Sam Walker, 35, has severe autism and other disabilities. He is deaf and cannot speak. Sometimes when he’s frustrated, he hits himself or others.
Medicaid provides about $8,500 a month for health workers who visit his apartment in the basement of his parents’ home. The staffers help him with everyday tasks, including dressing, bathing, and eating. They also take Walker on outings, such as dining at restaurants, volunteering at Goodwill, and exercising at a recreation center or on park trails. They stick to a strict routine, which soothes him.
His parents say that without the in-home services, their son would need to move to a specialized residential facility in another state. Sending him away would break their hearts and cost taxpayers much more money. They strive to keep him home because they know change makes him anxious.
“The last thing I want is to put him into some kind of care facility, where he’ll just get kicked out,” said his mother, Leisa. The Iowa Department of Health and Human Services did not respond to čŅ╣¾Õ·┤½├ĮęĢŅl Health News’ questions about the Walkers’ case.
Federal Cuts Raise Pressure
Patient advocates say state administrators in Iowa appear to be reining in Medicaid spending by cutting what are known as home and community-based services for people with disabilities, and they’ve heard of multiple families facing battles like the Walkers’.
Disability rights advocates expect the pressure to intensify as states respond to reductions in federal Medicaid funding called for under the Trump administration’s signature tax and spending law, which passed last year.
June Klein-Bacon, CEO of the Brain Injury Association of Iowa, said the cuts and proposed rule changes appear to be part of a quiet attempt to save money in response to the state’s budget deficit and expected reductions in federal Medicaid funding.
Medicaid, jointly financed by the federal and state governments, covers people with low incomes or disabilities. Walker is one of served by “Medicaid waiver” programs, which pay for care that allows people with disabilities or who are at least 65 to live at home.
Unlike most parts of Medicaid, waiver programs are optional for states. Idaho’s governor noted that fact in January, when he suggested legislators consider cutting them. Disability rights groups fear other states will do the same. Leaders in , , and have considered such cuts this year.
Leisa Walker has heard Trump administration officials claim the national Medicaid cuts are intended to reduce waste, fraud, and abuse. That’s not how it will play out, she said. “These are real people, real families, and this causes real suffering when you do this to people,” she said. “It’s a very scary time.”
a private insurance company that manages Sam Walker’s Medicaid benefits, intends to cut his in-home care coverage by about $3,200 per month, his mother said. Company leaders told a judge they are following state officials’ direction, but they did not dispute Leisa Walker’s math.
Walker has been on the waiver program for three decades. It covers assistance from workers known as “direct service providers” ŌĆö one of whom has been with him for 25 years. His parents receive no pay for the hours they spend caring for him when the aides aren’t working.
On a February morning, Leisa and Kent Walker drove an hour and a half to Des Moines for an appeal hearing. An administrative law judge sat behind a wooden desk in a conference room as the Walkers and their lawyer faced off against three representatives from Iowa Total Care, a subsidiary of the national insurer Centene Corp.
Leisa testified that her son is 6 feet tall and weighs 230 pounds. Although he knows some sign language, he has trouble communicating, she said. When he becomes frustrated or his routine is interrupted, he sometimes wails and hits himself or other people. “It’s devastating to watch,” she testified.
He’s not a bad person, she said. “He doesn’t understand how strong he is.”
She said her family would try to keep his main caregiver employed under the planned Medicaid reduction but would have to drop others who cover nights and weekends. She said no residential facility near their southern Iowa home could address her son’s complicated needs. She said a case manager told her that a Florida facility might be the closest one that could safely handle him.
Leisa Walker testified that the state’s Medicaid program would pay about $22,000 per month to put him in an institution, more than double what the program spends on his home care.
Sam Walker’s longtime psychiatrist, Christopher Okiishi, testified that Walker’s family and their support staff spent years developing a “fragile” but stable existence for him.
Lori Palm, a senior manager for Iowa Total Care, testified that Sam Walker gets about 16 hours of daily assistance financed by Medicaid. Palm said much of that time amounts to “supervision.” She said state officials recently advised her company that the program should pay mainly for “skill-building” time, not supervision.
The Walkers showed the judge a 2018 document in which a previous Iowa Medicaid director stipulated that supervision of people with disabilities is an allowable service for workers paid under the program.

