The Powerful Constraints on Medical Care in Catholic Hospitals Across America
Nurse midwife Beverly Maldonado recalls a pregnant woman arriving at Ascension Saint Agnes Hospital in Maryland after her water broke. It was weeks before the baby would have any chance of survival, and the patientโs wishes were clear, she recalled: โWhy am I staying pregnant then? Whatโs the point?โ the patient pleaded.
But the doctors couldnโt intervene, she said. The fetus still had a heartbeat and it was a Catholic hospital, subject to the โ for Catholic Health Care Servicesโ that prohibit or limit procedures like abortion that the church deems โimmoralโ or โintrinsically evil,โ according to its interpretation of the Bible.
โI remember asking the doctors. And they were like, โWell, the baby still has a heartbeat. We canโt do anything,โโ said Maldonado, now working as a nurse midwife in California, who asked them: “What do you mean we canโt do anything? This babyโs not going to survive.โ
The woman was hospitalized for days before going into labor, Maldonado said, and the baby died.
Ascension declined to comment for this article.
The Catholic Churchโs directives are often at odds with accepted medical standards, especially in areas of reproductive health, according to physicians and other medical practitioners.
The American College of Obstetricians and Gynecologistsโ for managing pre-labor rupture of membranes, in which a patientโs water breaks before labor begins, state that women should be offered options, including ending the pregnancy.
Maldonado felt her patient made her wishes clear.
โUnder the ideal medical practice, that patient should be helped to obtain an appropriate method of terminating the pregnancy,โ said Christian Pettker, a professor of obstetrics, gynecology, and reproductive sciences at the Yale School of Medicine, who helped author the guidelines.
He said, โIt would be perfectly medically appropriate to do a termination of pregnancy before the cessation of cardiac activity, to avoid the health risks to the pregnant person.โ
โPatients are being turned away from necessary care,โ said Jennifer Chin, an OB-GYN at UW Medicine in Seattle, because of the โemphasis on these ethical and religious directives.โ
They can be a powerful constraint on the care that patients receive at Catholic hospitals, whether emergency treatment when a womanโs health is at risk, or access to birth control and abortions.

More and more women are running into barriers to obtaining care as Catholic health systems have aggressively acquired secular hospitals in much of the country. Four of the 10 largest U.S. hospital chains by number of beds are Catholic, according to federal data from the Agency for Healthcare Research and Quality. There are just over 600 Catholic general hospitals nationally and roughly 100 more managed by Catholic chains that place some religious limits on care, a ั๎น๓ๅ๚ดซรฝา๎l Health News investigation reveals.
Maldonadoโs experience in Maryland came just months before the Supreme Courtโs ruling in 2022 to overturn Roe v. Wade, a decision that compounded the impact of Catholic health care restrictions. In its wake, roughly a third of states have banned or severely limited access to abortion, creating a one-two punch for women seeking to prevent pregnancy or to end one. Ironically, some states where Catholic hospitals dominate โ such as Washington, Oregon, and Colorado โ are now considered medical havens for women in nearby states that have banned abortion.
ั๎น๓ๅ๚ดซรฝา๎l Health News analyzed state-level birth data to discover that more than half a million babies are born each year in the U.S. in Catholic-run hospitals, including those owned by CommonSpirit Health, Ascension, Trinity Health, and Providence St. Joseph Health. Thatโs 16% of all hospital births each year, with rates in 10 states exceeding 30%. In Washington, half of all babies are born at such hospitals, the highest share in the country.
โWe had many instances where people would have to get in their car to drive to us while they were bleeding, or patients who had had their water bags broken for up to five days or even up to a week,โ said Chin, who has treated patients turned away by Catholic hospitals.
Physicians who turned away patients like that โwere going against evidence-based care and going against what they had been taught in medical school and residency,โ she said, โbut felt that they had to provide a certain type of care โ or lack of care โ just because of the strength of the ethical and religious directives.โ
Following religious mandates can be dangerous, Chin and other clinicians said.

