The plan was to begin handing out boxes of groceries at 11, but the truck delivering the food blew a tire en route. No one complained.
Perry Hall was among those waiting. His wife, Lilly Hall, volunteers with the distribution team. Perry has been dealing with a form of cancer called multiple myeloma. The Halls get by on around $1,500 a month from his Social Security benefits, plus assistance from the federal , or SNAP. But because of her age, Lilly, 59, recently became subject to new SNAP work requirements and at risk of losing her benefits.
As part of the federal One Big Beautiful Bill Act, all “able-bodied adults” 64 or younger who don’t have dependents and don’t work, volunteer, or participate in job training at least 80 hours a month are now restricted to three months of benefits every three years from SNAP, formerly known as food stamps. Previously, the federal requirement applied to those 54 or younger. The new rule, which went into effect in November, also applies to parents of children 14 or older. And it removed exemptions for veterans, people experiencing homelessness, and young adults who’ve aged out of foster care.
Proponents of work requirements argue that they incentivize people who are “work-ready” to seek and keep jobs, reducing dependence on government assistance and upholding the “.”
Rhonda Rogombé serves as health and safety net policy analyst for the . She and her colleagues have studied the effects of SNAP work rules and found that requiring recipients to work does not lower an area’s unemployment rate.
Previous work requirements were suspended nationwide during the covid pandemic and reinstated in fall 2023. The researchers found that the average number of people employed in Mingo County each month actually went down after the requirement was reimposed.
A 2018 federal research project that examined several data sources, including SNAP data from nine states, found that work requirements “have no impact on labor force participation and the number of hours worked.”
There are a number of possible explanations, Rogombé said, “but when people are hungry, they’re not able to support themselves. When people are hungry, it’s harder to focus at work. It’s harder to engage in work activity, and we think that that’s part of it.”
Jobs are scarce in this southern West Virginia county. Lilly Hall found work at a Delbarton restaurant. But it’s unpaid until a waitress position opens ŌĆö enough to preserve her benefits, but far from ideal.
On that mild Wednesday in late March, House of Hope provided chicken, eggs, bread, potatoes, fresh fruit and vegetables, and milk.
Among those in line were older residents and “some young people that have lost their way and they can’t get work and they just need help,” said Timothy Treleven, who operates the pantry with his wife, Christine, and Gail Lendearo.

House of Hope’s scheduled distribution day is the last Saturday of each month ŌĆö supplemented by occasional weekday Facing Hunger visits ŌĆö as money from monthly checks begins to run out and cupboards go bare.
On a typical Saturday, pantry staff and volunteers hand out up to 400 boxes of food.
“It’s an honor to do this,” Lendearo said. “It’s a blessing.”
Perry Hall’s cancer is now in remission, but for a while his treatment required that he and Lilly travel back and forth, 4┬Į hours each way, to Morgantown. The couple’s van couldn’t make the trip, so they paid a friend for rides.
Mingo’s population is just under 22,000, down from around 27,000 in 2010. It once flourished, fueled by coal. Williamson, the county seat, was home to an opera house and businesses operated by immigrants from Italy, Russia, and Syria. The region is still referred to as “the coalfields,” but little is mined here these days. .
Rogombé and her colleagues found that Mingo County residents face significant barriers to securing what few jobs are available. These include unreported physical and mental impairments, housing insecurity, and a lack of high school diplomas and identification documents.

Filing the paperwork to receive benefits or to confirm compliance is difficult for many residents. The West Virginia Center on Budget and Policy’s research found that about 1 in 4 lack reliable internet access.
Additional changes lie ahead for the SNAP program. Currently, the federal government and the states share administrative costs equally, but in October states will assume 75% of those costs. And beginning in October 2027, they’ll be required to pay additional costs based on .
Kentucky, like West Virginia, is among the poorer states that will be most affected by the new requirements and costs. The Kentucky Center for Economic Policy estimates that with the expanded work requirements.
Jessica Klein, a researcher with the center, worries about the consequences. “We know SNAP has an impact on health, and not just because it decreases food insecurity,” she said. It worsens blood pressure rates, obesity, medication adherence, and more.
With the additional financial burden placed on states, “I think what we’ll see is some states changing rules that impact participation in order to have a smaller, more affordable program,” Klein said. “My fear is that some states will choose not to operate SNAP at all.”
In Mingo County, folks are stepping up. At least eight food pantries offer groceries to those in need.
Janet Gibson runs the Blessing Barn pantry in the Ben Creek community. “I can go from one end of the creek to the other” and tell you everyone’s name and a little something about them, she said. She takes pride in feeding her people.

Gibson said it can be hard to find even volunteer opportunities in the county, largely because of transportation challenges. A look at a local map can be misleading: A couple of dozen miles into a holler or up a ridge could take an hour or more.
“Whether you’re working full-time or not, you’re still spinning out gas to get to work,” Gibson said, “and gas ain’t cheap now.”
A single mother of three, Trista Shankle of Paducah, Kentucky, isn’t subject to the new SNAP requirements, but she worries about the fragility of the social safety net. She overcame challenges, is earning a master’s degree in social work, and works for an organization that connects community college students with benefits. Her family receives SNAP, Medicaid, housing support, and assistance from the USDA’s . If any one of those is cut, she said, she may have to drop out of school.
Shankle is certain she wouldn’t have advanced to where she is today without the benefits she and her family have received: “They bring a sense of calm and comfort. I know that my kids aren’t going to go hungry.”
The first week in April, Lilly Hall reported for work at Black Bear Trails Restaurant. She’s grateful for the opportunity. And when a waitress slot opens, “I’ll snag that position so quick it’ll make your head flip.”
čŅ╣¾Õ·┤½├ĮęĢŅl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFŌĆöan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/medicaid/food-stamps-snap-work-requirements-hunger-west-virginia-foodbanks/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2228111&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>More than 80 of his customers who were enrolled in the same Medicare supplemental plan from the insurer Chubb got hit last August with a 45% increase.
“In my 49 years of doing biz as a broker, I’ve never seen a premium increase be effective immediately on everyone, instead of on their policy anniversary,” said Jaggi, whose brokerage scrambled to find more affordable options for clients. The policies pick up deductibles and other costs not covered in traditional Medicare, and without one there is no upper limit on how much a consumer might owe each year.
While 45% was an unusually big jump, Jaggi and other brokers say double-digit premium increases for Medicare supplemental, or Medigap, policies are becoming the norm.
A Chubb spokesperson did not respond to requests for comment on the increase.
More than 12 million people ŌĆö of those in traditional Medicare ŌĆö buy a Medigap policy. Others rely on some sort of retiree employer coverage or a different backup. About 13% of people in traditional Medicare don’t have supplemental coverage, according to KFF, meaning they could be vulnerable to large costs if they have a serious illness.
In the supplemental market, following big increases last year, rates appear to be rising again. In early 2026 filings with state insurance commissioners from Aetna, Blue Cross Blue Shield, Cigna, Humana, Mutual of Omaha, and UnitedHealthcare, rate increases for Plan G policies ŌĆö the most commonly purchased supplement type ŌĆö ranged from just in the first quarter, according to Nebraska-based consulting firm Telos Actuarial.
“While this is a small dataset across a select number of states, it’s an indication that carriers are looking to correct their premium rates in light of upward pressure on their claims experience,” said Brett Mushett, a consulting actuary with Telos.
Climbing Numbers
Premium rates vary based on the type of coverage chosen, where a beneficiary lives, and their age. For Plan G coverage, beneficiaries paid an in 2023, according to KFF. That amount has likely risen since.
“In some states, like Ohio, Medicare supplements for years would have a 3% to 5% year-over-year increase. Now it’s 10% to 15%,” said Amanda Brewton, owner of Medicare Answers Now, a marketing organization whose clients are sales agents.
