment company. “I put it off.”
Galvin said his wife, Nancy, is delaying a costly CT scan for a few years until she too qualifies for Medicare, so it can foot the bill. The federal health program offers coverage for all Americans 65 and older.
People on Affordable Care Act plans nearing retirement age experienced some of the largest price increases following the expiration of enhanced federal subsidies at the end of December. Those with incomes above 400% of the federal poverty level ‚ÄĒ ‚ÄĒ had been getting help paying for the plans since the Biden administration expanded the subsidies during the covid-19 pandemic. Adults ages 50 through 64 of those ACA enrollees.
Now, without that federal financial help, some in this age group say they’re wrestling with whether to delay care until they qualify for Medicare. Not only does that put their physical health at risk, said patient advocates, doctors, and health policy researchers, but it potentially just shifts the costs ‚ÄĒ and could lead to taxpayers’ footing even bigger bills to fix health issues that worsen amid the delays.
“There’s going to be a lot of pent-up demand and unmet need,” said , a health policy consultant who worked in the Obama and Biden administrations. “Medicare is going to have to spend a whole heck of a lot of money covering and dealing with their treatment.”
The Affordable Care Act has been a key source of health care coverage for people 50 through 64. Access to Obamacare plans helped cut the uninsured rate for this age group by half, , a lobbying group that represents older adults. That allowed some people to retire early while keeping coverage. It also has provided a safety net for small-business owners and those with jobs that don’t offer health insurance.
Last fall, the longest-ever government shutdown occurred amid an unsuccessful effort by Democrats to extend the enhanced subsidies. Republicans opposing the extension had said the assistance went to insurers, incentivizing fraud and wasteful coverage.
The issue will continue to have political relevance, especially in this year’s midterm elections, including among older Americans who reliably show up to the polls, said Republican strategist , who runs the Atlas Strategy Group.
“Is affordability going to be an issue? Absolutely,” he said. “Are health care prices going to factor into that? Yes.”
Even before the subsidies expired, the costs of medical care, nursing homes, and prescription drugs were among the top health-related concerns for people over 50, a found.
Middle-aged adults with Obamacare plans acutely feel the pinch of the expired subsidies, because to charge adults in their 60s up to three times as much for premiums as those in their 20s, who generally use fewer medical services.
And many middle-aged adults were already enrolled in the lowest-cost plans available, which leaves them without cheaper options to fall back on, said , a policy analyst with KFF, a health information nonprofit that includes —ÓĻůŚķīę√Ĺ“ēÓl Health News.
“This is very dire for the older marketplace enrollees,” he said.
Someone making a few dollars over 400% of the federal poverty level earns too much to get a subsidy now, and in some states average premium payments were due to for this group. Many people are seeing yearly rate increases of thousands of dollars, with premium payments totaling as much as a quarter of their incomes.
, a primary care physician and health policy researcher at the University of Michigan, said he has regular conversations with older patients who are trying to figure out how to afford their medical care. Some in their early 60s are likely to drop ACA coverage because of rising premiums, he said.
“That’s a gamble,” he added.
Marci Heinbaugh may take that bet. The 63-year-old social services worker, who lives in rural Illinois, said her monthly premium payments more than doubled, from roughly $1,100 to $2,333, for a plan with a $10,150 out-of-pocket maximum.
She knew she’d be paying more, she said, but wasn’t anticipating that kind of increase. A few months in, she’s not sure if she’ll stick with the plan for the rest of the year. She said she may go uninsured.
“I’m petrified to even think about that,” Heinbaugh said.
People want to buy their own insurance on the marketplace, and many middle-aged adults could afford it with just a little federal financial help, said , senior vice president of public policy at AARP. Those who drop coverage or delay care until they reach age 65 might save money now, but that could be more costly for them ‚ÄĒ and taxpayers ‚ÄĒ later.
“There’s significant possibility that the purported savings associated with reducing subsidies as people approach retirement end up turning into higher utilization costs for Medicare,” Weil said.
And Medicare enrollees aren’t insulated from rising costs. In January, for example, standard Medicare from $185 per month to almost $203.
Until Galvin joins Medicare, he said, he expects to burn through a $30,000 retirement account to cover his marketplace plan’s premium payments and deductible.
A found that 1 in 5 adults over 50 had no retirement savings and 3 in 5 were worried they wouldn’t have enough retirement savings to support themselves.
The expiration of these Obamacare subsidies puts additional financial pressure on Americans as they approach retirement, health policy researchers said.
“It’s forcing people to make impossible choices,” said , director of federal health advocacy for the national nonprofit Justice in Aging.
Are you struggling to afford your health insurance? Have you decided to forgo coverage? Click here to contact —ÓĻůŚķīę√Ĺ“ēÓl Health News and share your story.
—ÓĻůŚķīę√Ĺ“ēÓl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚ÄĒan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-care-costs/health-costs-middle-aged-adults-delay-affordable-care-act-obamacare-medicare/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2169414&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>LISTEN: Can’t afford health insurance this year? Don’t be afraid to talk to your doctor about money and the cost of care. On WAMU’s “Health Hub” on March 4, —ÓĻůŚķīę√Ĺ“ēÓl Health News correspondent Sam Whitehead shared tips for people seeking affordable options without skipping care.
Health insurance could be out of reach for many Americans in 2026.
About a for Affordable Care Act marketplace coverage this year. The Congressional Budget Office told lawmakers that more could opt out in coming years after the GOP-led Congress let expire subsidies that helped many afford a plan. Meanwhile, plan premiums jumped, and new, stricter Medicaid eligibility rules kicked in.
If you lost health insurance this year, there may be ways to see the doctor without breaking the bank. On March 4, in conversation with WAMU host Esther Ciammachilli, —ÓĻůŚķīę√Ĺ“ēÓl Health News correspondent Sam Whitehead shared tips on .
Renuka Rayasam and Taylor Cook contributed reporting.
—ÓĻůŚķīę√Ĺ“ēÓl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚ÄĒan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/insurance/listen-wamu-health-hub-insurance-costs-tips-affordable-care/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2164599&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>The 59-year-old, who lives in Harrisburg, North Carolina, closed her nonprofit circus arts school last year because she could no longer see well enough to complete paperwork. She then worked making dough at a pizza shop for a bit. Currently, she sorts recyclable materials, including cans and bottles, at a local concert venue. It is her main source of income ― but the work isn’t year-round.
“This place knows me, and this place loves me,” Kelley said of her employer. “I don’t have to explain to this place why I can’t read.”
Kelley, who lives in a camper, survives on less than $10,000 a year. She says that’s possible, in part, because of her Medicaid health coverage, which pays for arthritis and anxiety medications and has enabled doctor visits to manage high blood pressure.
But she worries about losing that coverage next year, when rules take effect requiring millions of people like Kelley to work, volunteer, attend school, or perform other qualifying activities for at least 80 hours a month.
“I’m scared right now,” she said.


Before the coverage changes were signed into law, Republican lawmakers suggested that young, unemployed men were taking advantage of the government health insurance program that provides coverage to millions of low-income or disabled people. Medicaid is not intended for “29-year-old males sitting on their couches playing video games,” House .