Judge Rachel Morgan asked the Iowa Total Care representatives if the recent policy change was made in writing by the state Department of Health and Human Services. They said it was not and that they couldn’t specify who at the department had given them the new guidance.
The judge suggested during the hearing that for someone like Sam Walker, learning to regulate emotions could be an important form of skill-building. Three days later, the judge ruled in the Walkers’ favor, writing that the insurer’s attempt to cut care hours was improper. The insurer appealed the decision to the director of the Iowa Department of Health Human Services, who could overrule it. The dispute could eventually wind up in district court.
Iowa Total Care and the state Department of Health and Human Services did not respond to questions about the reports that many other Iowans with disabilities face reductions in care hours covered by Medicaid. Department spokesperson Danielle Sample said in an email that the agency supports home and community-based services, which, she noted, help “states save money by avoiding expensive long-term facility care.”
Spokespeople for the federal Department of Health and Human Services, which oversees Medicaid nationally, did not respond to a request for comment on the issue.
Medicaid waiver programs started in the 1980s, after President Ronald Reagan heard about an Iowa girl with a disability who was forced to live in a hospital for months because Medicaid wouldn’t pay for home care. The Republican president thought it was outrageous that the girl, had to live that way, even though home care would have been cheaper.
Members of Congress approved allowing states to use their Medicaid programs to pay for in-home care. But they made the change optional, to offer states flexibility and encourage innovation.
Designating such spending as optional “waiver programs” also made the change more politically palatable, said Kim Musheno, senior director of Medicaid policy for , which represents people with intellectual and developmental disabilities.
Prospects were much different for babies born with serious disabilities before the change, Musheno said. “Doctors instructed families to forget they existed, and to put them in an institution.”
Waivers Have Been Cut Before
All states have Medicaid waiver programs, but benefits and the number of people covered vary significantly. Applicants often wait months or years to get into the programs because of limited funding. More than 600,000 Americans were on waiting lists or “interest lists” for waiver services in 2025, , a health information nonprofit that includes čŅ╣¾Õ·┤½├ĮęĢŅl Health News.
Disability rights advocates and care providers have fought for decades to maintain funding for the programs, but a national leader said the threat feels especially severe now.
“When Medicaid is cut, people with disabilities are at the center of the impact,” said Barbara Merrill, CEO of the American Network of Community Outcomes and Resources, which represents agencies that care for people with intellectual disabilities or autism.
That’s what happened after Congress reduced Medicaid funding in 2011, according to a recent paper published by .
States could again rein in waiver programs by limiting enrollment, reducing covered services, or cutting pay for caregivers, who already are in short supply.
However, states that try to cut the in-home care programs could face legal challenges, Musheno said. The U.S. Supreme Court declared in 1999 that people with disabilities have a right to live outside of institutions if possible. The decision, in the case of , has been cited in lawsuits against states that fail to provide care options apart from nursing homes and similar facilities.
Several Iowans who belong to a Facebook group for Medicaid participants have posted in recent weeks that their families were notified of impending cuts in coverage of home care services for people with disabilities.
Sam Walker’s main caregiver, Andy Koettel, has worked with him since Walker was in fourth grade. Koettel, who works full-time, knows how to keep Walker calm in most situations and soothe him during a blowup. Their relationship took years to build, and it is a key reason Walker can continue to live at home with his parents, Koettel said.
“If I was not there, it would be incredibly difficult for all of them,” he said.
čŅ╣¾Õ·┤½├ĮęĢŅl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFŌĆöan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/medicaid/medicaid-cuts-disabilities-home-community-based-services-iowa/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2162736&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Services at risk include the 24/7 care that allows a 39-year-old with cerebral palsy to live independently; the in-home caregiving that lets a 26-year-old with brain damage from a hemorrhage at birth stay in his family home; and private duty nursing for a 19-year-old with cerebral palsy who has qualified for hospice care for complications including pulmonary decline from a spinal cord injury.
Concerns for such care arose when Idaho Gov. Brad Little, a Republican, proposed cutting $22 million from Medicaid ŌĆö the joint state-federal health insurance program for people with low incomes or disabilities ŌĆö to balance the state budget. Home- and community-based services such as caregiving, nursing, and residential rehabilitation are optional under Medicaid, and Little for the cuts.
Across the country, people with disabilities and their families are confronting similar plans to cut Medicaid as states grapple with budget challenges compounded by congressional Republicans’ One Big Beautiful Bill Act, which is expected to reduce federal spending on Medicaid by nearly $1 trillion over the next decade.
A four-hour town hall on the proposal in Idaho drew to the state capitol. Colorado lawmakers heard from concerned residents before pausing a pay cut for family caregivers. In Missouri, families raised alarms about a to services for people with disabilities.
“We saw this coming. We’ve tried to educate members of Congress,” said Kim Musheno, the senior director of Medicaid policy at The Arc, a national disability rights organization.
“Whenever there’s pressure on state budgets like those that are caused by the One Big Beautiful Bill Act, they go after Medicaid, and then they go after optional services,” Musheno said.
Many cuts included in the GOP bill, which President Donald Trump signed into law in July, haven’t yet taken effect, but the law is already impacting state budgets, particularly in states that align their tax rules with federal regulations.
Conforming to the federal law is expected to cost Idaho this year. Colorado lawmakers were called into a special session last year to address a created by the law. Those shortfalls ŌĆö combined with national trends of increased Medicaid costs, , and further tax cuts passed by some state legislatures ŌĆö are putting pressure on Medicaid programs.
Still, Musheno said she was surprised by how quickly Idaho targeted services for people with disabilities. “I couldn’t believe it.”
Little had already ordered Medicaid cuts last year as part of an effort to address a budget shortfall after years of and increasing program costs. That led to a in September for medical providers’ work with Medicaid patients. Little’s new proposed would be on top of those previous rate cuts.
“We were told by the legislature that they want to save some money in Medicaid, and so what we put together was a list of seven different options that were there,” Little said at a Feb. 17 press event. “There’s only so many levers we can pull in the Medicaid area that doesn’t jeopardize our funding.”


ŌĆśWe Just Hold Our Breath’
Amber Grant said any further cuts for the nursing agency that provides care for her 19-year-old son, Matty, could be catastrophic.
He was born with brain damage and cerebral palsy before suffering a spinal cord injury when he was 10. In 2024, he briefly received hospice care before the family decided to work with a palliative care team to help him live out his life.
Through Medicaid, Matty qualifies for 120 hours of in-home private duty nursing care per week. But because of a nursing shortage, he typically receives only about half of that care, and Grant said it would get worse if the nursing agency is subjected to any more reductions.
“The reality is that any of us at any point in time could become disabled,” Grant said. “What kind of quality of care would we want?”

The potential cuts run even deeper for Grant’s family. Through another optional in-home Medicaid program, she and her husband, Jason, are both eligible to be paid for caring for their older son, Luke. The 24-year-old has autism, epilepsy, and an autoimmune condition and requires supervision 24 hours a day.
Jason primarily works as a self-employed remodeler, but Grant’s only income is the $21 an hour she gets to care for Luke. But she can be compensated only for the time she has him one-on-one, meaning when someone else is taking care of Matty, such as Jason or his nurses.
Grant said keeping up with the family’s house payments will be nearly impossible if they lose that income, and she said it seems like only a matter of time before some or all of her sons’ in-home care is disrupted. Idaho is in federal Medicaid funding over the next decade as a result of the One Big Beautiful Bill Act, according to KFF, a national health information nonprofit that includes čŅ╣¾Õ·┤½├ĮęĢŅl Health News.
“We just hold our breath every legislative session,” Grant said. “I feel like I’m always trying to prove their worth, to prove their value, and it’s exhausting.”
State Rep. Josh Tanner, a Republican who co-chairs the legislature’s powerful budget committee, said he opposed cutting home- and community-based services, but it was up to a separate committee and workgroup to finalize cuts to the Medicaid program.
Medicaid covers . , the federal government picked up 80% of the state program’s $3.6 billion tab in 2023. Tanner said tapping the state’s $1.3 billion in reserves to fill the $22 million gap was a nonstarter.
“We don’t really have an overall revenue problem in the state right now,” Tanner said, “but we do have a spending problem, and part of that has been Medicaid in general.”
Senate Minority Leader Melissa Wintrow, a Democrat on the budget committee, disagreed, pointing instead to five years of tax cuts passed by the Republican supermajority that have in lost revenue, including last year.
“What we need to do is restore the revenue that we cut and put it back and admit the mistake and stop harming people and the very services that Idahoans depend on,” Wintrow said.
ŌĆśIt Keeps Me Awake at Night’
It’s also unclear whether cuts to community-based care would save Idaho money, something Tanner acknowledged. For optional Medicaid programs to be approved by the federal government, states must demonstrate that they are cheaper than existing alternatives, such as being cared for in a nursing home. Cutting community-based care would probably push many people with disabilities into more costly institutional care.
That’s what Toni Belknap-Brinegar fears for her son Antahn Brinegar.