When a patient has chosen to end a pregnancy after the amniotic sac โ or water โ has broken, Pettker said, โany delay that might be added to a procedure that is inevitably going to happen places that person at risk of serious, life-threatening complications,โ including sepsis and organ infection.
Reporters analyzed American Hospital Association data as of August and used Catholic Health Association directories, news reports, government documents, and hospital websites and other materials to determine which hospitals are Catholic or part of Catholic systems, and gathered birth data from state health departments and hospital associations. They interviewed patients, medical providers, academic experts, advocacy organizations, and attorneys, and reviewed hundreds of pages of court and government records and health institutions to understand how the directives affect patient care.
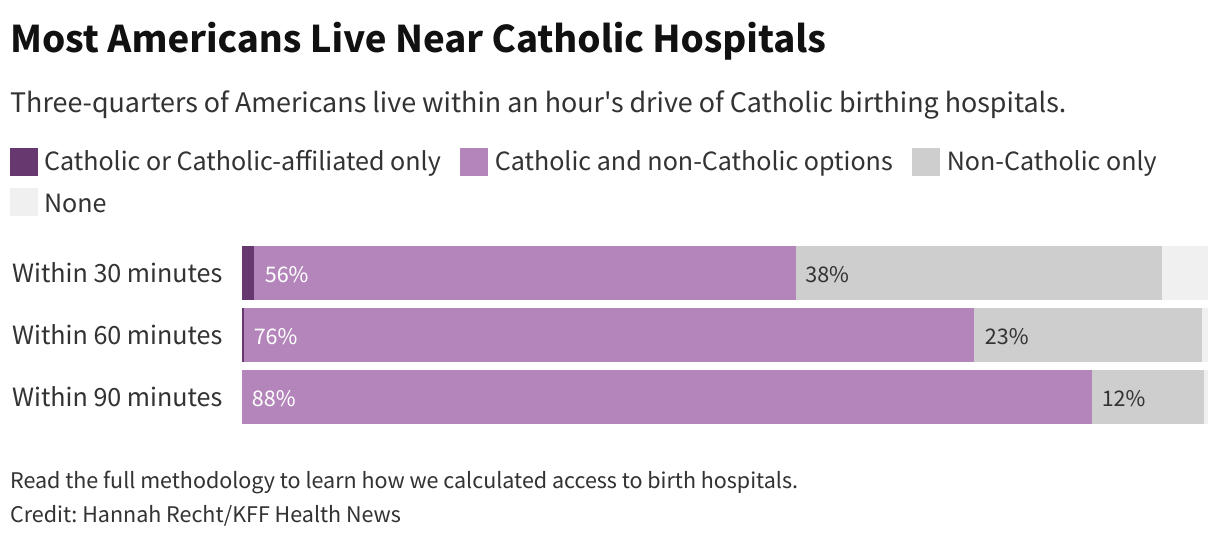
Nationally, nearly 800,000 people have only Catholic or Catholic-affiliated birth hospitals within an hourโs drive, according to ั๎น๓ๅ๚ดซรฝา๎l Health Newsโ analysis. For example, thatโs true of 1 in 10 North Dakotans. In South Dakota, itโs 1 in 20. When care is more than an hour away, academic researchers often define the area as a . Pregnant women who must drive farther to a delivery facility are at higher risk of harm to themselves or their fetus, .
Many Americans donโt have a choice โ non-Catholic hospitals are too far to reach in an emergency or arenโt in their insurance networks. Ambulances may take patients to a Catholic facility without giving them a say. Women often donโt know that hospitals are affiliated with the Catholic Church or that they restrict reproductive care, .