In Alaska, Premera Blue Cross raised the premiums on its Plan G policies by nearly 12% for this year, according to rate sheets provided to čŅ╣¾Õ·┤½├ĮęĢŅl Health News by insurance agent Patricia Mack, who said another insurer raised rates by nearly 13%.
For example, a 65-year-old woman who last year would have been charged $172 a month for a Plan G policy would now face a monthly rate of $192, said Mack, who owns Alaska Insurance Benefits in Wasilla.
Premera spokesperson Courtney Wallace said in an email that Medicare makes changes to deductible and copayment rates each year, which affects supplemental plans that cover those increasing amounts.
Wallace also noted that the insurer saw higher medical service use among its members, “which further drove claims costs and ultimately impacted premiums.”
Agents and policy experts blame a range of factors for rising premiums: an increase in the use of medical services by beneficiaries; the aging of the population; increases in labor and medical costs; rules in some states governing Medigap plans; and people’s enrolling in ŌĆö or getting out of ŌĆö private Medicare Advantage plans.
“Five years ago, it was exceedingly uncommon to have a carrier with a rate increase of more than 10%. Now it’s very uncommon to see a rate increase below 10%, and it’s not uncommon to see it over 20%,” said Chalen Jackson, vice president for government affairs at Integrity, a Dallas-based company that sells life and health insurance.
Jaggi, who co-owns Jaggi Petry Insurance & Investments in Forsyth, Illinois, along with his daughter, said he eventually found other options for many of those 80-plus clients with the large increase, which came from an insurer that had previously been the lowest-cost option. But it wasn’t easy ŌĆö and continuing increases are expected.
“These are unbelievable increases,” said Jaggi, who said he is seeing premium hikes exceeding 15% this year across a range of insurers.
Policy experts have outlined possible solutions, including for Congress to cap out-of-pocket costs for Medicare beneficiaries or subsidize the purchase of Medigap coverage.
“Traditional Medicare is the only federal health insurance program without an out-of-pocket cap,” Sen. Ron Wyden (D-Ore.) wrote in an email, adding that the program “needs to be updated and strengthened to protect the Medicare guarantee for American seniors.”
But making changes to Medicare that require congressional approval is unlikely in the current legislative environment, especially because adding an out-of-pocket cap would add costs to the federal budget.
How This Plays Out
People generally qualify for Medicare when they turn 65. Beneficiaries after they initially enroll in the traditional fee-for-service program to purchase a Medigap plan at standard rates without having to answer health-related questions.
Strict rules then kick in around when beneficiaries can enroll in or switch Medigap coverage and options become much more limited, with each one generally involving trade-offs or tough choices.
have what’s known as a “birthday rule,” which requires insurers once a year to allow people enrolled in a Medigap plan to change to different supplemental coverage ŌĆö usually around their birthdays ŌĆö without being medically underwritten. Those rules can help consumers, including those with health conditions, to switch.
An additional ŌĆö Connecticut, Massachusetts, Maine, and New York ŌĆö require insurers to offer at least one Medigap policy to all applicants either year-round or during an annual enrollment period, depending on the state. Changes are allowed no matter the person’s health.
Another option for those facing high Medigap costs is to leave traditional Medicare and enroll in a private-sector Medicare Advantage plan, which have out-of-pocket caps. But joining one means beneficiaries must generally rely on a set of in-network doctors and hospitals. And if they change their mind and want to go back to traditional Medicare, they have only a 12-month window in which to purchase a Medigap plan without passing health questions. After that, it can be more difficult.
“A lot of people don’t know that if they are in Medicare Advantage for a year, they can get turned down by a Medigap plan or charged really high premiums because of a preexisting condition, which for many people effectively traps them in MA plans,” said , a research associate at the liberal Center for American Progress and co-author of a on the issue.
There are some exceptions. For example, if a Medicare Advantage plan withdraws from a market or leaves the Medicare program, its enrollees can qualify for a supplemental plan without being asked health questions or charged more for having preexisting conditions.
For this year alone, about 2.6 million people when their insurer pulled out of their markets, according to KFF, and more than a million lost coverage for 2025. Many switched to other MA plans, but “somewhere around 440,000 of those people did go to a Medicare supplement policy,” sometimes because there was no other MA plan in their area, said George Dippel, president of Deft Research, a Minneapolis-based market research organization focused on insurance for older people. Deft is part of Integrity, the Dallas company.
Some Medicare experts note that anytime insurers enroll people whose health status they can’t consider ŌĆö whether because of birthday rules or because their Medicare Advantage plan left the market and thus qualified them for an exemption from medical underwriting ŌĆö it potentially exposes them to more health care utilization and higher costs, making them more likely to increase premiums across the board to offset the possible financial hit.
Another option mentioned by brokers for people looking to lower their costs is to consider one of the two types of Medigap plans that come with a deductible, which is currently just under $3,000 for a year. Those plans charge far lower monthly premiums than Medigap plans that pick up a much larger portion of annual amounts people must pay toward their Medicare services.
Still, “a lot of people are not comfortable with a $3,000 deductible,” Mack said.
čŅ╣¾Õ·┤½├ĮęĢŅl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFŌĆöan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/medicare/medigap-medicare-advantage-premiums-rate-increase-few-alternatives/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2228699&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Two bills moving through the state Senate seek to prevent immigration enforcement officers from isolating patients from their loved ones and interfering with their ability to get legal help. Analyses for both bills cite reporting by čŅ╣¾Õ·┤½├ĮęĢŅl Health News that found family members and attorneys have faced extreme difficulty locating and supporting patients hospitalized while in immigration custody.
čŅ╣¾Õ·┤½├ĮęĢŅl Health News found that some hospitals have facilitated patient isolation through what are known as blackout policies, which can include registering people under pseudonyms, withholding their names from the hospital directory, and preventing staff from contacting patients’ relatives to let them know their location and condition.
A bill by Democratic state Sen. Caroline Menjivar of the San Fernando Valley, , would largely prohibit the use of blackout policies for patients in immigration custody and ensure they retain the right to have their families and others notified of their whereabouts and condition. Blackout policies would be allowed when the health care provider determines the patient is a credible risk to themself or others and the risk is documented in the patient’s medical record. Patients would also be allowed to receive visitors.
It seeks to address reports of Immigration and Customs Enforcement agents guarding patients in their hospital rooms while they undergo medical exams or talk with doctors, interfering with medical decisions, and pushing for patients to be discharged prematurely to detention facilities ill-equipped to provide follow-up care.
“These are actions that have no place in health care, and it is a clear violation of the patients’ rights,” Menjivar said.
Under Menjivar’s proposal, agents would not be allowed into the rooms of patients they bring in for care unless they can show legal authorization to be there. If agents remain in the room, staff would be required to ask them to leave during medical exams and patient care discussions. If agents refuse, health care facility staff would need to document it.
, authored by state Sen. Susan Rubio, a Democrat from the San Gabriel Valley, would require health care providers to inform staff and relevant volunteers to respond when patients want their families to know where they are, and to post a notice at facility entrances with information about visitation and access policies. The law already says patients can agree to have loved ones notified they’re in the hospital, and Rubio’s bill seeks to make sure staff and others know they can do that for patients in immigration custody.
The federal Department of Homeland Security, which oversees immigration enforcement, did not respond to a request for comment.
Both bills were passed by the Senate Health and Judiciary committees along party lines and will be heard next by the Senate Appropriations Committee.
More than 20 immigrant rights advocates and health care workers voiced support for strengthened protections for patients at a hearing last week.
“This state must do everything in its power to protect against these abuses and ensure detainees have the right to contact their loved ones when they are hospitalized and in critical conditions,” said Hector Pereyra, political manager with the Inland Coalition for Immigrant Justice.