A brain hemorrhage at birth left Antahn, now 26, with severe brain damage, physical and developmental issues, and a seizure disorder. Belknap-Brinegar is his primary caregiver, but she realized when Antahn was 8 or 9 that she wasn’t physically capable of caring for her growing son. Now 200 pounds, he has two paid in-home caregivers, Belknap-Brinegar said, both single mothers whose own livelihoods may be in the balance amid talks of cuts.
Nursing homes aren’t equipped to properly care for Antahn, Belknap-Brinegar said. He needs to be constantly monitored for seizures. He can’t communicate his needs well, for example when he has to go to the bathroom.
“Without the services that he has and the care that he gets now, he would end up in a care center, and frankly, he would die,” Belknap-Brinegar said.
While home and community-based services are technically optional parts of Medicaid, a required states to provide them to people with disabilities when appropriate. A Justice Department investigation in the waning days of the Biden administration found that Idaho was into nursing homes, in violation of that ruling. The Trump administration is attempting to slash access to the lawyers who help ensure those rules are followed.
Documents also show the state agency that oversees Medicaid does not think the state has enough space in its residential facilities to care for all the people whose home- and community-based services could be cut under the governor’s plan.
That’s Ned Fowkes’ worry for his 39-year-old daughter, Eva.
A brain bleed when she was an infant left Eva with severe cerebral palsy and significant developmental disabilities. Although Eva is unable to speak, she has a “wonderful awareness,” Fowkes said, and is able to communicate through her expressions and convey her preferences.
After being cared for by her parents for 21 years, Eva was eager for the chance to move into a supported living home, where she could get round-the-clock care while living with another person with disabilities.
“Like most 21-year-olds, she probably wanted to hit the road and not be under the roof of her parents anymore,” Fowkes recalled. “She’s always been courageous in that sense.”


Fowkes and his wife visit at least three times a week, but at 79 and 76, they are no longer able to provide their daughter’s direct care.
The staff at Eva’s home already barely make a living wage, Fowkes said. Cuts to the program that pays for her care would trigger more turnover ŌĆö or, worse, shutter the agency that staffs the home.
“I don’t know what we would do,” Fowkes said. “Eventually we’d lose our home. We would be bankrupt. Where would Eva go? Where would her roommate go? Who would care for them?”
“It keeps me awake at night,” he said. “Believe me.”
čŅ╣¾Õ·┤½├ĮęĢŅl Health News’ Hayat Norimine contributed to this report.
This <a target="_blank" href="/medicaid/medicaid-cuts-disabled-in-home-care-idaho-one-big-beautiful-bill/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2161466&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>The 59-year-old, who lives in Harrisburg, North Carolina, closed her nonprofit circus arts school last year because she could no longer see well enough to complete paperwork. She then worked making dough at a pizza shop for a bit. Currently, she sorts recyclable materials, including cans and bottles, at a local concert venue. It is her main source of income ― but the work isn’t year-round.
“This place knows me, and this place loves me,” Kelley said of her employer. “I don’t have to explain to this place why I can’t read.”
Kelley, who lives in a camper, survives on less than $10,000 a year. She says that’s possible, in part, because of her Medicaid health coverage, which pays for arthritis and anxiety medications and has enabled doctor visits to manage high blood pressure.
But she worries about losing that coverage next year, when rules take effect requiring millions of people like Kelley to work, volunteer, attend school, or perform other qualifying activities for at least 80 hours a month.
“I’m scared right now,” she said.