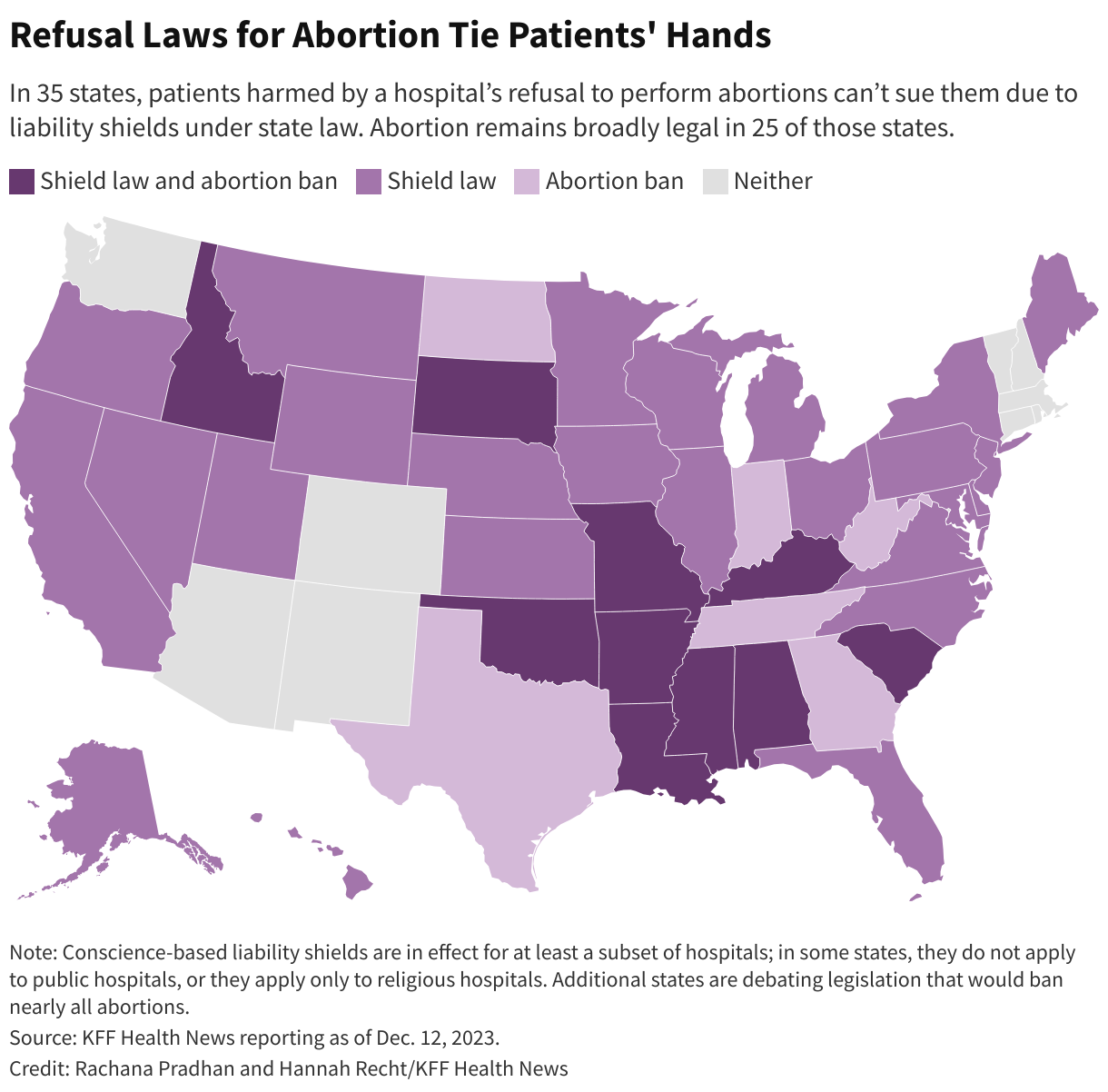
And, in most of the country, state laws shield at least some hospitals from lawsuits for not performing procedures they object to on religious grounds, leaving little recourse for patients who were harmed because care was withheld. Thirty-five states prevent patients from suing hospitals for not providing abortions, including 25 states where abortion remains broadly legal. About half of those laws donโt include exceptions for emergencies, ectopic pregnancies, or miscarriages. Sixteen states prohibit lawsuits against hospitals for refusing to perform sterilization procedures.