However, representatives from the California Hospital Association and California Medical Association told lawmakers last week they had concerns that directing health care workers to document agents’ badge numbers and ask them to leave patients’ rooms could create conflict and pose a safety risk.
“While we understand that this is an important issue, we want to ensure the bill strikes the right balance and does not create conflicting or unclear obligations for hospitals and their staff and clinicians, particularly in real-time interactions with federal officers,” said Vanessa Gonzalez, a vice president of state advocacy for the hospital association.
čŅ╣¾Õ·┤½├ĮęĢŅl Health News reported that one man, 43-year-old Julio César Peña, was held at a hospital in Victorville for almost two weeks before his attorney and family found out where he was. Peña, who had terminal kidney disease, was shackled to his hospital bed, guarded by immigration agents, and told he wasn’t allowed to disclose his location, according to his wife. He then suffered a seizure that left him intubated and unconscious, but no one notified his family. Peña died Feb. 25, less than two months after he was released to go home.
Advocates for immigrants and health care workers, as well as lawmakers, fear similar incidents are happening around the state.
Menjivar said her bill “seeks to close the gap between existing law and practice by empowering health care provider entities with the tools to uphold the privacy, health, and visitation rights of a patient brought in under immigration custody.”
SB 915 would prohibit hospitals and clinics from allowing immigration officers to make medical decisions for the patient or provide interpretation. Health care facilities would be required to document and verify, “to the extent possible,” the identities of immigration officers; provide patients access to communication tools; and inform patients of their rights. They would also need to complete discharge planning that includes attempts to coordinate with any receiving facility, such as a detention center, to ensure patients receive follow-up care.
The bills come on the heels of legislation passed last year that sought to limit immigration enforcement at health care facilities, including by prohibiting medical establishments from allowing federal agents without a valid search warrant or court order into private areas. However, that bill did not address situations in which patients are already in immigration custody.
“ICE has instilled fear in our hospitals and has kept us from doing our job,” said SatKartar Khalsa, an emergency medicine resident at a safety net hospital in San Francisco who has treated detained patients and testified in support of SB 915. “This has all led to worse care for our patients and has added another layer of fear among health care workers.”
čŅ╣¾Õ·┤½├ĮęĢŅl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFŌĆöan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-industry/ice-custody-immigrant-patient-protection-california-legislation/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2229421&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>But officials warned that all optional Medicaid services are still under review as the state health department looks for cuts to offset a shortfall driven by higher-than-expected Medicaid costs.
Jon Ebelt, a spokesperson with the Montana Department of Public Health and Human Services, said the agency is preparing a request to the federal government to add doula care to the state’s Medicaid program. It would cost the state about $118,000 in its first year to provide doula Medicaid reimbursements, according to .
His April 15 comments came three weeks after department officials told čŅ╣¾Õ·┤½├ĮęĢŅl Health News that the state budget deficit had put those plans on hold. Ebelt denied that a final decision had been made in March to scrap the doula Medicaid payments, which state lawmakers approved in a bill last year. The coverage is “now proceeding as planned,” he said.
“At the time of your initial inquiry, we were still in the process of analyzing the appropriation,” Ebelt said.
Federal health officials must approve any amendments to the state’s Medicaid program before payments can begin. reimburse doulas through Medicaid.
Doulas are trained, nonmedical workers who support people through pregnancy and after they give birth. The care they provide is in health complications, which has prompted more states to cover doula services in recent years.
Montana lawmakers who supported expanding Medicaid to cover doula care in 2025 cited scarce maternity services, especially in rural and Indigenous communities. But this year, the state has a Medicaid budget deficit of more than and is expecting a similar shortfall next year. Plus, federal policy changes slated to take effect later this year are expected to increase costs.
“ŌĆŖThere’s a need and a desire for doula services, but a lot of people can’t afford it,” said Sheri Walker, a Helena-based doula and president of the . “So that means many of us have other jobs that we have to juggle.”
Walker is a part-time labor and delivery nurse outside of her doula work.
On March 25, health department spokesperson Holly Matkin said in an email to čŅ╣¾Õ·┤½├ĮęĢŅl Health News that the agency “will not be moving forward with the implementation of doula services in the Montana Medicaid benefit package at this time.” She had added that it was unclear whether state law gives the department the authority to authorize coverage during the budget shortfall.
State Sen. , a Democrat who sponsored last year’s bipartisan doula reimbursement bill, said she didn’t know about the department’s plans until she saw čŅ╣¾Õ·┤½├ĮęĢŅl Health News’ reporting. Neumann said she and groups that had backed the legislation began calling health officials, making the case for doula services as a low-cost way to provide critical care.
After about a week, Neumann said, state officials told her the agency was moving ahead with doula services after all.
“They were on the chopping block,” Neumann said. “This is a story of how important it is for all Montanans to pay attention and stay connected to what’s happening.”
Ebelt did not clarify what led the department to change its position. However, he warned that optional Medicaid services, such as doula services, may still be cut.
“All optional services, including this service, are being reviewed,” Ebelt said, referring to doula care. He did not respond to a follow-up query as to whether the department might still decide to postpone the program following federal approval.
are types of care that states choose to cover through their Medicaid programs but aren’t required by federal law. That can include covering eyeglasses, prescription drugs, and prosthetics, and more specialized care such as physical therapy, or inpatient psychiatric services for people under 21.
Those services may not sound optional, said , who studies Medicaid financing at KFF, a health information nonprofit that includes čŅ╣¾Õ·┤½├ĮęĢŅl Health News. But she said they’re one of the few avenues states have to make adjustments when budgets get tight.
Congressional Republicans’ One Big Beautiful Bill Act, the spending measure President Donald Trump signed into law last July, is expected to put more states in a budget crunch as its provisions start to take effect by the end of the year. The federal government has estimated that the law will reduce federal Medicaid spending by nearly $1 trillion over 10 years. The law also left states with a higher share of the costs to provide food assistance.
Williams said many states expanded services in recent years by boosting optional Medicaid benefits and provider pay.
“We could see them walk those back,” Williams said.
Montana’s financial problems preceded federal changes. Last year, state lawmakers cut some of the health department’s funding and underestimated Medicaid use. The state also overestimated what the federal government would pay toward Montana’s Medicaid costs.
Health officials must outline a plan to cut costs before the state’s 2027 budget year begins on July 1. Simultaneously, the agency is trying to hire more staffers to begin vetting whether Medicaid enrollees meet or are exempt from new work requirements that also go in place July 1. The new rules, mandated through long-delayed state legislation and the federal spending law, will have a three-month grace period.
Stephanie Morton, executive director of , said she’s grateful the state is back on track to pay for doula services through Medicaid. But she said she’s worried about potential health care cuts to come.
“We know that doulas are a critical piece of that infrastructure, but standing alone and losing other sources of care really isn’t optimal,” Morton said. “These are not robust systems as it stands.”
čŅ╣¾Õ·┤½├ĮęĢŅl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFŌĆöan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/medicaid/doula-care-pregnancy-medicaid-montana-budget-cuts/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2229052&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>McLeod, who lives near Charleston, South Carolina, is still paying off chemotherapy bills that followed her 2017 diagnosis. She also now faces an onslaught of out-of-pocket costs for follow-up monitoring and care, including regular visits to a pulmonologist and allergist.
McLeod, 45, said she had already spent $2,500 in the first two months of the year and owes an additional $1,300 from a January colonoscopy. That’s on top of the $895 monthly premium for a health insurance plan that covers her family of six.
Those costs have led McLeod to ration her other care. Despite feeling intense chest pain since February, for example, she is putting off a CT scan and a visit to a heart specialist.