Before the coverage changes were signed into law, Republican lawmakers suggested that young, unemployed men were taking advantage of the government health insurance program that provides coverage to millions of low-income or disabled people. Medicaid is not intended for “29-year-old males sitting on their couches playing video games,” House .
But, in reality, adults ages 50 to 64, particularly women, are likely to be , said Jennifer Tolbert, deputy director of the Program on Medicaid and the Uninsured at KFF, a health information nonprofit that includes čŅ╣¾Õ·┤½├ĮęĢŅl Health News. For Kelley and others, the work requirements will create barriers to keeping their coverage, Tolbert said. Many could lose Medicaid as a result, putting their physical and financial health at risk.
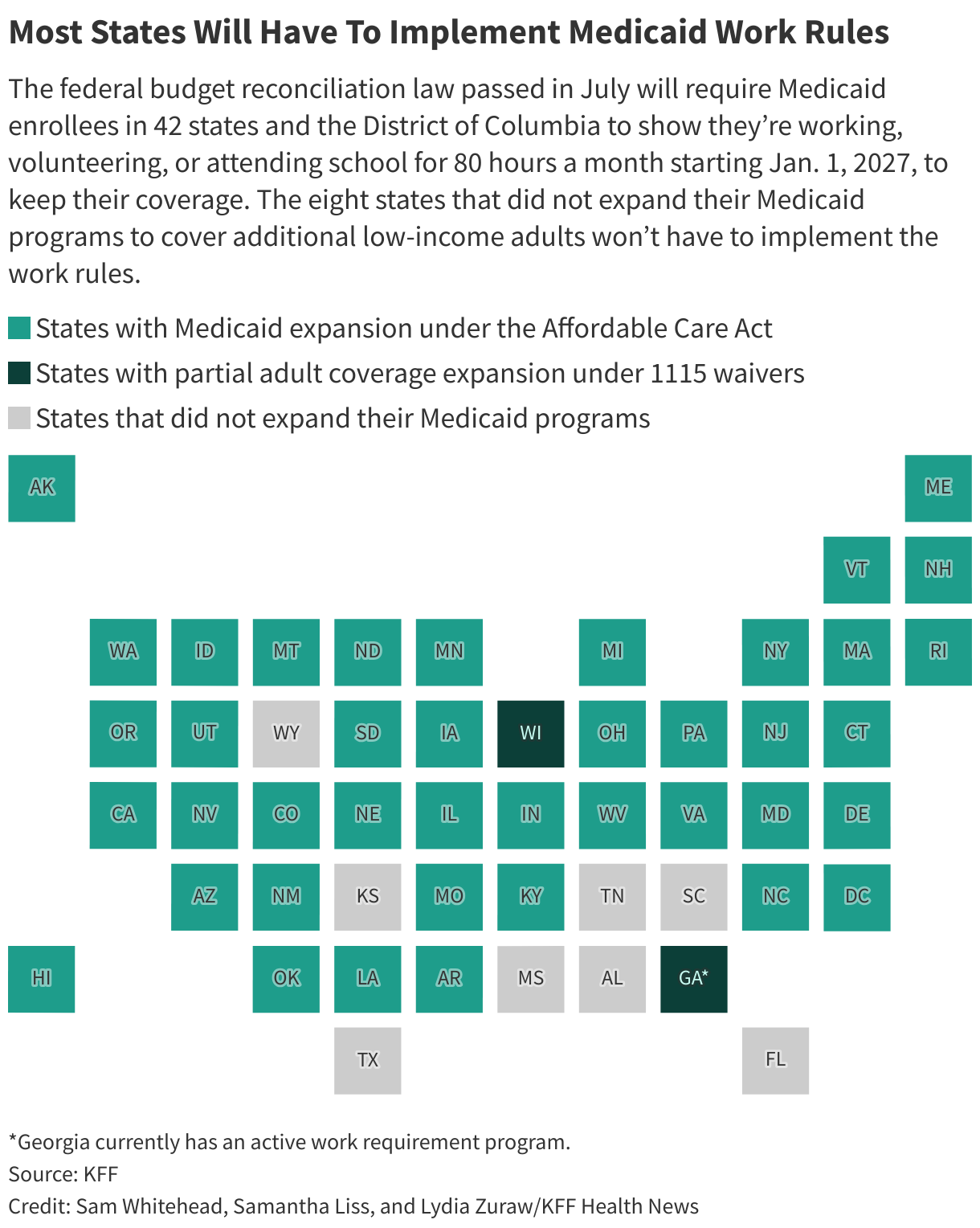
Starting next January, some 20 million low-income Americans in 42 states and Washington, D.C., will need to meet the activity requirements to gain or keep Medicaid health coverage.
Alabama, Florida, Kansas, Mississippi, South Carolina, Tennessee, Texas, and Wyoming didn’t expand their Medicaid programs to cover additional low-income adults under the Affordable Care Act, so they won’t have to implement the work rules.
The nonpartisan Congressional Budget Office predicts the work rules will result in at least 5 million fewer people with Medicaid coverage over the next decade. Work rules are the largest driver of coverage losses in the GOP budget law, which slashes nearly $1 trillion to offset the costs of tax breaks that mainly benefit the rich and increase border security, .
“We’re talking about saving money at the expense of people’s lives,” said Jane Tavares, a gerontology researcher at the University of Massachusetts Boston. “The work requirement is just a tool to do that.”
Department of Health and Human Services spokesperson Andrew Nixon said requiring “able-bodied adults” to work ensures Medicaid’s “long-term sustainability” while safeguarding it for the vulnerable. Exempt are people with disabilities, caregivers, pregnant and postpartum individuals, veterans with total disabilities, and others facing medical or personal hardship, Nixon told čŅ╣¾Õ·┤½├ĮęĢŅl Health News.
Medicaid expansion has provided a lifeline for middle-aged adults who otherwise would lack insurance, according to . Medicaid covers 1 in 5 Americans ages 50 to 64, giving them access to health coverage before they qualify for Medicare at age 65.
Among women on Medicaid, those ages 50 through 64 are more likely to face challenges keeping their coverage than their younger female peers and are likely to have a greater need for health care services, Tolbert said.
These middle-aged women are less likely to be working the required number of hours because many serve as family caregivers or have illnesses that limit their ability to work, Tolbert said.
Tavares and other researchers found that of the total Medicaid population is considered “able-bodied” and not working. This group consists largely of women who are very poor and have left the workforce to become caretakers. Among this group, 1 in 4 are 50 or older.
“They are not healthy young adults just hanging out,” the researchers stated.
Plus, making it harder for people to maintain Medicaid coverage “may actually undermine their ability to work” because their health problems go untreated, Tolbert said. Regardless, if this group loses coverage, their chronic health conditions will still need to be managed, she said.
Adults often start wrestling with health issues before they’re eligible for Medicare.
If older adults don’t have the means to pay to address health issues before age 65, they’ll ultimately be sicker when they qualify for Medicare, costing the program more money, health policy researchers said.
Many adults in their 50s or early 60s are no longer working because they’re full-time caregivers for children or older family members, said caregiver advocates, who refer to people in the group as “the sandwich generation.”


The GOP budget law does allow some caregivers to be exempted from the Medicaid work rules, but the carve-outs are “very narrow,” said Nicole Jorwic, chief program officer for the group Caring Across Generations.
She worries that people who should qualify for an exemption will fall through the cracks.
“You’re going to see family caregivers getting sicker, continuing to forgo their own care, and then you’re going to see more and more families in crisis situations,” Jorwic said.
Paula Wallace, 63, of Chidester, Arkansas, said she worked most of her adult life and now spends her days helping her husband manage his advanced cirrhosis.
After years of being uninsured, she recently gained coverage through her state’s Medicaid expansion, which means she’ll have to comply with the new work requirements to keep it. But she’s having a hard time seeing how that will be possible.
“With me being his only caregiver, I can’t go out and work away from home,” she said.
Wallace’s husband receives Social Security Disability Insurance, she said, and the law says she should be exempt from the work rules as a full-time caregiver for someone with a disability.
But federal officials have yet to issue specific guidance on how to define that exemption. And ― the only states to have run Medicaid work programs ― shows that many enrollees struggle to navigate complicated benefits systems.
“I’m very concerned,” Wallace said.
čŅ╣¾Õ·┤½├ĮęĢŅl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFŌĆöan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-care-costs/medicaid-work-requirements-middle-aged-adults-women/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2151346&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Dunnebacke lay still atop a folding table that was dressed as a bed, complaining that her legs hurt. Registered nurse Ana Kanellos, rolling up two small white towels, demonstrated how to elevate her ankles to ease the pain.
“ŌĆŖMom’s legs are always swollen? Raise ’em up,” Kanellos said.
About 20 New Orleans residents listened intently, eager to learn more about how to care for loved ones at home when they’re nearing the end of their lives. Attendee Alix Vargas said she used to be terrified of dying. But about three years ago, a close cousin’s death led her to attend group writing workshops, helping her embrace her grief and conquer her fear.
“ŌĆŖI’m feeling very called towards this work,” she said. “It’s definitely knowledge that I wanted to obtain and expand my mind in that way. And this is also something that we’re all going to encounter in our lives.”
The workshop made her think about a neighbor whose mother has dementia.
“ŌĆŖI was immediately thinking, ŌĆśOK, there’s someone in my immediate orbit that is experiencing this,’” Vargas recalled. ŌĆś“Here’s a practical way to put the mutual aid in use.’”
Demand for home health care, including at-home hospice care, has skyrocketed since the onset of the covid pandemic, as has the number of family caregivers. An estimated 63 million people in the U.S. ŌĆö nearly a quarter of all American adults ŌĆö provided care over the previous year to another person with a medical condition or disability, usually another adult, according to by AARP and the National Alliance for Caregiving. In the past 10 years, about 20 million more people have served as caregivers.