But, in reality, adults ages 50 to 64, particularly women, are likely to be , said Jennifer Tolbert, deputy director of the Program on Medicaid and the Uninsured at KFF, a health information nonprofit that includes —ÓĻůŚķīę√Ĺ“ēÓl Health News. For Kelley and others, the work requirements will create barriers to keeping their coverage, Tolbert said. Many could lose Medicaid as a result, putting their physical and financial health at risk.
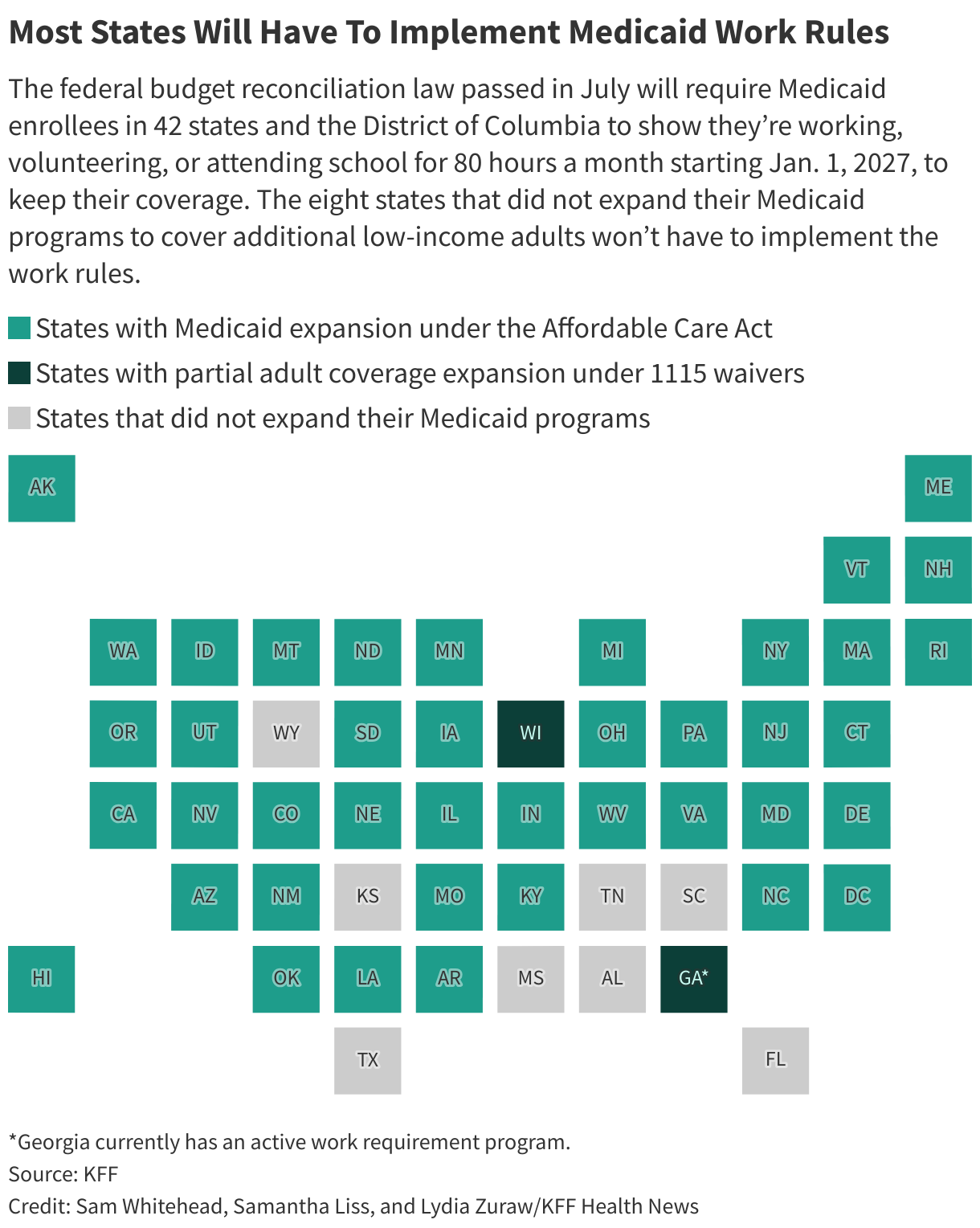
Starting next January, some 20 million low-income Americans in 42 states and Washington, D.C., will need to meet the activity requirements to gain or keep Medicaid health coverage.
Alabama, Florida, Kansas, Mississippi, South Carolina, Tennessee, Texas, and Wyoming didn’t expand their Medicaid programs to cover additional low-income adults under the Affordable Care Act, so they won’t have to implement the work rules.
The nonpartisan Congressional Budget Office predicts the work rules will result in at least 5 million fewer people with Medicaid coverage over the next decade. Work rules are the largest driver of coverage losses in the GOP budget law, which slashes nearly $1 trillion to offset the costs of tax breaks that mainly benefit the rich and increase border security, .
“We’re talking about saving money at the expense of people’s lives,” said Jane Tavares, a gerontology researcher at the University of Massachusetts Boston. “The work requirement is just a tool to do that.”

Department of Health and Human Services spokesperson Andrew Nixon said requiring “able-bodied adults” to work ensures Medicaid’s “long-term sustainability” while safeguarding it for the vulnerable. Exempt are people with disabilities, caregivers, pregnant and postpartum individuals, veterans with total disabilities, and others facing medical or personal hardship, Nixon told —ÓĻůŚķīę√Ĺ“ēÓl Health News.
Medicaid expansion has provided a lifeline for middle-aged adults who otherwise would lack insurance, according to . Medicaid covers 1 in 5 Americans ages 50 to 64, giving them access to health coverage before they qualify for Medicare at age 65.
Among women on Medicaid, those ages 50 through 64 are more likely to face challenges keeping their coverage than their younger female peers and are likely to have a greater need for health care services, Tolbert said.
These middle-aged women are less likely to be working the required number of hours because many serve as family caregivers or have illnesses that limit their ability to work, Tolbert said.
Tavares and other researchers found that of the total Medicaid population is considered “able-bodied” and not working. This group consists largely of women who are very poor and have left the workforce to become caretakers. Among this group, 1 in 4 are 50 or older.
“They are not healthy young adults just hanging out,” the researchers stated.
Plus, making it harder for people to maintain Medicaid coverage “may actually undermine their ability to work” because their health problems go untreated, Tolbert said. Regardless, if this group loses coverage, their chronic health conditions will still need to be managed, she said.
Adults often start wrestling with health issues before they’re eligible for Medicare.
If older adults don’t have the means to pay to address health issues before age 65, they’ll ultimately be sicker when they qualify for Medicare, costing the program more money, health policy researchers said.
Many adults in their 50s or early 60s are no longer working because they’re full-time caregivers for children or older family members, said caregiver advocates, who refer to people in the group as “the sandwich generation.”


The GOP budget law does allow some caregivers to be exempted from the Medicaid work rules, but the carve-outs are “very narrow,” said Nicole Jorwic, chief program officer for the group Caring Across Generations.