โItโs hard for the ordinary citizen to understand, โWell, what difference does it make if my hospital is bought by this other big health system, as long as it stays open? Thatโs all I care about,โโ said Erin Fuse Brown, who is the director of the Center for Law, Health & Society at Georgia State University and an expert in health care consolidation. Catholic directives also ban medical aid in dying for terminally ill patients.
People โmay not realize that theyโre losing access to important services, like reproductive health [and] end-of-life care,โ she said.
โOur Faith-Based Health Care Ministryโ
After the Supreme Court ended the constitutional right to abortion in June 2022, Michigan resident Kalaina Sullivan wanted surgery to permanently prevent pregnancy.

Michigan voters in November enshrined the right to abortion under the state constitution, but the stateโs concentration of Catholic hospitals means people like Sullivan sometimes still struggle to obtain reproductive health care.
Because her doctor worked for the Catholic chain Trinity Health, the nationโs fourth-largest hospital system, she had the surgery with a different doctor at North Ottawa Community Health System, an independent hospital near the shores of Lake Michigan.
Less than two months later, that, too, became a Catholic hospital, newly acquired by Trinity.
To mark the transition, Cory Mitchell, who at the time was the mission leader of Trinity Health Muskegon, stood before his new colleagues and offered a blessing.
โThe work of your hands is what makes our faith-based health care ministry possible,โ he said, according to a video of the ceremony Trinity Health provided to ั๎น๓ๅ๚ดซรฝา๎l Health News. โMay these hands continue to bring compassion, compassion and healing, to all those they touch.โ
Trinity Health declined to answer detailed questions about its merger with North Ottawa Community Health System and the ethical and religious directives. โOur commitment to high-quality, compassionate care means informing our patients of all appropriate care options, and trusting and supporting our physicians to make difficult and medically necessary decisions in the best interest of their patientsโ health and safety,โ spokesperson Jennifer Amundson said in an emailed statement. โHigh-quality, safe care is critical for the women in our communities and in cases where a non-critical service is not available at our facility, the physician will transfer care as appropriate.โ
Leaders in Catholic-based health systems have hammered home the importance of the churchโs directives, which are issued by the U.S. Conference of Catholic Bishops, all men, and were first drafted in 1948. The essential view on abortion is as it was in 1948. The last revision, in 2018, added several directives addressing Catholic health institution acquisitions or mergers with non-Catholic ones, including that โwhatever comes under control of the Catholic institution โ whether by acquisition, governance, or management โ must be operated in full accord with the moral teaching of the Catholic Church.โ
โWhile many of the faithful in the local church may not be aware of these requirements for Catholic health care, the local bishop certainly is,โ wrote Sister Doris Gottemoeller, a former board member of the Bon Secours Mercy Health system, in a 2023 . โIn fact, the bishop should be briefed on a regular basis about the hospitalโs activities and strategies.โ
Now, for care at a non-Catholic hospital, Sullivan would need to travel nearly 30 miles.
โI donโt see why thereโs any reason for me to have to follow the rules of their religion and have that be a part of whatโs going on with my body,โ she said.
Risks Come With Religion
Nathaniel Hibner, senior director of ethics at the Catholic Health Association, said the ethical and religious directives allow clinicians to provide medically necessary treatments in emergencies. In a pregnancy crisis when a personโs life is at risk, โI do not believe that the ERDs should restrict the physician in acting in the way that they see medically indicated.โ
โCatholic health care is committed to the health of all women and mothers who enter into our facilities,โ Hibner said.