With nearly 1 in 5 Americans expected to be 65 or older by 2030, health care experts predict the demand for at-home caregivers will continue to rise. Online resources for end-of-life care are widely available, but hands-on training to prepare people to become caregivers is not, and it can be expensive. Yet untrained family members-turned-caregivers are taking on nursing and medical tasks.
Donald Trump promised more support for caregivers during his 2024 campaign, including a pledge to create new tax credits for those caring for family members. He endorsed a bill reintroduced in Congress this year that would allow family caregivers to receive tax credits of up to $5,000, but the legislation hasn’t moved forward.
Meanwhile, the Medicaid cuts expected from Republicans’ One Big Beautiful Bill Act, which President Trump signed in July, could prompt states looking to offset their added expenses to reconsider participating in optional state Medicaid programs, such as the one that helps pay for . That would threaten to make dying at home even more unaffordable for low-income families, said advocates and researchers.
Advocates like Osha Towers are trying to help caregivers navigate the uncertainty. Towers leads LGBTQ+ engagement at , a national organization that focuses on improving end-of-life care, preparation, and education.
“It is certainly very scary, but what we know we can do right now is be able to just show up for all individuals to make sure that they know what they need to be prepared for,” Towers said.
In New Orleans, a , which focuses on supporting family caregivers providing end-of-life and death care, is one of the organizations trying to help fill the knowledge gap. Wake put on the free, three-day September workshop where Dunnebacke, the group’s founder, pretended to be a dying patient. Such workshops are aimed at preparing attendees for what to expect when loved ones are dying and how to care for them, even without costly professional help. Full-time at-home care is rare.
“You don’t have to have any special training to do this work,” Dunnebacke said. “You just need some skills and some supports to make that happen.”


In some ways, the evolution of end-of-life care in the U.S. over the past century has come full circle. It was only starting in the 1960s that people shifted from dying at home to dying in hospitals, nursing homes, and hospice facilities.
Such institutions can provide immediate advanced medical support and palliative care for patients, but they often lack the human connection that home care provides, said Laurie Dietrich, Wake’s programs manager.
Now, more people want to die in their homes, among family, but with the support and technology that comes with modern medical facilities.
In the past decade, death doulas ŌĆö who support the nonmedical and emotional needs of the dying and their loved ones ŌĆö have grown in popularity to help guide people through the dying process, helping to fill that gap. Douglas Simpson, executive director of the , said his organization recognizes the lack of resources for death care, so it is training doulas to be community educators. He hopes doulas can be especially useful in rural communities and lead conversations about dying.
“Making people more open, more comfortable about talking about death and considering their mortality,” Simpson said.
Death doula training varies depending on the organizer, but Simpson’s group focuses on teaching attendees about the dying process, how to maintain the autonomy of the dying person, and how to be aware of how they show up to a job and take care of themselves while caring for others.
Some people who attended Wake’s workshop had also attended some form of death doula training in the past. After Nicole Washington’s mother was killed in 2023, she considered becoming a death doula. But she thought the doula training, which can cost $800 to $3,000, was clinical and impersonal, as opposed to Wake’s community-based approach.
“I feel very energized, very uplifted,” Washington said. “It’s also really nice to be in a space with people who are familiar with death and grief.”
Ochsner Health’s Susan Nelson, who has worked as a geriatrician for 25 years, said there is a need for more specialized programs to train and prepare caregivers, like Wake’s.
“Learning caregiving skills is probably, unfortunately, more trial by fire,” Nelson said.
Compassion & Choices is another organization trying to educate caregivers. Towers said the group’s training ranges from advanced planning to acting as a health care proxy to caring for the dying.
“We’ve gone to a place in our country where we’re so removed from end-of-life care in a way that we didn’t used to be,” Towers said.
Towers said the movement to care for people at home and give them community support has roots in the AIDS epidemic, when some doctors for AIDS patients. Friends, especially in the , started coordinating food delivery, visits, bedside vigils, and even touch circles, where patients could receive comforting forms of touch such as hand-holding to ease pain and feelings of isolation.
“I like to look at it as a blueprint for what we can get back to doing now, which is again just prioritizing community care,” Towers said.

This article was produced in collaboration with . Verite News reporter Christiana Botic contributed to this report.
This <a target="_blank" href="/aging/end-of-life-home-hospice-care-dying-new-orleans-louisiana/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2121520&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>“I have no children, no husband, no siblings,” Barden remembered saying. “Who’s going to hold my hand while I die?”
Barden, 75, never had children. She’s lived on her own in western Massachusetts since her husband passed away in 2003. “You hit a point in your life when you’re not climbing up anymore, you’re climbing down,” she told me. “You start thinking about what it’s going to be like at the end.”
It’s something that many older adults who live alone ŌĆö a growing population, ŌĆö wonder about. Many have family and friends they can turn to. But some have no spouse or children, have relatives who live far away, or are estranged from remaining family members. Others have lost dear friends they once depended on to advanced age and illness.
More than 15 million people 55 or older don’t have a spouse or biological children; nearly 2 million have no family members at all.