She worries that people who should qualify for an exemption will fall through the cracks.
“You’re going to see family caregivers getting sicker, continuing to forgo their own care, and then you’re going to see more and more families in crisis situations,” Jorwic said.
Paula Wallace, 63, of Chidester, Arkansas, said she worked most of her adult life and now spends her days helping her husband manage his advanced cirrhosis.
After years of being uninsured, she recently gained coverage through her state’s Medicaid expansion, which means she’ll have to comply with the new work requirements to keep it. But she’s having a hard time seeing how that will be possible.
“With me being his only caregiver, I can’t go out and work away from home,” she said.
Wallace’s husband receives Social Security Disability Insurance, she said, and the law says she should be exempt from the work rules as a full-time caregiver for someone with a disability.
But federal officials have yet to issue specific guidance on how to define that exemption. And experience from Arkansas and Georgia ― the only states to have run Medicaid work programs ― shows that many enrollees struggle to navigate complicated benefits systems.
“I’m very concerned,” Wallace said.
—ÓĻůŚķīę√Ĺ“ēÓl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚ÄĒan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-care-costs/medicaid-work-requirements-middle-aged-adults-women/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2151346&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>The 27-year-old resident of Bloomington, Indiana, has a pacemaker and a painful joint disease. She also has fused vertebrae in her neck from a spinal injury, preventing her from turning her head.
Indiana’s Medicaid agency currently considers Brader “medically frail,” giving her access to an expanded set of benefits, such as physical therapy.
New federal rules will require more than 18 million Medicaid enrollees nationwide to show they’re working, volunteering, or going to school for 80 hours a month starting in 2027 to keep their coverage. Brader is exempt as long as she’s deemed medically frail.
But lacking sufficient federal guidance, states are wrestling with how to define medical frailty — a consequential decision that could cut Medicaid coverage for many people, said state officials, consumer advocates, and health policy researchers.
“It’s terrifying,” Brader said. “I already have fought so hard to get my health care.”
‘Incredibly High’ Stakes
President Donald Trump’s One Big Beautiful Bill Act slashes nearly $1 trillion from Medicaid over the next decade, with much of the savings projected to come from no longer covering those who don’t qualify under the new work rules. Those spending cuts help offset the costs of GOP priorities, such as extra border security and tax cuts that mainly benefit the wealthy.
Conservative lawmakers have argued that Medicaid, the government health insurance program for people with low incomes or with disabilities, has grown too large and expensive, especially in the wake of its expansion to more low-income adults under the Affordable Care Act. They also say that requiring participants to work is common sense.
The work rules in Trump’s tax-and-spending law offer exemptions for several groups who might struggle to meet them, including people deemed “medically frail.” The law spells out certain “medically frail” conditions such as blindness, disability, and substance use disorder. But it does not list many others.
Instead, the law exempts those with a “serious or complex medical condition,” a term whose interpretation could vary by state.
State officials say they need more clarity to ensure that people who cannot work for health reasons retain rightful access to Medicaid. They also worry that, even with a clear definition, people will face the onerous task of having to regularly vouch for being medically frail, which is a challenge without reliable access to medical care.
“The stakes are incredibly high,” said Kinda Serafi, a partner at consulting firm Manatt Health.
The new work requirements will affect Medicaid recipients in 42 states and Washington, D.C. Eight states — Alabama, Florida, Kansas, Mississippi, South Carolina, Tennessee, Texas, and Wyoming — did not expand their Medicaid programs to cover additional low-income adults, so they won’t have to implement the work rules.
The Medicaid work rules are expected to be the over the next decade, according to the nonpartisan Congressional Budget Office.
Forty-four percent of all adults covered by states’ expanded Medicaid programs , according to KFF.

A Challenge for States
State Medicaid agencies are scrambling to implement the rules with little direction from the U.S. Department of Health and Human Services, which has yet to issue specific guidance. Federal officials will clarify the “medically frail” definition next year, said Andrew Nixon, an agency spokesperson.
Ultimately, states will have to decide who is unhealthy enough to be exempt from work rules. And it won’t be easy for state workers and their computer systems to track.
Every year, state eligibility systems screen millions of applicants to check if they qualify for Medicaid and other government programs. Now, these same systems must screen applicants and existing enrollees to determine whether they meet the new work rules.
Jessica Kahn, a partner at consulting firm McKinsey & Co., has urged states to start planning how to adapt eligibility systems to verify work status. States can do a “tremendous amount” of work without direction from the federal government, said Kahn, a former federal Medicaid systems official, who spoke during a recent Medicaid advisory panel hearing. “Time is a-wasting already.”
State Medicaid directors are pondering the challenge.
“Medical frailty gets so complex,” Emma Sandoe, Oregon’s Medicaid director, said during a recent panel discussion. Conditions that can keep people from working, such as mental health disorders, can be hard to prove, she said.
A state might try to use data pulled from a person’s health records, for instance, to determine medical frailty. But information from a patient’s chart may not paint a clear picture of someone’s health, especially if they lack regular access to medical care.
It’s a tall order for eligibility systems that historically have not had to scrape medical records to screen applicants, said Serafi of Manatt Health.
“That is an incredibly new thing that eligibility enrollment systems are just not fluent in at all,” Serafi said.
Lobbying groups for the private health insurance companies that help run Medicaid in many states also have urged federal regulators to clearly define medical frailty so it can be applied uniformly.
In a Nov. 3 letter to federal officials, the Medicaid Health Plans of America and the Association for Community Affiliated Plans advocated for allowing enrollees to qualify for the exemption by saying on their applications that they have conditions that make them medically frail. Successfully implementing exemptions for the medically frail will be “crucial” given the “severe health risks of coverage loss for these populations,” the groups said.
Some state officials worry about unintended consequences of the work rules for people with chronic conditions.

Jennifer Strohecker, who recently resigned as Utah’s Medicaid director, reiterated the high stakes, especially for those with diabetes on Medicaid. They may be very healthy and functional with insulin, but if they fail to complete the work requirements, that may change, Strohecker said during a recent Medicaid advisory hearing.
Whether someone is deemed medically frail already depends heavily on where they live.
For example, in Arkansas, people indicate on their Medicaid applications that they’re disabled, blind, or need help with daily living activities.
Approximately 6% of the roughly 221,000 people enrolled in Arkansas’ Medicaid expansion program are deemed medically frail, according to Gavin Lesnick, a spokesperson for the Arkansas Department of Human Services.
In West Virginia, the state accepts a medical frailty designation when an applicant self-reports it.
The burden of proof is higher in North Dakota. Applicants there must answer a questionnaire about their health and submit additional documentation, which may include medical chart notes and treatment plans. More than half of applicants were denied last year, according to Health and Human Services Department spokesperson Mindy Michaels.
Indiana’s Family and Social Services Administration, which runs its Medicaid program, declined an interview and said it could not comment on individual cases, like Brader’s.
Brader worries the additional red tape will cause her to lose Medicaid again. She said she was temporarily kicked off the program in 2019 for failing to meet the state’s work rules when Indiana said her work-study job didn’t count as employment.