“You’re forced to pick and choose as to where your priorities really need to be,” said McLeod, director of strategic programs and partnerships at the Cancer Hope Network, a nonprofit that supports cancer patients. Even in that role, she struggles to navigate the financial aftermath of surviving the disease.
The cost of postcancer care often “keeps us hostage,” she said.
McLeod is one of nearly 19 million U.S. cancer survivors, many of whom continue to need prescriptions, doctor visits, and procedures to monitor their condition and manage posttreatment side effects. Of more than 1,200 cancer patients and survivors , about 47% said they had carried medical debt, with nearly half having owed more than $5,000, according to the American Cancer Society Cancer Action Network.

Yet health policy researchers and patient advocates said the experiences of cancer survivors reveal the limits of the Trump administration’s proposals to lower premiums, which may not help patients who accumulate large medical bills year after year. The proposals center on increasing the availability of high-deductible health plans, which have lower monthly payments but require patients to pay thousands of dollars out-of-pocket before coverage kicks in.
In addition, the administration has supported allowing insurers more leeway to sell plans that are not compliant with the Affordable Care Act. Such plans could bar people who have preexisting health conditions, like a cancer diagnosis, and exclude that ACA plans are required to cover.
The administration did not answer a request for comment on how its proposals would affect cancer survivors. But its supporters say, in general, people would have more flexibility to personalize coverage and more options for plans with lower monthly fees.
Michael Cannon, director of health policy studies at the Cato Institute, a libertarian think tank, believes patients would have better control over spending, and the option to choose what kind of care gets covered, if health plans were exempted from the ACA’s regulations. A person could opt for a plan that includes cancer treatment but not maternity care, for example.
History proves insurance coverage is not that simple, especially for people with preexisting conditions, said Jennifer Hoque, an associate policy principal with the American Cancer Society Cancer Action Network. When health plans could “pick and choose” enrollees based on preexisting conditions prior to the ACA, people needing the costliest care often struggled to find coverage, she said.
“They’re not going to choose a cancer survivor,” Hoque said of health insurers.
That was the case for Veronika Panagiotou, who said private insurers refused her coverage back in September 2013 because she had a high body mass index. Two months later, as a 25-year-old uninsured graduate student, she was diagnosed with non-Hodgkin lymphoma. The hospital treated her, she recalled, “and sent me all the bills.”
In January 2014, Panagiotou was able to buy one of the first ACA plans that went into effect. It covered chemotherapy and immunotherapy treatment, imaging, medications, hospital stays, weekly blood draws, a blood transfusion, and emergency room visits.
Now Panagiotou, 37, is cancer-free and works as director of advocacy and programs at Cancer Nation, a nonprofit advocacy group. Even though she is covered through her employer, Panagiotou said treatment-related expenses weigh heavily on her life decisions.
“Every choice I make, I think about cancer,” she said.

Chris Bond, a spokesperson for AHIP, the main health insurance trade association, said its members are working to improve access to coverage. But that can be a challenge when doctors and drugmakers are hiking prices, he said. Health plans are trying to “shield Americans from the full impact of those rising costs,” Bond said.
The Lymphoma Research Foundation has seen a 10% increase in applications to its patient aid fund this year, CEO Meghan Gutierrez said. “This trajectory suggests that financial safety nets, when they exist, are straining,” she said.
Rising prices are affecting everyone, regardless of the kind of health insurance they have, if any, said Brian Blase, president of Paragon Health Institute, a Republican-aligned think tank. “The biggest challenge for cancer patients isn’t the type of coverage,” he said. “It’s the underlying cost of care.”
Blase pointed to President Donald Trump’s as potentially helpful to cancer survivors. The Medicare Drug Price Negotiation Program, established by the Inflation Reduction Act of 2022, required the Department of Health and Human Services to negotiate prices for certain high-cost drugs, to lower prices for the federal health insurance program for people ages 65 and older. Drugs for breast, prostate, and kidney cancers are already on that list, .
Yet Hoque fears efforts to weaken ACA protections and financial support for marketplace plans will give cancer survivors ŌĆö who she said tend to “hang on to insurance for dear life” ŌĆö fewer options, especially between jobs or during career changes.
Erin Jones, a 31-year-old food policy researcher living in Fort Collins, Colorado, who was diagnosed with Hodgkin lymphoma as a young adult, is now cancer-free but still sees two oncologists, visits a high-risk breast clinic, and gets a breast MRI annually. Jones gets health insurance through the university where she works, and said she recently deferred acceptance to a PhD program partly due to uncertainty over affordable coverage.
“I don’t have the freedom to do the things I want to do as easily,” she said, “because I am constantly worried about health insurance.”
Costs related to surviving cancer, including monitoring for recurrence and treatment of side effects, were expected to reach $246 billion by 2030, up from $183 billion in 2015, according to .
Advancements in both detecting and curing cancer have resulted in a higher percentage of people surviving five years or more after diagnosis, according to the American Cancer Society. The number of survivors is expected to grow to more than 22 million people by 2035, .
Despite these advancements, the cost of treatment can steal the spotlight, said Ezekiel Emanuel, a co-director of the Healthcare Transformation Institute at the University of Pennsylvania and a onetime health policy adviser to former President Barack Obama.
An oncologist, Emanuel said he had observed patients make the difficult decision to delay or skip postcancer care as a result.
“Even when we triumph,” he said, “we don’t seem to be able to have a celebration.”
Are you struggling to afford your health insurance? Have you decided to forgo coverage? Click hereŌĆ»to contact čŅ╣¾Õ·┤½├ĮęĢŅl Health News and share your story.
čŅ╣¾Õ·┤½├ĮęĢŅl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFŌĆöan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-care-costs/cancer-survival-costs-testing-treatment-premiums-deductibles-trump/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2229400&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>
April 16
Katheryn Houghton reads the week’s news: Many Americans say it’s hard to pay for the dentist, but putting off care also has its costs. Plus, for some patients, Medicare will start covering GLP-1 drugs for weight loss this year.
April 9
Zach Dyer reads the week’s news: Rising health costs have some middle-aged adults skipping the doctor until Medicare will pick up the tab. Plus, there’s little evidence that immigrants without legal status are using Medicaid, despite White House claims.
April 2
Arielle Zionts reads the week’s news: Scientists say staff losses at the National Institutes of Health could lead to fewer medical breakthroughs. Plus, doctors worry they’ll see more kids with potentially deadly complications from measles, as cases surge.
March 26
Jackie Fortiér reads the week’s news: Consumers know which party they blame after Congress failed to extend enhanced Obamacare subsidies. Plus, updated standards say seniors should aim for even lower blood pressure readings.
March 19
Sam Whitehead reads the week’s news: Amid federal spending cuts and suspicion of fluoride, tooth problems are sending more kids to the ER. Plus, patients look to health savings accounts to deal with rising medical costs.
March 12
Katheryn Houghton reads the week’s news: Looming Medicaid cuts could mean states stop covering dental care for adults, and a growing number of U.S. nurses are moving to Canada.
March 5
Zach Dyer reads the week’s news: The Trump administration is calling for sharp restrictions on direct-to-consumer drug ads, and for some people facing skyrocketing health insurance costs, becoming eligible for Medicare because of a new diagnosis is a terrible irony.
Feb. 26
Sam Whitehead reads the week’s news: Some places are bringing back house calls to try to fight maternal and infant mortality, and almost all Americans benefit from health care subsidies in different forms.
Feb. 19
Arielle Zionts reads the week’s news: Some health systems are using AI tools to help patients get primary care, and the Trump administration’s new data-sharing rules make going to the hospital more dangerous for people without legal status.
Feb. 12
Jackie Fortiér reads the week’s news: Moves by the Trump administration have slowed cancer research, and more of America’s doctors are working into their golden years.