The directives permit care to cure โa proportionately serious pathological condition of a pregnant womanโ even if it would โresult in the death of the unborn child.โ Hibner demurred when asked who defines what that means and when such care is provided, saying, โfor the most part, the physician and the patients are the ones that are having a conversation and dialogue with what is supposed to be medically appropriate.โ
It is common for practitioners at any hospital to consult an ethics board about difficult cases โ such as whether a teenager with cancer can decline treatment. At Catholic hospitals, providers must ask a board for permission to perform procedures restricted by the religious directives, clinicians and researchers say. For example, could an abortion be performed if a pregnancy threatened the motherโs life?

How and when an ethics consultation occurs depends on the hospital, Hibner said. โThat ethics consultation can be initiated by anyone involved in the direct care of that situation โ the patient, the surrogate of that patient, the physician, the nurse, the social worker all have the ability to request a consultation,โ he said. When asked whether a consultation with an ethics board can occur without a request, he said โsometimes it could.โ
How strictly directives are followed can depend on the hospital and the views of the local bishop.
โIf the hospital has made a difficult decision about a critical pregnancy or an end-of-life care situation, the bishop should be the first to know about it,โ Gottemoeller wrote.
In an interview, Gottemoeller said that even when pregnancy termination decisions are made on sound ethical grounds, not informing the bishop puts him in a bad position and hurts the church. โIf thereโs a possibility of it being misunderstood, or misinterpreted, or criticized,โ Gottemoeller said, the bishop should understand what happened and why โbefore the newspapers call him and ask him for an opinion.โ
โAnd if he has to say, โWell, I think you made a mistake,โ well, all right,โ she said. โBut donโt let him be blindsided. I mean, weโre one church and the bishop has pastoral concern over everything in his diocese.โ
Katherine Parker Bryden, a nurse midwife in Iowa who works for MercyOne, said she regularly tells pregnant patients that the hospital cannot perform tubal sterilization surgery, to prevent future pregnancies, or refer patients to other hospitals that do. MercyOne is one of the largest health systems in Iowa. Nearly half of general hospitals in the state are Catholic or Catholic-affiliated โ the highest share among all states.
The National Catholic Bioethics Center, an ethics authority for Catholic health institutions, that referrals for care that go against church teaching would be โimmoral.โ
โAs providers, youโre put in this kind of moral dilemma,โ Parker Bryden said. โAm I serving my patients or am I serving the archbishop and the pope?โ
In response to questions, MercyOne spokesperson Eve Lederhouse said in an email that its providers โoffer care and services that are consistent with the guidelines of a Catholic health system.โ
Maria Rodriguez, an OB-GYN professor at Oregon Health & Science University, said that as a resident in the early 2000s at a Catholic hospital she was able to secure permission โ what she calls a โpope noteโ โ to sterilize some patients with conditions such as gestational diabetes.
Annie Iriye, a retired OB-GYN in Washington state, said that more than a decade ago she sought permission to administer medication to hasten labor for a patient experiencing a second-trimester miscarriage at a Catholic hospital. She said she was told no because the fetus had a heartbeat. The patient took 10 hours to deliver โ time that would have been cut by half, Iriye said, had she been able to follow her own medical training and expertise. During that time, she said, the patient developed an infection.

Iriye and Chin were part of an effort by reproductive rights groups and medical organizations that pushed for a state law to protect physicians if they act against Catholic hospital restrictions. The bill, , was opposed by the Washington State Hospital Association, whose membership includes multiple large Catholic health systems.
State lawmakers in Oregon in 2021 enacted legislation that if they would reduce access to the types of care constrained by Catholic directives. The hospital lobby has . Washington state lawmakers last year, which the hospital association opposes.
Hibner said Catholic hospitals are committed to instituting systemic changes that improve maternal and child health, including access to primary, prenatal, and postpartum care. โThose are the things that I think rural communities really need support and advocacy for,โ he said.
Maldonado, the nurse midwife, still thinks of her patient who was forced to stay pregnant with a baby who could not survive. โTo feel like she was going to have to fight to have an abortion of a baby that she wanted?โ Maldonado said. โIt was just horrible.โ
ั๎น๓ๅ๚ดซรฝา๎l Health News data editor Holly K. Hacker contributed to this report.