“Anytime I have tried to receive help from the state of Indiana, it has been a bureaucratic nightmare,” she said.
As states await federal guidance, Kristi Putnam, a senior fellow at the conservative Cicero Institute and former secretary of the Arkansas Department of Human Services, which oversees the state Medicaid program, said even if a state creates an extensive list of qualifying “medically frail” conditions, the line must be drawn somewhere.
“You can’t possibly create a policy for exemptions that will catch everything,” she said.
—ÓĻůŚķīę√Ĺ“ēÓl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚ÄĒan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-care-costs/medicaid-work-rules-exempt-medically-frail-who-qualifies/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2120581&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>The texts were part of a pilot run to test technology the Trump administration says will make it easier for some Medicaid enrollees to prove they meet new requirements ‚ÄĒ working, studying, job training, or volunteering at least 80 hours a month ‚ÄĒ set to take effect in just over a year.
But only 894 people completed the quarterly wage check, or just under 7% of enrollees who got the text, according to Drew Maranto, undersecretary for the Louisiana Department of Health.
“We’re hoping to get more to opt in,” Maranto said. “We plan to raise awareness.”
The clock is ticking for officials in 42 states ‚ÄĒ excluding those that did not expand Medicaid at all ‚ÄĒ and Washington, D.C., to figure out how to verify that an estimated 18.5 million Medicaid enrollees meet rules included in President Donald Trump’s tax and spending law. They have until the end of next year, and federal officials are giving those jurisdictions a total of $200 million to do so.
The policy change is one of several to free up money for Trump’s priorities, such as increased border security and tax breaks that mainly benefit the wealthy.
The nonpartisan Congressional Budget Office has said the millions of people won’t be able to access health insurance over the next decade. It estimates changes to the Medicaid program will result in 10 million fewer Americans covered by 2034 ‚ÄĒ more than half of them because of the eligibility rules.
For now, state officials, health policy researchers, and consumer advocates are watching the pilot program in Louisiana and another in Arizona. , director of the Centers for Medicare & Medicaid Services, has touted those test-drives and said they will allow people to verify their incomes “within seven minutes.”
“There have been efforts to do this in the past, but they haven’t been able to achieve what we can achieve because we have technologies now,” said Oz, in August.
Brian Blase, the president of the conservative Paragon Health Institute and a key architect of Medicaid changes in the new law, has chimed in, saying during a that with today’s artificial intelligence “people should be able to seamlessly enter how they are spending their time.”
—ÓĻůŚķīę√Ĺ“ēÓl Health News found scant evidence to support such claims. Federal and state officials have offered little insight into what new technology the two pilots have tested. They do say, however, that it connects directly with the websites of Medicaid enrollees’ payroll providers, rather than using artificial intelligence to draw conclusions about their activities.
Oz said the Trump administration’s efforts started “as soon as the bill was signed” in July. But work on the pilot programs .
And Medicaid is a state-federal program: The federal government contributes most of the funds, but it is up to the states to administer them, not the federal government.
“Oz can say, ‚ÄėOh no, we’re going to fix this. We’re going to do this.’ Well, they don’t actually run the program,” said , a health policy researcher at Georgetown’s Center for Children and Families.
Officials have also offered few details about the pilots’ effectiveness in assisting enrollees in Medicaid or other public benefit programs.
The shortage of information has some state officials and health policy researchers worried that the Trump administration lacks viable solutions to help states implement the work rules. As a result, they say, people with a legal right to Medicaid benefits could lose access to them.
“What actually keeps me up at night is the fear that members that are eligible for Medicaid and are trying to get health care services would fall through the cracks and lose coverage,” said Emma Sandoe, Oregon’s Medicaid director.
Officials involved in the Louisiana and Arizona projects declined to answer many specific questions about their efforts, instead directing —ÓĻůŚķīę√Ĺ“ēÓl Health News to federal officials.
Spokespeople for Arizona’s Medicaid and Economic Security departments ‚ÄĒ Johnny Córdoba and Brett Bezio, respectively ‚ÄĒ did not share data on how many people participated in the state’s pilot test nor describe the outcome. They said the pilot had been used to verify eligibility only for the federal Supplemental Nutrition Assistance Program, a smaller program than Medicaid.
The , a nonprofit that helps people sign up for such SNAP benefits, hadn’t heard of the pilot program.
State officials and health policy researchers said neither pilot program could confirm whether a person meets other qualifying activities ‚ÄĒ such as community service ‚ÄĒ or any of the numerous exemptions. The tools being tested can verify only income.
Andrew Nixon, director of communications for the U.S. Department of Health and Human Services, which oversees Oz’s agency, wrote in a statement that the digital tools officials aim to share with states “are largely under development.”
One person is Michael Burstein, who until recently worked at the U.S. Digital Service, which later became known as the Department of Government Efficiency.
As the U.S. Digital Service was turned into DOGE, Burstein and other staffers left and started a nonprofit called to finish supporting the technology to make it easier for people to verify their incomes for Medicaid enrollment.
But without permission from state officials, Burstein would not describe the tool in development, aside from saying that it’s mobile-first, can quickly verify income for a new or returning client, “and we’re pretty happy with it.”
The state agencies that manage benefit programs, such as Medicaid and SNAP, are understaffed, and they use different eligibility systems, many of which need updating, which makes improving them “a challenging task,” he said.
The $200 million in start-up costs the federal government has earmarked for systems to track work requirements equals roughly four times what it cost to administer Georgia’s Medicaid work requirement program alone.
That state, which has the nation’s only active work requirement program, called Georgia Pathways to Coverage, in September was granted a , despite a from a federal watchdog saying it hadn’t received enough federal oversight. A complicated sign-up process has kept enrollment in the program far below Georgia’s own projections.
Trump’s tax and spending law allows states to ask for extra time ‚ÄĒ until the end of 2028 ‚ÄĒ to start enforcing the rules, but only with the approval of HHS Secretary Robert F. Kennedy Jr. It also allows counties with high unemployment rates to be exempted, but states must apply for that exemption.
Even with an app that states can use to prove people are eligible for Medicaid, enrollees would still need to know that app existed and how to use it ‚ÄĒ neither of which is a given, Alker said. There is also no guarantee they’d have reliable cell service or internet access. As —ÓĻůŚķīę√Ĺ“ēÓl Health News has reported, millions of Americans live in rural areas without reliable internet.
Private vendors also have been working on such apps, said , who researches Medicaid eligibility and enrollment at the Center on Budget and Policy Priorities. Wagner said she has seen several vendors demonstrate products they plan to pitch to states for the work rules. Many are limited in scope, she said, like those in the pilot tests.
“Nobody has a magical solution that’ll make sure eligible people don’t lose coverage,” she said.
—ÓĻůŚķīę√Ĺ“ēÓl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚ÄĒan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-care-costs/medicaid-eligibility-tool-pilot-test-work-requirements-ai-louisiana-arizona-georgia/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2103530&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>“We’re going to take care of the sickest patients first,” Margo, a family medicine physician, said.