Feb. 5
Katheryn Houghton reads the week’s news: American farmers are being hit hard by the end of extra Obamacare subsidies, and hospitals are starting their own Medicare Advantage plans.
Jan. 29
Zach Dyer reads this week’s news: An expensive new gene therapy that can potentially cure people with sickle cell disease will be covered by Medicaid, but only when it works for patients. Plus, community health centers are preparing to help care for millions more uninsured people.
Jan. 22
Arielle Zionts reads the week’s news: Some states are cutting public funding for a type of autism therapy, and older adults are more likely than younger ones to stop taking GLP-1 drugs such as Ozempic.
Jan. 15
Jackie Fortiér reads the week’s news: Parents are confused by an overhaul of U.S. childhood immunization guidelines, and while people 65 and older make up the fastest-growing homeless population in the country, traditional homeless shelters often can’t accommodate them.
Jan. 8
Zach Dyer reads the week’s news: Instead of extending extra Affordable Care Act subsidies that would keep monthly premiums more affordable, some Republicans are pushing health savings accounts. Plus, people seeking cheaper health insurance options outside the ACA marketplaces may find some, but they come with downsides.
Jan. 1
Katheryn Houghton reads the week’s news: AI voices can help patients who have had their voice boxes removed sound like themselves again, and many state-run psychiatric hospitals don’t have enough beds to treat patients unless they’ve been charged with a crime.
The čŅ╣¾Õ·┤½├ĮęĢŅl Health News Minute is available every Thursday on CBS News Radio.
čŅ╣¾Õ·┤½├ĮęĢŅl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFŌĆöan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/news/listen-to-the-latest-kff-health-news-minute-2026/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2138213&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>The lawsuit, settled on confidential terms last year, blamed not only the managers of City Creek Post-Acute and Assisted Living but also the building’s owner, a real estate investment trust, or REIT.
In the year Darby died, City Creek paid CareTrust REIT more than $1 million in rent, while the Sacramento, California, nursing home ran a deficit, court records show.
Federal tax rules ban REITs from running health care facilities, but CareTrust was not an absentee landlord either, according to internal records filed in the case. It chose the nursing home’s management company and required through the lease that the home keep at least 80% of beds occupied. CareTrust granularly tracked how well the home kept to its financial plan, down to the money spent monthly on nurses and food, the records said. And the documents showed that the real estate company kept tabs on government safety inspection findings and Medicare quality ratings.

Both CareTrust and the nursing home operator denied liability for Darby’s death. CareTrust officials said in court papers that it is not involved in day-to-day nursing home decisions or patient care, and that it monitors facilities to ensure nothing jeopardizes rent payments. In a written statement, CareTrust Corporate Counsel Joseph Layne told čŅ╣¾Õ·┤½├ĮęĢŅl Health News: “We are the property owners, not the operators.”
Landlords With Influence
Over the past decade, real estate investment trusts have bought thousands of buildings that house nursing homes, hospitals, assisted living facilities, and medical offices. A čŅ╣¾Õ·┤½├ĮęĢŅl Health News examination of court filings and corporate records shows that these landlords have more influence than the health care facilities publicly acknowledge.
The documents reveal REITs often select the management who oversee the operations and leave them in place even when they are aware of threadbare staffing, floundering governance, repeated safety violations, or other problems that hamper quality of care. A California jury in March awarded $92 million in punitive damages against a former REIT over the death of a 100-year-old resident with dementia who froze to death outside her assisted living facility.
“The REITs are in charge,” said Laraclay Parker, one of the lawyers who represent Darby’s daughter.
Absence of Oversight
Despite their ubiquity, REITs remain invisible to state and federal health regulators. Hospitals and nursing homes are not required to disclose rent payments or landlord identities in the annual reports they submit to Medicare.
Under President Donald Trump, the Centers for Medicare & Medicaid Services a Biden-era requirement that nursing homes . Catherine Howden, a CMS spokesperson, said in a statement that the agency does not regulate facilities based on their tax status or corporate form and instead focuses on the quality of the care they provide.
REITs now of the nation’s senior housing, which includes assisted living, memory care, and independent living, according to an industry analysis. REITs also hold investments in nursing homes. Publicly traded REITs that focus on health care are now worth nearly a quarter of a trillion dollars, according to Nareit, an industry association.
čŅ╣¾Õ·┤½├ĮęĢŅl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFŌĆöan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-industry/real-estate-investment-trusts-senior-housing-nursing-homes-profit/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2228343&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>After some federal financial aid expired, many Americans found that high-deductible health plans were the only option they could afford.
In a new episode of NPR’s Life Kit podcast, čŅ╣¾Õ·┤½├ĮęĢŅl Health News reporter Jackie Fortiér and podcast host Marielle Segarra discuss what these plans are, and why they can feel so confusing. Imagine paying $100 out-of-pocket for a routine doctor visit that used to cost you $20. Imagine shouldering thousands of dollars in bills before your insurance pays a cent.
Still, for some people ŌĆö especially those who rarely need medical care ŌĆö high-deductible plans work. Listen to the episode to explore how timing your care and taking advantage of free preventive services can help you make the most of your coverage.
čŅ╣¾Õ·┤½├ĮęĢŅl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFŌĆöan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/insurance/listen-health-care-helpline-life-kit-high-deductible-plans-out-of-pocket-costs/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2228954&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>The Office of Personnel Management 65 insurance companies to provide monthly reports with detailed medical and pharmaceutical claims data of more than 8 million people enrolled in federal health plans, čŅ╣¾Õ·┤½├ĮęĢŅl Health News reported earlier this month. The request, which could dramatically expand the personally identifiable medical information OPM can access, alarmed health ethicists, insurance company executives, and privacy advocates.
Now, OPM Director Scott Kupor has two letters on his desk ŌĆö one from 16 U.S. senators and another led by Rep. Robert Garcia, the top Democrat on the House Oversight Committee ŌĆö asking him to drop the agency’s proposal.
“The collection of broad, personally identifiable data regarding medical care and treatment raises concerns that OPM could target certain federal employees seeking vital health care services that the Administration disagrees with on political grounds,” the Democratic House members , citing čŅ╣¾Õ·┤½├ĮęĢŅl Health News.
The letters from congressional Democrats alone are unlikely to reverse OPM’s plans. Republicans ŌĆö who control Congress and, ultimately, any oversight activities ŌĆö have not weighed in on OPM’s notice.
OPM did not immediately respond to a request for comment on the letters. The agency, which said in its notice that it will use the data for oversight and to manage the federal health plans, has not publicly addressed written concerns about its proposal.
The notice, posted and sent to insurers in December, states that insurers are legally permitted to disclose “protected health information” to OPM and does not provide instructions to redact identifying information, such as names or diagnoses, from the claims.
That data could be used to implement cost-saving measures, health policy experts told čŅ╣¾Õ·┤½├ĮęĢŅl Health News earlier this month. But it would also give the Trump administration ŌĆö which has laid off or fired tens of thousands of federal workers ŌĆö access to a vast trove of personal information.
In the letters, Democratic lawmakers lay out a number of concerns about potential consequences of OPM’s obtaining detailed medical claims for millions of federal workers.
The ŌĆö led by Adam Schiff of California and Mark Warner of Virginia ŌĆö argues that OPM is not equipped to safeguard such sensitive data and that the administration could share the records across government agencies, as it has done with personal information on millions of Medicaid enrollees.
They also assert that the agency does not have a legal right to the data and that insurers’ sharing the information with OPM would “violate the core principles of the Health Insurance Portability and Accountability Act.” HIPAA requires certain organizations that maintain identifiable health information ŌĆö such as hospitals and insurers ŌĆö to protect it from being disclosed without patient consent. The proposal, the senators warn, threatens patients’ relationships with their clinicians, especially “sensitive disclosures regarding mental health, chronic illness, or other deeply personal conditions.”