Still other older adults have become isolated due to sickness, frailty, or disability. Between , who do not live in nursing homes, aren’t in regular contact with other people. And research shows that isolation becomes even more common as death draws near.
Who will be there for these solo agers as their lives draw to a close? How many of them will die without people they know and care for by their side?
Unfortunately, we have no idea: National surveys don’t capture information about who’s with older adults when they die. But dying alone is a growing concern as more seniors age on their own after widowhood or divorce, or remain single or childless, according to demographers, medical researchers, and physicians who care for older people.
“We’ve always seen patients who were essentially by themselves when they transition into end-of-life care,” said Jairon Johnson, the medical director of hospice and palliative care for Presbyterian Healthcare Services, the largest health care system in New Mexico. “But they weren’t as common as they are now.”
Attention to the potentially fraught consequences of dying alone surged during the covid-19 pandemic, when families were shut out of hospitals and nursing homes as older relatives passed away. But it’s largely fallen off the radar since then.
For many people, including health care practitioners, the prospect provokes a feeling of abandonment. “I can’t imagine what it’s like, on top of a terminal illness, to think I’m dying and I have no one,” said Sarah Cross, an assistant professor of palliative medicine at Emory University School of Medicine.
Cross’ research shows that more people die at home now than in any other setting. While hundreds of hospitals have “No One Dies Alone” programs, which match volunteers with people in their final days, similar services aren’t generally available for people at home.
Alison Butler, 65, is an end-of-life doula who lives and works in the Washington, D.C., area. She helps people and those close to them navigate the dying process. She also has lived alone for 20 years. In a lengthy conversation, Butler admitted that being alone at life’s end seems like a form of rejection. She choked back tears as she spoke about possibly feeling her life “doesn’t and didn’t matter deeply” to anyone.

Without reliable people around to assist terminally ill adults, there’s also an elevated risk of self-neglect and deteriorating well-being. Most seniors don’t have enough money to pay for assisted living or help at home if they lose the ability to shop, bathe, dress, or move around the house.
Nearly $1 trillion in cuts to Medicaid planned under President Donald Trump’s tax and spending law, previously known as the “One Big Beautiful Bill Act,” probably will , economists and policy experts predict. Medicare, the government’s health insurance program for seniors, generally doesn’t pay for home-based services; Medicaid is the primary source of this kind of help for people who don’t have financial resources. But states may be forced to eviscerate Medicaid home-based care programs as federal funding diminishes.
“I’m really scared about what’s going to happen,” said Bree Johnston, a geriatrician and the director of palliative care at Skagit Regional Health in northwestern Washington state. She predicted that more terminally ill seniors who live alone will end up dying in hospitals, rather than in their homes, because they’ll lack essential services.
“Hospitals are often not the most humane place to die,” Johnston said.
While is an alternative paid for by Medicare, it too often falls short for terminally ill older adults who are alone. (Hospice serves people whose life expectancy is six months or less.) For one thing, hospice is underused: Fewer than half of older adults under age 85 take advantage of hospice services.
Also, “many people think, wrongly, that hospice agencies are going to provide person power on the ground and help with all those functional problems that come up for people at the end of life,” said Ashwin Kotwal, an associate professor of medicine in the division of geriatrics at the University of California-San Francisco School of Medicine.
Instead, agencies usually provide only intermittent care and rely heavily on family caregivers to offer needed assistance with activities such as bathing and eating. Some hospices won’t even accept people who don’t have caregivers, Kotwal noted.
That leaves hospitals. If seniors are lucid, staffers can talk to them about their priorities and walk them through medical decisions that lie ahead, said Paul DeSandre, the chief of palliative and supportive care at Grady Health System in Atlanta.
If they’re delirious or unconscious, which is often the case, staffers normally try to identify someone who can discuss what this senior might have wanted at the end of life and possibly serve as a surrogate decision-maker. Most states have laws specifying default surrogates, usually family members, for people who haven’t named decision-makers in advance.
If all efforts fail, the hospital will go to court to petition for guardianship, and the patient will become a ward of the state, which will assume legal oversight of end-of-life decision-making.
In extreme cases, when no one comes forward, someone who has died alone may be classified as “unclaimed” and buried in a common grave. This, too, is an increasingly common occurrence, according to “The Unclaimed: Abandonment and Hope in the City of Angels,” a book about this phenomenon, published last year.
Shoshana Ungerleider, a physician, founded End Well, an organization committed to improving end-of-life experiences. She suggested people make concerted efforts to identify seniors who live alone and are seriously ill early and provide them with expanded support. Stay in touch with them regularly through calls, video, or text messages, she said.
And don’t assume all older adults have the same priorities for end-of-life care. They don’t.
Barden, the widow in Massachusetts, for instance, has focused on preparing in advance: All her financial and legal arrangements are in order and funeral arrangements are made.
“I’ve been very blessed in life: We have to look back on what we have to be grateful for and not dwell on the bad part,” she told me. As for imagining her life’s end, she said, “it’s going to be what it is. We have no control over any of that stuff. I guess I’d like someone with me, but I don’t know how it’s going to work out.”