It’s not like there was space on that June afternoon anyway. A small monitor on the wall pulsed with the vitals of current patients, who filled the ER. An ambulance idled outside in the South Texas heat with a patient waiting for a bed to open up.
“Everybody shows up here,” Margo said. “When you’re overwhelmed and you’re overrun, there’s only so much you can do.”
Starr County, a largely rural, Hispanic community on the southern U.S. border, when it voted Republican in a presidential election for the first time in more than a century. Immigration and the economy in this community, where roughly a third of the population falls below the poverty line.

Now, recent actions by the Trump administration and the GOP-controlled Congress have triggered a new concern: the inability of doctors, hospitals, and other health providers to continue to care for uninsured patients. It’s a fear not only in Starr County, which has one of the highest uninsured rates in the nation. Communities across the U.S. with similarly high proportions of uninsured people could struggle as additional residents lose health coverage.
About 14 million fewer Americans are expected to have health insurance in a decade due to President Donald Trump’s new tax-and-spending law, which Republicans dubbed the One Big Beautiful Bill Act, and the pending expiration of enhanced subsidies that slashed the price of Affordable Care Act plans for millions of people. The new law also that send billions of dollars to help those who care for uninsured people stay afloat.
“You can’t disinsure this many people and not have, in many communities, just a collapse of the health care system,” said Sara Rosenbaum, founding chair of the Department of Health Policy and Management at George Washington University’s Milken Institute School of Public Health.
“The future is South Texas,” she said.
—ÓĻůŚķīę√Ĺ“ēÓl Health News is examining the impact of national health care policy changes on uninsured people and their communities. Though the Trump administration told —ÓĻůŚķīę√Ĺ“ēÓl Health News it is making “a historic investment in rural health care,” people who treat low-income patients, as well as researchers and consumer advocates, say recent policy decisions will make it harder for people to stay healthy. Doctors, hospitals, and clinics that make up the health care safety net could lose so much money they must close their doors, some of them warn.
“Because the patient’s bill is not going to get paid,” said Joseph Alpert, editor-in-chief of The American Journal of Medicine and a professor of medicine at the University of Arizona. “Uninsured patients stress the health care system.”
Starr County shows how this dynamic unfolds.
Primary care doctors in the county serve an average of each, nearly three times the U.S. average.
Margo, the family physician, said because so many people lack insurance and there are so few places to seek care, many residents treat the ER as their first stop when they’re sick.
In many cases, they have neglected their health, making them sicker and more expensive to treat. And requires ERs at hospitals in the Medicare program to stabilize or transfer patients, regardless of their ability to pay.
That leaves Margo and his team to practice what he described as “disaster medicine.”
“They come in with chest pain or they stop breathing. They collapse. They’ve never seen a doctor,” Margo said. “They’re literally dying.”
Health Systems in ‘Survival Mode’
When people are uninsured or on Medicaid, they tend to rely on a safety net of doctors, hospitals, clinics, and community health centers, which offer services free of charge or absorb getting reimbursed at lower rates than they do treating patients on commercial insurance.
Those providers’ financial situations can often be precarious, leading them to rely on myriad federal supports. The Trump administration’s cuts to health care and Medicaid in the name of eliminating “waste, fraud, and abuse” have many concerned they won’t weather the additional financial strain.
Trump’s new law funds his priorities, like extending tax cuts that mainly benefit wealthier Americans and expanding immigration enforcement. Those costs are covered in part by a nearly $1 trillion reduction in federal health spending for Medicaid within the next decade and changes to the ACA, such as requiring additional paperwork and shortening the time for people to sign up.
Many Republicans have argued Medicaid has gotten too large and strayed from the state-federal program’s core mission of covering those with low incomes and disabilities. And the GOP has fought to roll back the ACA since its passage.
Kush Desai, a spokesperson for the White House, said projections from the nonpartisan Congressional Budget Office about how many people could lose health insurance are an “overestimate.” He did not provide an estimate the administration sees as more accurate.
Supporters of the “One Big Beautiful Bill” say those who need health coverage can still get it if they meet new requirements such as working in exchange for Medicaid coverage.
And Michael Cannon, director of health policy studies at the Cato Institute, a libertarian think tank, said even with the legislation, Medicaid spending will grow, just not as quickly.
The budget law won’t cause “the sky to fall,” Cannon said. “The inefficient providers should be shutting down.”
from AMGA, formerly the American Medical Group Association, which represents health systems across the country, found nearly half of rural facilities could close or restructure due to Medicaid cuts. Nearly three-quarters of respondents said they anticipated layoffs or furloughs, including of front-line clinicians.
Public health departments, which often fill gaps in care, also face federal funding cuts that have reduced their capacity. In South Texas’ Cameron County, the health department has eliminated nearly a dozen positions, said agency head Esmer Guajardo. In neighboring Hidalgo County, the health department has laid off more than 30 people, said Ivan Melendez, who helps oversee its operations.
In July, the Texas Department of State Health Services , a massive annual event that last year provided free health services to nearly 6,000 South Texas residents.
Gateway Community Health Center in Laredo, a border city north of the Rio Grande Valley, is in “survival mode,” with about a third of patients already lacking insurance and even more who will struggle to afford health care if the ACA subsides aren’t renewed, said David Vasquez, its director of communications and public affairs. The center is looking for other forms of funding to avoid layoffs or cuts to services, and its expansion and hiring plans are on hold, Vasquez said.
That downsizing is happening as more people lose health insurance and need free or reduced-cost care.
Esther Rodriguez, 39, of McAllen has been out of work for two years and her husband makes $600 a week working in construction. Neither of them has health insurance.
Medicaid covered the bills for the births of her five children. Now, she depends on a mobile health clinic run by a local medical school, where she can pay out-of-pocket for routine checkups and drugs to control her Type 2 diabetes. If she needed more care, Rodriguez said, she would go to the ER.
“You have to adapt,” she said in Spanish.
‘Death by a Thousand Cuts’
People’s inability to pay results in uncompensated care, or services that hospitals, doctors, and clinics don’t get paid for, which, under an earlier version of the megabill, was projected to increase by $204 billion over the next decade, , a nonprofit think tank.
But the Trump administration is also cutting other support that helped offset the cost of care for people who can’t pay. The new law caps federal programs that many health providers for low-income people have come to depend on, especially in rural areas, to shore up their budgets. These include taxes on hospitals, health plans, and other providers that states use to help fund their Medicaid programs. Such provider taxes are a “financial gimmick,” Desai said.
While the law creates a temporary $50 billion fund to support rural doctors and hospitals, that’s a little over a third of estimated Medicaid funding losses in rural areas, , a health information nonprofit that includes —ÓĻůŚķīę√Ĺ“ēÓl Health News. Desai called the analysis “flawed.”
Any loss in revenue could spell financial ruin, especially for small rural hospitals, said Quang Ngo, president of the Texas Organization of Rural & Community Hospitals Foundation.
“It’s kind of like death by a thousand cuts,” he said. “Some will probably not make it.”