“For these reasons, we strongly urge you to cease any further consideration of this proposal,” states the letter, which was sent to Kupor on April 19.
The American Federation of Government Employees, the largest union for federal employees, to čŅ╣¾Õ·┤½├ĮęĢŅl Health News’ reporting. The union noted in a statement from its national president, Everett Kelley, that OPM’s proposal “comes in the context of coordinated attacks on federal employees and repeated stretching of the legal boundaries for sharing sensitive personal data across government agencies.
“The question of what this administration intends to do with eight million Americans’ most private health information is not academic,” the AFGE statement read. “It is urgent.”
In an emailed statement, Kelley applauded the congressional letters.
“We are pleased that Democratic lawmakers on the Hill are just as outraged as we are over this administration’s blatant attempt to breach the privacy of millions of Americans across the country,” Kelley wrote. “We share their concerns regarding potential misuse of the information to continue illegally targeting workers and their demand for OPM to withdraw this proposal.”
čŅ╣¾Õ·┤½├ĮęĢŅl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFŌĆöan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-industry/opm-federal-workers-health-records-hipaa-democratic-letters/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2228955&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>But physicians, dentists, ambulance companies, and other health care providers are still taking their patients to court, a Connecticut Mirror-čŅ╣¾Õ·┤½├ĮęĢŅl Health News investigation of state legal records shows.
Lawsuits by doctors and other nonhospital providers now dominate health care collections in Connecticut, the records show, accounting for more than 80% of cases filed against patients and their families in 2024.
That’s a major reversal from just five years earlier, when hospital system lawsuits made up three-quarters of health-related collection cases in the state’s courts.
The shift is moving medical debt collections into a less regulated realm. Most hospitals, because they are tax-exempt nonprofits, must make financial aid available to low-income patients and follow federal regulations that limit aggressive collection activities. Other medical providers, such as private medical groups, are generally exempt from these rules.
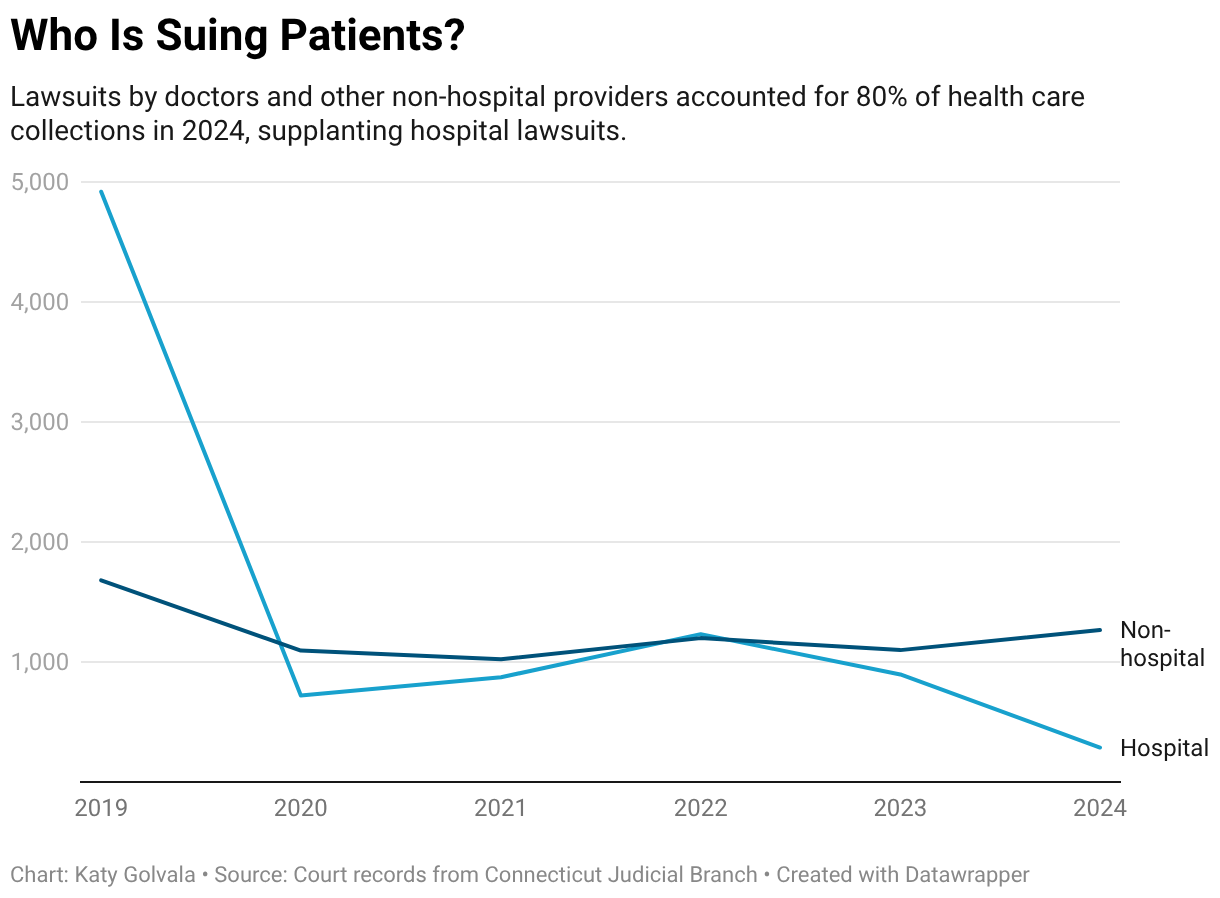
The lawsuits are typically over bills of less than $3,000, but the impact on patients can be devastating. Lawsuits are among the most ruinous byproducts of a health care debt problem that burdens an estimated 100 million people in the U.S.
Lawsuits can lead to garnished wages, liens on homes, and hundreds of dollars of added debt from interest and court fees. They also pile additional financial strains on struggling families, prevent patients from getting needed care, and sap trust in medical providers.
“It’s really messed up,” said Allie Cass-Wilson, a nurse in Bristol, Connecticut, who was sued over a $1,972 debt by an OB-GYN practice where she’d been a patient years earlier. “How can they do that to people?” She did not contest the lawsuit, court records show.
Cass-Wilson, who is 36 and lives in a small apartment just off an expressway on-ramp, said she learned of the outstanding debt only when she was sued. When she tried making an appointment, she said, she was told her doctor wouldn’t see her. “They said I was blacklisted,” Cass-Wilson said. “I was so confused. I couldn’t believe that my medical provider let my care be interrupted like this.”
Cass-Wilson ultimately sought medical care elsewhere.
Radiologists, Dentists, Ambulances
Overall, CT Mirror and čŅ╣¾Õ·┤½├ĮęĢŅl Health News identified more than 16,000 health care-related debt cases in Connecticut courts from 2019 to 2024. The database was assembled from online court records with the help of January Advisors, a data science consulting firm that helped extract and sort the data.
Over the six-year period, most of Connecticut’s more than 25,000 did not pursue patients in court for outstanding balances.
But records show that more than 400 medical providers, including several hospital systems, sued their patients. Among those filing lawsuits were radiologists, anesthesiologists, eye doctors, podiatrists, allergists, and pediatricians.
Dentists, periodontists, and other dental providers filed more than 1,000 lawsuits against patients. And ambulance companies sued more than 140 people.
Med-Aid, a company based outside New Haven, Connecticut, that provides orthopedic braces and other medical supplies to patients, sued more than 400 people, the court records show. The company’s president, Frank Dilieto, did not respond to repeated interview requests.