Some people want to die as they’ve lived ŌĆö on their own. Among them is 80-year-old Elva Roy, founder of Age-Friendly Arlington, Texas, who has lived alone for 30 years after two divorces.
When I reached out, she told me she’d thought long and hard about dying alone and is toying with the idea of medically assisted death, perhaps in Switzerland, if she becomes terminally ill. It’s one way to retain a sense of control and independence that’s sustained her as a solo ager.
“You know, I don’t want somebody by my side if I’m emaciated or frail or sickly,” Roy said. “I would not feel comforted by someone being there holding my hand or wiping my brow or watching me suffer. I’m really OK with dying by myself.”
čŅ╣¾Õ·┤½├ĮęĢŅl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFŌĆöan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/aging/aging-fear-dying-alone-single-childless-widowhood-divorce/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
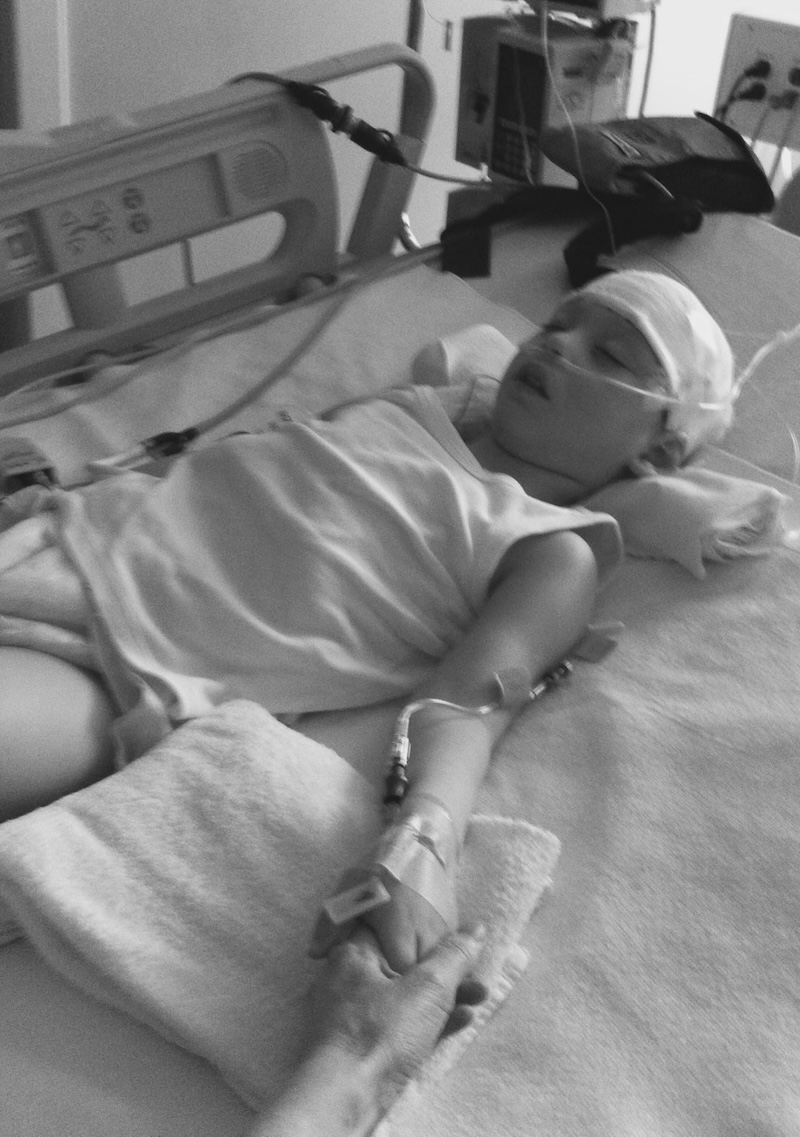
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2094660&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>“It is almost impossible to explain what it takes to keep a child alive who should be dead,” said Fabrello, whose son, Ysadore Maklakoff, experienced a rare brain condition called acute necrotizing encephalopathy at 9 months old.
Through North Carolina’s Medicaid program, Maklakoff qualifies for a large slate of medical care in the family’s home in Chapel Hill. Fabrello said she works with staffing agencies to arrange services. She also learned to give the care ordinarily performed by a doctor, skilled nurse, or highly trained therapist because she often can’t get help.
Now, broad cuts to North Carolina Medicaid will make finding and paying for care even more difficult.
Nationwide, states are scrambling to close budget shortfalls and are eyeing Medicaid, generally one of a state’s biggest costs ŌĆö even before President Donald Trump’s hulking tax-and-spending law decreases federal spending on Medicaid by about over the next decade.
North Carolina and Idaho have already announced plans to cut Medicaid payments to health care providers, including hospitals, doctors, and caregivers.
In Michigan and Pennsylvania ŌĆö where lawmakers have yet to pass budgets this year ŌĆö spending on Medicaid is part of those debates. In , lawmakers approved cuts to the program that will not affect who is eligible, said Hayden Mackley, a spokesperson for the state’s Office of Financial Management.
Medicaid is government health insurance for people with low incomes or disabilities and both state and federal dollars pay for the program.
North Carolina’s Medicaid agency announced it will institute on Oct. 1 a in pay for all providers who treat Medicaid patients. Primary care doctors face an 8% cut and specialty doctors a 10% drop in payments, according to the North Carolina Department of Health and Human Services.
Fabrello said her son’s dentist already called to say the office will not accept Medicaid patients come November. Fabrello fears dental work will become another service her son qualifies for but can’t get because there aren’t enough providers who accept Medicaid coverage.
Occupational and speech therapy, nursing care, and respite care are all difficult or impossible to get, she said. In a good week, her son will get 50 hours of skilled nursing care out of the 112 hours he qualifies for.
“When you say, ŌĆśWe’re just cutting provider rates,’ you’re actually cutting access for him for all his needs,” Fabrello said.
Shannon Dowler, former chief medical officer for North Carolina Medicaid, said that reduced payments to dentists and other providers will lower the number of providers in the state’s Medicaid network and result in “an immediate loss of access to care, worse outcomes, and cause higher downstream costs.”
The imminent cuts in North Carolina “don’t have anything to do” with the new federal law that cuts Medicaid funding, Dowler said.
“This is like the layers of the onion,” she said. “We are hurting ourselves in North Carolina way ahead of the game, way before we need to do this.” North Carolina alone is projected to in federal Medicaid dollars over the next decade.
More than 3 million North Carolinians are enrolled in Medicaid. Deadlocked state lawmakers agreed to a mini budget in July to continue funding state programs that gave the Medicaid agency $319 million less than it requested. Lawmakers can choose to reinstate funding for Medicaid this fiscal year, Dowler said.
“We all hope it changes,” Dowler said, adding that if it does not, “you’re going to see practices dropping coverage of Medicaid members.”
Each year since at least 2019, North Carolina’s Medicaid agency has asked for more money than it received from the state legislature. A variety of federal resources, including money provided to states during the covid-19 pandemic, helped bridge the gap.
But those funds are gone this year, leaving the agency with a choice: Eliminate some optional parts of the program or force every provider that accepts the public insurance to take a pay cut. The state opted mostly for the latter.
“It’s a difficult moment for North Carolina,” said Jay Ludlam, deputy secretary for North Carolina Medicaid. The cut in the budget is “absolutely the opposite direction of where we really want to go, need to go, have been headed as a state.”
For Anita Case, who leads a small group of health clinics in North Carolina, the cuts make it harder to take care of the “most vulnerable in our community.”
Western North Carolina Community Health Services’ three clinics serve about 15,000 patients in and around Asheville, including many non-English-speaking tourism workers. Case said she will look at staffing, services, and contracts to find places to trim.
Idaho has about 350,000 people enrolled in Medicaid. This month, state leaders there responded to an $80 million state budget shortfall by cutting Medicaid pay rates .
The broad cuts have raised backlash from nursing home operators and patient advocacy groups. Leaders of one nursing home company wrote in a in the Idaho Statesman newspaper that 75% to 100% of the funding at their facilities comes from Medicaid and the cuts will force them to “to reduce staff or accept fewer residents.”
Idaho Department of Health and Welfare spokesperson AJ McWhorter said the state faced tough choices. It forecasted in Medicaid spending this year.