And the hits could keep coming. The Trump administration’s budget request for the coming fiscal year calls for cuts to multiple rural health programs operated through the Health Resources and Services Administration. Desai said the spending law’s investment in rural health “dwarfs” the cuts.
In February, the Trump administration announced funding cuts of 90% to the ACA navigator program, which helps people find health insurance. That program has been “historically inefficient,” Desai said.
In December 2023, nearly 3 million of Texas’ uninsured were eligible for ACA subsidies, Medicaid, or the Children’s Health Insurance Program, , a public policy think tank.

Maria Salgado spends her workdays tabling at community events, dropping off flyers at doctors’ offices, and holding one-on-one meetings with clients of MHP Salud, a nonprofit that connects residents to Medicaid and ACA coverage.
She worried funding cuts would really set the organization’s efforts back: “A lot of community members here, they’re going to be left behind,” said Salgado, a community health worker, or promotora.
Chris Casso, a primary care physician who grew up in McAllen and now practices there, held back tears as she described treating patients who have put off seeing a doctor because of an inability to pay, only to have their preventable conditions deteriorate.
She worries about the future of her community as , potentially leaving few providers to treat uninsured people.
“It’s heartbreaking,” she said, sitting in a small back room in her office in a suburban strip mall, wedged between a Kohl’s and a Shoe Carnival. “These are hardworking people,” she said. “They try their best to take care of themselves.”
Casso said her own sister, who worked as a medical biller in a physician’s office, couldn’t afford health insurance. She delayed care and died at age 45 of complications from diabetes and heart disease. Casso worries the future will find more people in similar situations.
“Our population is going to suffer,” she said. “It’s going to be devastating.”

This <a target="_blank" href="/health-care-costs/uninsured-texas-rio-grande-valley-strain-local-health-systems-medicaid-aca/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2085435&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>
Patients begin lining up before dawn at , an annual five-day health clinic in Texas’ Rio Grande Valley. Many residents in this predominantly spanning the Mexican border lack insurance, making the health fair a major source of free medical care in South Texas for more than 25 years.
Until this year. The Trump administration’s plan to strip in federal public health and pandemic funds from Texas helped prompt just before its scheduled July 21 start.
“Some people come every year and rely on it,” said Hidalgo County Health and Human Services Director Dairen Sarmiento Rangel. “Some people even camp out outside of Border Health so they can be the first in line to receive services. This event is very important to our community.”
States and local governments have made painful program cuts in the wake of major reductions in federal health funding that have already taken effect. Now, they’re sizing up the financial hits to come ‚ÄĒ some not until late next year or beyond ‚ÄĒ from the “,” the tax and spending law congressional Republicans passed in July that enacts much of President Donald Trump’s domestic agenda.
Texas, for instance, expects to see its federal Medicaid funds reduced by as much as over 10 years due to new barriers for enrollment, such as more frequent eligibility checks, according to a July analysis by KFF.
Taken together, the reductions amount to a seismic shift in how state health programs are provided and paid for. The administration is, in effect, pushing a significant amount of health costs to states. That will force their leaders to make difficult choices, as many state budgets are already strained by declining tax revenues, a slowdown in federal pandemic spending, and economic uncertainty.
Revenue forecasters have lowered expectations for the coming year, according to a .
“It’s almost inevitable that states will enact a number of cuts to health services because of the fiscal pressure,” said Wesley Tharpe, senior adviser for state tax policy at the left-leaning .
Some are proactively trying to stanch the impact.
Hawaii lawmakers are looking to aid nonprofits that are already contending with federal funding cuts. They’re in grants to health, social service, and other nonprofits hit by federal funding cuts. To get the money, nonprofits must show a termination or drop in funding, or that they have otherwise been harmed by the cuts.
“It is not fair that organizations dedicated to supporting the people of Hawaii are being forced to scale back due to federal funding cuts,” Democratic Gov. Josh Green .
Other states are scaling back projects to contend with cuts. Delaware Gov. Matt Meyer, a Democrat, received notice in March that the Trump administration was in public health funding from the state. The next month, state legislative leaders halted a planned project to upgrade and expand the Capitol complex as a result.
“We recognized that the reckless federal cuts to the social safety nets of thousands of Delawareans called for us to hold back resources to protect our most vulnerable,” said , president pro tempore of the Delaware Senate.
In New Mexico, the state with the , a bipartisan group of lawmakers voted to create a trust fund to boost funding for the program. About 10% of the more than covered by Medicaid and the related Children’s Health Insurance Program could lose their health coverage under the federal spending law, based on .
Some state leaders are warning constituents that the worst may be yet to come.
At an Aug. 18 event at a hospital in the South Bronx section of New York City, New York Gov. Kathy Hochul, a Democrat, stood on stage among health care workers in white coats to skewer Trump’s new law.
“What Republicans in Washington have done through the ‚ÄėBig Ugliest Bill’ I’ve ever seen is literally screwing New Yorkers,” she said. The state’s health system is bracing for in annual cuts.
And in California, lawmakers weighed the impact of the coming cuts from the federal law at a general assembly , where some Democratic legislators said state efforts to protect reproductive health services and other programs were in jeopardy.
“We’ve been bracing for this reality: President Trump’s so-called ‚ÄėBig, Beautiful Bill’ is now law,” Democratic lawmaker Gregg Hart said at the hearing, calling it a “direct assault on California’s core programs and our values.”
“Sadly, the reality is, the state does not have the capacity to backfill all of these draconian federal funding cuts in the current budget,” Hart said. “We cannot simply write a check and make this go away.”

The sweeping budget law, which passed without any Democratic support, will reduce federal spending on Medicaid by about over the next decade, based on estimates from the . The spending reductions largely come from the imposition of a on people who’ve obtained Medicaid under the Affordable Care Act’s expansion, as well as other new barriers to coverage.
The law will mean more than 7.5 million people will lose Medicaid coverage and become uninsured, according to the Congressional Budget Office, while extending tax cuts for wealthy people who, Democrats say, don’t need them. Republicans and Trump have said the spending package and its accompanying program cuts were necessary to prevent fraud and waste, and to sustain Medicaid, a state-federal program for people with disabilities and lower incomes.
“The One Big Beautiful Bill removes illegal aliens, enforces work requirements, and protects Medicaid for the truly vulnerable,” the White House said in a .
The Medicaid cuts won’t begin until after the midterm elections in November 2026, but other cuts have already hit.
The Trump administration has sought to claw back earmarked to states because of the pandemic, spurring a with a coalition of Democratic-led states. It also in for mental health services in schools, and halted grants from the National Institutes of Health that provided money to more than 90 public universities.
HHS press secretary Emily Hilliard said the agency is prioritizing investments that advance Trump’s mandate to confront chronic disease. She defended some of the cuts and said, erroneously, that the spending law doesn’t cut Medicaid.
“The covid-19 pandemic is over, and HHS will no longer waste billions of taxpayer dollars responding to a crisis that Americans moved on from years ago,” she said.
State leaders say the pandemic funding the administration wants returned was earmarked for other public health measures, such as tracking emerging diseases, outbreak responses, and staffing. State attorneys general in May won a against the administration.