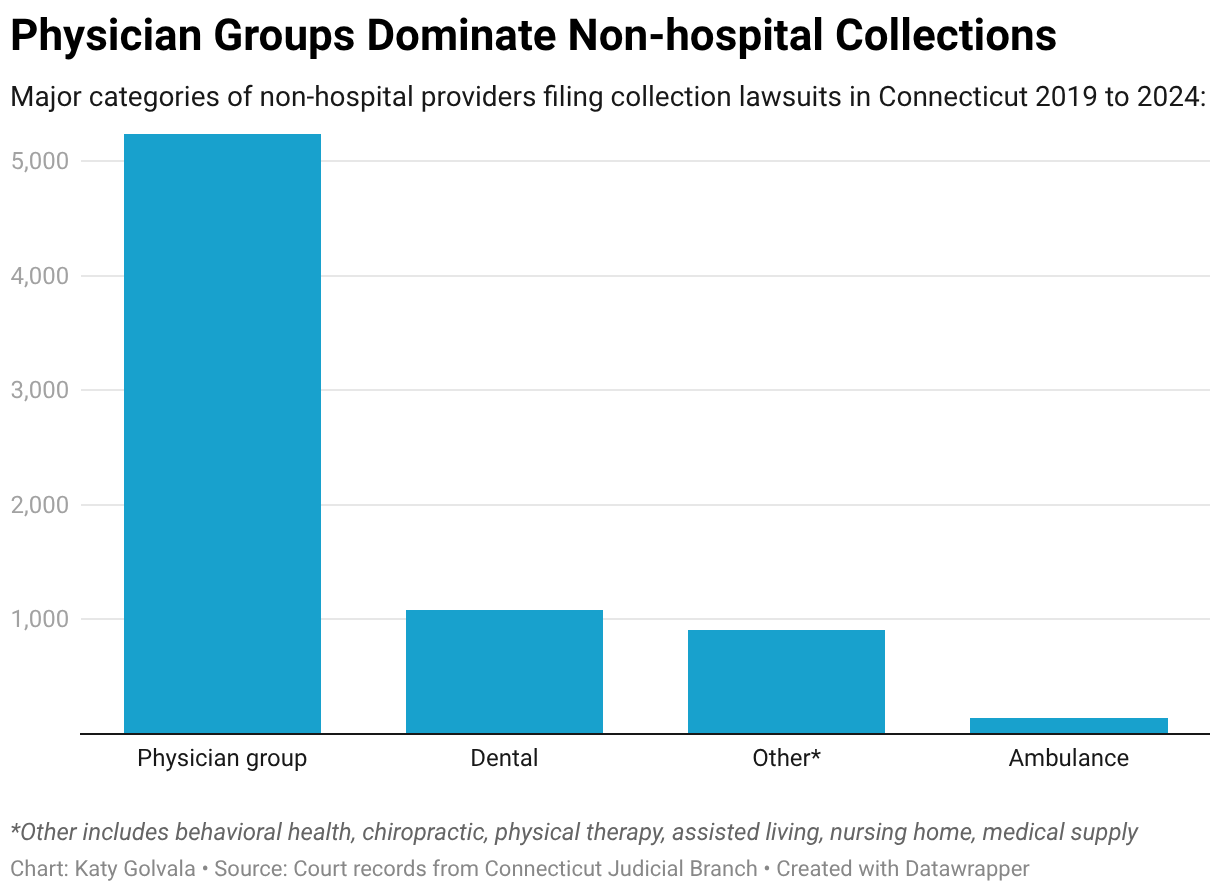
Cass-Wilson was sued by Briar Rose Network in Bristol, Connecticut, a member of a large network of OB-GYN practices across Connecticut called Physicians for Women’s Health. The network’s members sued close to 100 patients in 2024, records show.
Paula Greenberg, CEO of Women’s Health Connecticut, a private equity-backed company affiliated with Physicians for Women’s Health that manages business operations for the network, said the lawsuits represent a small fraction of the more than 300,000 patients the network sees every year.
“This is an organization committed to patients,” Greenberg said. She noted that the group offers options to help patients pay, including installment plans and financial aid.
Geoffrey Manton, president of Naugatuck Valley Radiological Associates, said his practice also will work with people who say they can’t pay. But, he said, patients sometimes stop responding to their bills.
“Hiding from your problems isn’t going to solve them,” Manton said. “If we didn’t take any action, there could be that person that is in that late-model Mercedes that just chooses not to pay any bills.” The group sued more than 125 patients from 2019 to 2024, according to the court records.
Many medical providers say that aggressive collections stem from the growing prevalence of high-deductible health plans that leave patients with thousands of dollars of bills before their coverage kicks in.
Greenberg and Manton said each of their physician groups must collect. “This is a business,” Greenberg said. “We have to look at our operating costs.”
Critics of medical collection lawsuits note that the patients are typically sued over relatively small debts that are likely to have little impact on multimillion-dollar medical practices.
The average patient debt that members of Physicians for Women’s Health sued over in 2024 was less than $1,100, court records show. The physician group’s annual revenues are typically in the tens of millions of dollars, according to Greenberg.
Even relatively small debts — which often include interest — can place substantial burdens on families struggling to keep up with their bills, especially while dealing with a serious illness, patient advocates say.
“We don’t have a realistic choice in using health care,” said Lisa Freeman, who heads the Connecticut Center for Patient Safety and has advocated for patients struggling with medical bills. “To then get sued for it, when people have less and less funds available for anything extra, that’s very disheartening.”
A Stroke, Then a Lawsuit

Matthew Millman, 54, lost his job as an IT support worker after having a stroke. Then Meriden Imaging Center sued him over an $1,891 bill.
Millman and his wife said they tried to explain their financial situation to the center, which is affiliated with Midstate Radiology Associates, a large physician group that operates imaging centers and doctors’ offices across Connecticut.
“It was very frustrating,” said Millman, who lives in an aging apartment owned by his wife’s family in New Britain. Millman, his wife, and their teenage daughter are barely getting by on his two part-time jobs — one bagging groceries, the other helping homebound seniors. Together, the jobs pay about $1,500 a month, he said.
The imaging center, after winning the collection case against Millman, tried to garnish his wages, though that was unsuccessful because Millman had lost his IT job.
“It’s all about money,” Millman said, shaking his head. “If you are trained in helping somebody with their health, it shouldn’t be about the money first. It should be about their health.”
Court records show that Midstate Radiology, Meriden Imaging Center and affiliates filed more than 1,000 collection lawsuits against patients from 2019 to 2024, making them the most litigious nonhospital providers in the state. As is common in medical debt lawsuits, the plaintiffs prevailed in most cases, records show.
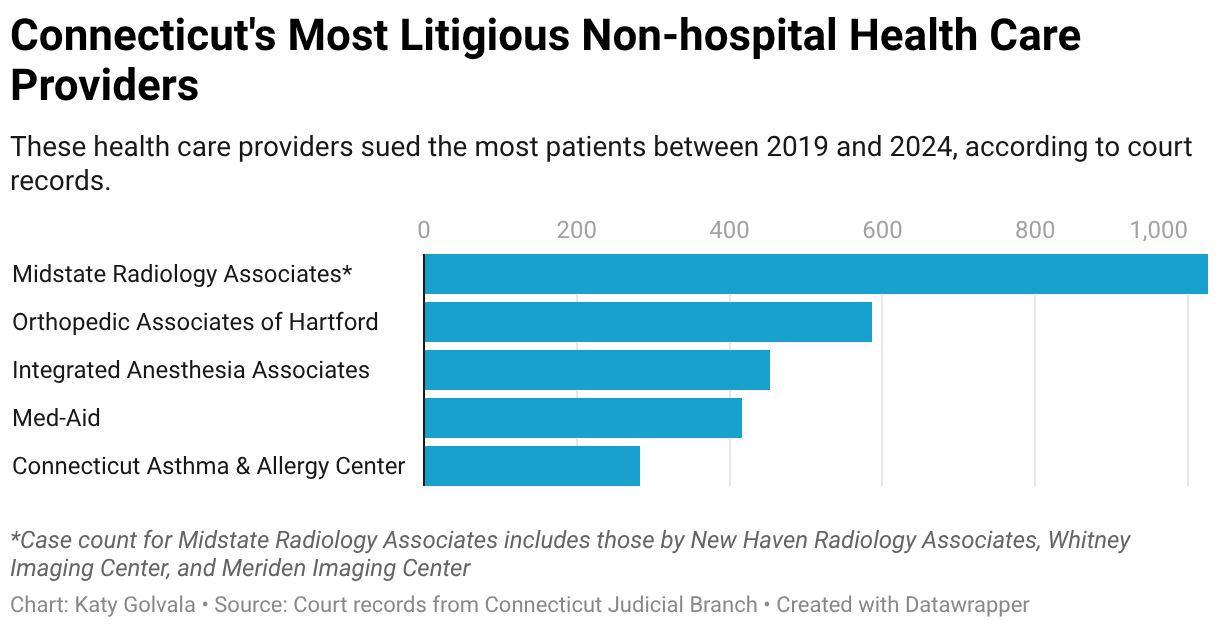
Midstate president Gary Dee, a radiologist, didn’t respond to emails and messages left at his West Hartford office.