“What we’re seeing now is states anticipating big cuts in Medicaid coming, but they’re also dealing with a whole variety of federal cutbacks in public health programs that are smaller but still quite meaningful,” said , executive vice president for health policy at KFF, a health information nonprofit that includes —ÓĻůŚķīę√Ĺ“ēÓl Health News.
Part of the challenge for states is simply understanding the changes.
“I think it’s fair to say there is concern, confusion, and uncertainty,” said Kathryn Costanza, a Medicaid expert at the National Conference of State Legislatures.
States are struggling to sort it all out, forming that are , suing to try to block the cuts, and reallocating funding.
In Colorado, lawmakers to let state Medicaid dollars pay for non-abortion care at Planned Parenthood of America clinics after Trump’s law banned federal funding for such care. Whether the ban holds up in court .
The Louisiana Legislature to state universities to make up for cuts to federal research funding, much of which goes to health-related research.
And in South Dakota, the state’s largest food bank has to make up for funding cuts to the U.S. Department of Agriculture.
States must balance their budgets every year, so cuts put many services at risk if state lawmakers are unwilling to raise taxes. The work will begin in earnest in January, when many states begin new legislative sessions.
And the tough choices are likely to continue. Congressional House Republicans are considering legislation that could , including by slashing the generous cost sharing the federal government provides for 20 million adults who enrolled in Medicaid under the ACA’s Medicaid expansion.
Some states will roll back their Medicaid expansions and cut more health programs as a result.
—ÓĻůŚķīę√Ĺ“ēÓl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚ÄĒan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-care-costs/state-budget-fallout-trump-health-funding-cuts-obbba/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2084813&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>
MIAMI ‚ÄĒ GOP lawmakers in the 10 states that refused the Affordable Care Act’s Medicaid expansion for over a decade have argued their conservative approach to growing government programs would pay off in the long run.
Instead, the Republican-passed budget law that includes many of President Donald Trump’s priorities will pose at least as big a burden on patients and hospitals in the expansion holdout states as in the 40 states that have extended Medicaid coverage to more low-income adults, hospital executives and other officials warn.
For instance, Georgia, with a population of just over 11 million, will see as many people lose insurance coverage sold through ACA marketplaces as will California, with more than triple the population, , a health information nonprofit that includes —ÓĻůŚķīę√Ĺ“ēÓl Health News.
The new law imposes additional paperwork requirements on Obamacare enrollees, slashes the time they have each year to sign up, and cuts funding for navigators who help them shop for plans. Those changes, all of which will erode enrollment, are expected to have far more impact in states like Florida and Texas than in California because a higher proportion of residents in non-expansion states are enrolled in ACA plans.
The budget law, which Republicans called the “One Big Beautiful Bill,” will cause sweeping changes to health care across the country as it trims federal spending on Medicaid by more than $1 trillion over the next decade. The program covers more than 71 million people with low incomes and disabilities. Ten million people will lose coverage over the next decade due to the law, according to the nonpartisan .
Many of its provisions are focused on the 40 states that expanded Medicaid under the ACA, which added millions more low-income adults to the rolls. But the consequences are not confined to those states. A proposal from conservatives to cut more generous federal payments for people added to Medicaid by the ACA expansion didn’t make it into the law.
“Politicians in non-expansion states should be furious about that,” said Michael Cannon, director of health policy studies at the Cato Institute, a libertarian think tank.
The number of people losing coverage could accelerate in non-expansion states if enhanced federal subsidies for Obamacare plans expire at the end of the year, driving up premiums as early as January and adding to the rolls of uninsured. KFF estimates as many as 2.2 million people could become uninsured just in Florida, a state where lawmakers refused to expand Medicaid and, partly as a result, now .
For people like Francoise Cham of Miami, who has Obamacare coverage, the Republican policy changes could be life-altering.
Before she had insurance, the 62-year-old single mom said she would donate blood just to get her cholesterol checked. Once a year, she’d splurge for a wellness exam at Planned Parenthood. She expects to make about $28,000 this year and currently pays about $100 a month for an ACA plan to cover herself and her daughter, and even that strains her budget.
Cham choked up describing the “safety net” that health insurance has afforded her ‚ÄĒ and at the prospect of being unable to afford coverage if premiums spike at the end of the year.
“Obamacare has been my lifesaver,” she said.
If the enhanced ACA subsidies aren’t extended, “everyone will be hit hard,” said , a health policy expert with Manatt Health, a consulting and legal firm, and a former deputy administrator for the Centers for Medicare & Medicaid Services.
“But a state that hasn’t expanded Medicaid will have marketplace people enrolling at lower income levels,” she said. “So, a greater share of residents are reliant on the marketplace.”
Though GOP lawmakers may try to cut Medicaid even more this year, for now the states that expanded Medicaid largely appear to have made a smart decision, while states that haven’t are facing similar financial pressures without any upside, said health policy experts and hospital industry observers.
—ÓĻůŚķīę√Ĺ“ēÓl Health News reached out to the governors of the 10 states that have not fully expanded Medicaid to see if the budget legislation made them regret that decision or made them more open to expansion. Spokespeople for Republican Gov. Henry McMaster of South Carolina and Republican Gov. Brian Kemp of Georgia did not indicate whether their states are considering Medicaid expansion.
Brandon Charochak, a spokesperson for McMaster’s office, said South Carolina’s Medicaid program focuses on “low-income children and families and disabled individuals,” adding, “The state’s Medicaid program does not anticipate a large impact on the agency’s Medicaid population.”
Enrollment in ACA marketplace plans nationwide has more than doubled since 2020 to 24.3 million. If enhanced subsidies expire, by more than 75% on average, according to an analysis by KFF. Some insurers are already signaling they plan to charge more.
The CBO estimates that allowing enhanced subsidies to expire will without health insurance by 4.2 million by 2034, compared with a permanent extension. That would come on top of the coverage losses caused by Trump’s budget law.
“That is problematic and scary for us,” said Eric Boley, president of the Wyoming Hospital Association.
He said his state, which did not expand Medicaid, has a relatively small population and hasn’t been the most attractive for insurance providers ‚ÄĒ few companies currently offer plans on the ACA exchange ‚ÄĒ and he worried any increase in the uninsured rate would “collapse the insurance market.”
As the uninsured rate rises in non-expansion states and the budget law’s Medicaid cuts loom, lawmakers say state funds will not backfill the loss of federal dollars, including in states that have refused to expand Medicaid.
Those states got slightly favorable treatment under the law, but it’s not enough, said Grace Hoge, press secretary for Kansas Gov. Laura Kelly, a Democrat who favors Medicaid expansion but who has been rebuffed by GOP state legislators.
“Kansans’ ability to access affordable healthcare will be harmed,” Hoge said in an email. “Kansas, nor our rural hospitals, will not be able to make up for these cuts.”
For hospital leaders in other states that have refused full Medicaid expansion, the budget law poses another test by limiting financing arrangements states leveraged to make higher Medicaid payments to doctors and hospitals.
Beginning in 2028, the law will reduce those payments by 10 percentage points each year until they are closer to what Medicare pays.