Across town from Millman’s apartment in New Britain, Joseph Lentz lives in a cramped apartment with his wife and daughter. He used to oversee operations at a Boy Scout camp but is now unemployed. Lentz lost his job during the pandemic. The family home went into foreclosure, he said.
In 2023, Orthopedic Associates of Hartford sued Lentz over a $3,644 bill the practice said he owed after having shoulder surgery in 2018.
“I’d pay it if I could, I guess,” said Lentz, 59. “But I don’t even know where next month’s rent is coming from. I’m trying to climb out as best I can. I guess this is just one more thing to shovel in.”
The orthopedic group filed more than 580 lawsuits against patients from 2019 to 2024, prevailing in most, records show.
The medical group declined interview requests. But chief executive David Mudano said in a statement: “As an independent physician practice, we strive to balance compassion for patients with the financial responsibility required to sustain our practice.”
Old Debts and Disputed Claims
Lentz, who did not contest the lawsuit, said he has no reason to doubt he owes the debt. But in many cases reviewed by CT Mirror and čŅ╣¾Õ·┤½├ĮęĢŅl Health News and in interviews, patients being sued questioned the accuracy of their medical bills, citing care they thought health insurance should have covered or, in some cases, bills for services they never received.
This reflects with aggressive collection tactics like lawsuits when disputes over the accuracy of medical bills and delayed or denied insurance claims are so widespread in American health care.
A by the federal Consumer Financial Protection Bureau found that nearly half of the medical debt complaints fielded by the agency involved bills that consumers said were erroneous in some way or that consumers said they’d already paid.
“We know people are billed incorrectly,” said Lester Bird, who studies debt collection lawsuits at the nonprofit Pew Charitable Trusts. Bird noted that courts are ill equipped to sort through disputed medical charges or insurance claims, especially when there is little documentation in most debt collection lawsuits.
“It’s complicated before it gets to the courts,” Bird said, “and it’s very complicated when it gets into the courts.”
This can create headaches for physicians and other providers. But billing problems ultimately affect patients and their families most, said Connecticut state Sen. Saud Anwar, a Democrat who is also a physician. “Patients are left to deal with it.”
Andrew Skolnick, an attorney in Milford, outside New Haven, was sued in 2023 by an imaging center where his wife had received services in 2020.
Skolnick said that when the couple, who were covered through his job-based insurance, originally received the bill from Diagnostic Imaging of Milford, he tried to tell the imaging center it had submitted the claim to the wrong insurance plan, but he said they wouldn’t speak with him.
The center later filed the lawsuit, alleging he owed more than $2,000, plus almost $300 in interest.
Despite interview requests, officials at Diagnostic Imaging of Milford did not comment for this article.
Unlike most patients who are sued, Skolnick had the resources and expertise to contest the suit. He said he offered to pay what would have been his responsibility under the plan if the imaging center had filed his claim correctly. He ultimately settled for $1,700, court records show.
“It wasn’t a tremendous amount, but I knew that they had made a mistake,” Skolnick said. “The system is not working.”
More Protections?
Anwar, the state lawmaker and physician, expressed concern that lawsuits undermine patients’ faith in their doctors.
“It’s a sacred relationship,” he said. “If your physician, who is taking care of you, is suing you for money, that’s a problem.
Many hospitals, facing bad publicity from suing patients, have stopped taking patients to court over unpaid bills. Hospital collection lawsuits identified by CT Mirror and čŅ╣¾Õ·┤½├ĮęĢŅl Health News in Connecticut court records plunged from more than 4,900 in 2019 to fewer than 300 in 2024.
Also, in recent years, several states, including Connecticut, have expanded protections for patients with bills they can’t pay.
Connecticut now from consumer credit reports, and legislators are pushing to get hospitals to provide more financial aid to patients. Other states have restricted the use of wage garnishment and property liens to collect medical debt.
But state efforts to rein in aggressive medical debt collections have mostly focused on hospitals. That may need to change, said Connecticut state Sen. Matt Lesser, a Democrat who co-chairs the legislature’s Human Services Committee.
He is a key backer of a bill that would bar hospitals from billing patients who receive public benefits like food assistance or who make less than twice the federal poverty level, about $32,000 for an individual.
The restriction would not apply to bills from physicians and other nonhospital providers, however. “We may have to go bigger if that’s where the heart of the matter is,” Lesser said.
Connecticut Gov. Ned Lamont, a Democrat who spearheaded an initiative to for more than 150,000 state residents, also expressed concern about physicians suing the people in their care.
“Everyone should do the right thing by patients,” he said.
This article was produced in partnership with , a statewide nonprofit newsroom that covers public policy and politics.
How We Did It: Analyzing Connecticut Health Care Debt Collection Lawsuits
How often do health care providers sue patients over unpaid bills?
In most states, that’s nearly impossible to answer because courts don’t typically identify which debt collection lawsuits involve a medical debt versus other kinds of debt, such as rent, credit cards, or cellphone bills.
But Connecticut is different. Debt collection cases filed in small-claims court for unpaid medical or dental bills must be classified as health care debt. We worked with the data science consulting firm January Advisors to pull these cases from the Connecticut court database and analyze them. (January Advisors has worked with nonprofits and researchers across the country to collect debt collection data from state courts. The firm did not have any editorial input in our project.)
We started with health care collection cases filed in small-claims court from 2019 to 2024. But this covered only cases involving debts smaller than $5,000. We also wanted to know about cases in which providers sued for bills exceeding $5,000. Connecticut courts don’t assign a “medical” category for large-claim cases. So we pulled all large-claim records for any plaintiff — hospital or nonhospital provider — that appeared in medical small-claims cases. We also included cases with plaintiffs that didn’t appear in that dataset but had common medical terminology in their names, like “hospital” or “DDS.”
We then went through each case manually to confirm that the plaintiff was a medical or dental provider. We determined whether the provider was part of a larger hospital or physician group. And we categorized each plaintiff by a provider type (e.g., hospital system, dental, physician group).
In some cases, the data we pulled was incomplete, so we looked up the court records online and manually entered the information into our database. The Connecticut Judicial Department purges case records from its online portal after a certain amount of time. In those cases, we asked the agency to provide summonses and claims so we could manually enter the case information into our database.
We removed cases with out-of-state defendants or out-of-state plaintiffs and any cases in which missing records made it difficult to confirm information about the provider.
This <a target="_blank" href="/news/medical-debt-connecticut-doctors-sue-patients/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2228622&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>