Richard Roberson, president of the Mississippi Hospital Association, said the state’s use of what’s called directed payments in 2023 helped raise its Medicaid reimbursements to hospitals and other health institutions from $500 million a year to $1.5 billion a year. He said higher rates helped Mississippi’s rural hospitals stay open.
“That payment program has just been a lifeline,” Roberson said.
The budget law includes a $50 billion fund intended to insulate rural hospitals and clinics from its changes to Medicaid and the ACA. But found it would offset only about one-third of the cuts to Medicaid in rural areas.
Trump encouraged Florida, Tennessee, and Texas to continue refusing Medicaid expansion in his first term, when his administration gave them an unusual 10-year extension for financing programs known as uncompensated care pools, which generate billions of dollars to pay hospitals for treating the uninsured, said Allison Orris, director of Medicaid policy for the left-leaning think tank Center on Budget and Policy Priorities.
“Those were very clearly a decision from the first Trump administration to say, ‚ÄėYou get a lot of money for an uncompensated care pool instead of expanding Medicaid,’” she said.
Those funds are not affected by Trump’s new tax-and-spending law. But they do not help patients the way insurance coverage would, Orris said. “This is paying hospitals, but it’s not giving people health care,” she said. “It’s not giving people prevention.”
States such as Florida, Georgia, and Mississippi have not only turned down the additional federal funding that Medicaid expansion brings, but most of the remaining non-expansion states spend less than the national average per Medicaid enrollee, provide fewer or less generous benefits, and cover fewer categories of low-income Americans.
Mary Mayhew, president of the Florida Hospital Association, said the state’s Medicaid program does not adequately cover children, older people, and people with disabilities because reimbursement rates are too low.
“Children don’t have timely access to dentists,” she said. “Expectant moms don’t have access nearby to an OB-GYN. We’ve had labor and delivery units close in Florida.”
She said the law will cost states more in the long run.
“The health care outcomes for the individuals we serve will deteriorate,” Mayhew said. “That’s going to lead to higher cost, more spending, more dependency on the emergency department.”
—ÓĻůŚķīę√Ĺ“ēÓl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚ÄĒan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-care-costs/medicaid-expansion-holdout-states-unrewarded-trump-health-policy/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2067640&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Alexander tried signing up for Pathways, the state’s limited Medicaid expansion, multiple times and got denied each time, he said, even though he met the qualifying terms because he’s a full-time student.
Georgia is one of 10 states that haven’t expanded Medicaid health coverage to a broader pool of low-income adults. Instead, it offers coverage to those who can prove they’re working or completing 80 hours a month of other qualifying activities, like going to school or volunteering. And it is the only state currently doing so.
“Why is this marketing out here?” said the 20-year-old, who lives in Conyers, east of Atlanta. “It’s truly not accessible.”
Each denial used the same boilerplate language, Alexander said, and his calls to caseworkers were not returned. State offices couldn’t connect him with caseworkers assigned to him from the same state agency. And when he requested contact information for a supervisor to appeal his denial, he said, the number rang to a fax machine.
“It’s impenetrable,” Alexander said. “I’ve literally tried everything, and there’s no way.”
Millions of Americans trying to access Medicaid benefits could soon find themselves navigating similar byzantine state systems and work rules. Legislation signed into law by President Donald Trump on July 4 allocates $200 million to help states that expanded Medicaid create systems by the end of next year to verify whether some enrollees are meeting the requirements.
Conservative lawmakers have long argued that public benefits should go only to those actively working to get off of government assistance. But the nation’s only Medicaid work requirement program shows they can be costly for states to run, frustrating for enrollees to navigate, and disruptive to other public benefit systems. Georgia’s budget for marketing is nearly as much as it has spent on health benefits. Meanwhile, most enrollees under age 65 or have a barrier that prevents them from doing so.
What Georgia shows is “just how costly setting up these administrative systems of red tape can be,” said Joan Alker, executive director of Georgetown University’s Center for Children and Families.
Over the past two years, —ÓĻůŚķīę√Ĺ“ēÓl Health News has documented the issues riddling Georgia’s Pathways program, launched in July 2023. More than 100,000 Georgians have applied to the program through March. Just over 8,000 were enrolled at the end of June, though about if the state fully expanded Medicaid under the terms of the Affordable Care Act.
The program has cost more than $100 million, with only $26 million spent on health benefits and more than $20 million allocated to marketing contracts, according to a —ÓĻůŚķīę√Ĺ“ēÓl Health News analysis of state reports.
“That was truly a pretty shocking waste of taxpayer dollars,” Alker said.
The Government Accountability Office is investigating the costs of the program after a group of Democratic senators — including both members of the Georgia delegation — asked the government watchdog to look into the program. Findings are expected this fall.
A state report to the federal government from March said Georgia couldn’t effectively determine if applicants meet the qualifying activities criteria. The report also said the state hadn’t suspended anyone for failing to work, a key philosophical pillar of the program. Meanwhile, as of March, more than 5,000 people were waiting to have their eligibility verified for Pathways.
The Pathways program has strained Georgia’s eligibility system for other public benefits, such as food stamps and cash assistance.
In April, the state applied to the federal government to renew Pathways. In its application, officials scaled back key elements, such as the requirement that enrollees document work every month. Critics of the program also say the red tape doesn’t help enrollees find jobs.
“Georgia’s experience shows that administrative complexity is the primary outcome, not job readiness,” said Natalie Crawford, executive director of Georgia First, which advocates for fiscal responsibility and access to affordable health care.
Despite the struggles, Garrison Douglas, a spokesperson for Georgia’s Republican governor, Brian Kemp, defended the program. “Georgia Pathways is doing what it was designed to do: provide free healthcare coverage to low-income, able-bodied Georgians who are willing to engage in one of our many qualifying activities,” he said in an emailed statement.
New federal requirements in the tax and spending legislation mean that the 40 states (plus Washington, D.C.) that expanded Medicaid will need to prepare technology to process the documentation some Medicaid recipients will now have to regularly file.
The federal law includes exemptions for people with disabilities, in addiction treatment, or caring for kids under 14, among others.
The Trump administration said other states won’t face a bumpy rollout like Georgia’s.
“We are fully confident that technology already exists that could enable all parties involved to implement work and community engagement requirements,” said Mehmet Oz, head of the Centers for Medicare & Medicaid Services, in an emailed statement.
In a written public comment on Georgia’s application to extend the program, Yvonne Taylor of Austell detailed the difficulties she faced trying to enroll.
She said she tried to sign up several times but that her application was not accepted. “Not once, not twice, but 3 times. With no response from customer service,” she wrote in February. “So now I am without coverage.”
Victoria Helmly of Marietta wrote in a January comment that she and her family members take care of their dad, but the state law doesn’t exempt caregivers of older adults.
“Georgia should recognize their sacrifices by supporting them with health insurance,” she wrote. “Let’s simplify this system and in the end, save money and lives.”
—ÓĻůŚķīę√Ĺ“ēÓl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚ÄĒan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/insurance/georgia-pathways-to-coverage-medicaid-work-requirements-gop-bill-implementation/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2061267&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>