The Idaho Hospital Association’s Toni Lawson said the financial strain will be greatest at about two dozen small hospitals ŌĆö ones with 25 or fewer beds ŌĆö that dot the state. Lawson, the organization’s chief advocacy officer, said one hospital leader reported they had less than two days’ cash on hand to make payroll. Others reported 30 days’ cash or less, she said.
“Hopefully, none of them will close,” Lawson said, adding that she expects labor and delivery and behavioral health units, which often lose money, to be the first to go because of this latest state reduction in payments. Several hospitals in mostly rural areas of the state closed their labor and delivery units last year, she said.
Nationwide, Medicaid makes up an average of 19% of a state’s general fund spending, second only to K-12 spending, said Brian Sigritz, director of state fiscal studies for the National Association of State Budget Officers.
States generally had strong revenue growth in 2021 and 2022 because of economic growth, which included federal aid to stimulate the economy. Revenue growth has since slowed, and some states have cut income and property taxes.
Meanwhile, spending on Medicaid, housing, education, and disaster response has increased, Sigritz said.
In North Carolina, Fabrello has been unable to work outside of caring for her son. Her savings are almost exhausted, Fabrello said, and she was on the brink of financial ruin until North Carolina began allowing parents to be compensated for caregiving duties. She’s received that income for about a year, she said. Without it, she worried about losing her home.
Now, if the state reductions go through, she faces a salary cut.
“As parents, we are indispensable lifelines to our children, and we are struggling to fight for our own survival on top of it,” Fabrello said.
čŅ╣¾Õ·┤½├ĮęĢŅl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFŌĆöan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-care-costs/state-medicaid-cuts-reimbursement-big-bill-north-carolina-idaho-budgets/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2090924&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Now, another proposed twist in the rules could mean that, even though Missouri pays her to do that work, she might still have to prove to the state that she’s not unemployed.
The Kansas City, Missouri, resident has cared for her disabled son, Daniel, for all 31 years of his life. A rare genetic condition called Prader-Willi syndrome, in addition to autism, left him with an intellectual disability; a constant, excessive hunger; and an inability to speak. His needs left Gallagher, an elementary school teacher by training, with little opportunity to work outside her home.
As congressional Republicans slash in federal Medicaid spending, Gallagher is among the 18.5 million Americans who could be required to prove that they work enough to keep their health insurance.
A budget bill that passed the House and Senate would require 80 hours of work or community service a month for adults who are insured through the Affordable Care Act’s Medicaid expansion program, which has allowed states to extend Medicaid coverage to more adults with low incomes. Forty states, plus Washington, D.C., have expanded their programs, additions that now cover about 20 million Americans, including Gallagher.
She enrolled in the coverage in December 2023, after she could no longer afford her private insurance. Before her husband died of cancer in 2019, the couple paid for private insurance and supported themselves on the income he earned as a master watchmaker. After his death, Gallagher was left to earn a living and find insurance on her own. At 59, she’s too young to collect her husband’s Social Security survivor benefit.

The Medicaid program that pays for in-home care for Daniel and 8,000 other Missourians with disabilities allows family members to be compensated for caregiving, but only if they’re not the legal guardian of the person they care for. So, Gallagher went to court to give up her rights to make decisions for her son and transfer authority to her parents.
“I think it’s appalling that it’s required, but it was necessary,” she said. “There was no way I could work outside of taking care of Daniel.”
Republicans have touted Medicaid work requirements both as a way to reduce federal spending on the program and as a moral imperative for Americans.
“Go out there. Do entry-level jobs. Get into the workforce. Prove that you matter. Get agency into your own life,” Mehmet Oz, administrator of the Centers for Medicare & Medicaid Services, said in a recent interview on Fox Business.
Democrats, meanwhile, have red tape that won’t meaningfully increase employment but will cause eligible people to lose their health insurance because of administrative hurdles.
Indeed, the of Americans enrolled in Medicaid expansion are already working, caregiving, attending school, or have a disability, according to an analysis by KFF, a health information nonprofit that includes čŅ╣¾Õ·┤½├ĮęĢŅl Health News.
And while the Congressional Budget Office estimates the work requirement included in the House bill would cause to lose their insurance, only of those people are unemployed because of lack of interest in working, according to the Urban Institute, a nonprofit research group. Recent history in states that have tried work requirements suggests technical and paperwork problems have caused a substantial portion of coverage losses.
Still, the provisions are generally popular among Republican lawmakers and the public. Sen. Josh Hawley (R-Mo.), who has cutting people off from Medicaid, has signaled support for adding work requirements.
And 68% of Americans favor the requirement described in the House bill, according to a conducted by KFF. But support for work requirements dropped as low as 35% when respondents learned that most Medicaid recipients already work and could lose their coverage because of paperwork requirements.
That’s what happened in Arkansas, where 18,000 people in 2018 after the state phased in a work requirement. Thousands more were on pace to lose coverage in 2019 before a , largely over concerns about coverage losses. In discussions with focus groups, KFF found that many Arkansas Medicaid participants did not fully understand the requirements, despite the state’s outreach efforts, and some people didn’t receive mailed notices. Others were confused because the work-reporting paperwork and separate forms to renew Medicaid coverage asked for similar information.
Many family caregivers would be exempt from the work requirements proposed in Congress, but Gallagher probably would not, since she had to relinquish guardianship of her son to be paid for the work. While the hours she already logs should be enough to satisfy the requirement, she’ll need to report them again ŌĆö unless the state can identify her through its existing data. But Missouri has a history of procedural problems in the state agency that administers Medicaid.

In early 2022, for example, Missouri was taking more than 100 days on average to process applications for Medicaid expansion, a wait that prompted patients to and was more than twice the processing time allowed by federal law.
And 79% of the more than 378,000 Missourians who lost Medicaid coverage when covid-era enrollment protections ended in 2023 did so because .
The next year, a federal judge ruled that Missourians were by the state, in part because insufficient staffing at call centers left eligible people without assistance.
“They’re historically understaffed,” Timothy McBride, a health economist at Washington University in St. Louis, said of the state agency that administers Medicaid and food assistance. “I think that’s really the underlying problem.”
McBride’s analysis of Missouri’s Medicaid recipients found that of the people enrolled in expansion in 2023 were unemployed for reasons other than caregiving, disability, attending school, or retirement. But many Missourians could lose their insurance if work requirements prompt disenrollment rates similar to Arkansas’ implementation, according to a study from the Center on Budget and Policy Priorities, a left-leaning think tank that analyzes government policies.
The estimate assumes many otherwise eligible people would still lose coverage as a result of falling through the cracks, McBride said.
Hawley, who backed the Senate bill, declined to comment for this article. The senator previously that “we can sort that out” when asked about eligible people inadvertently losing Medicaid because of work requirements.

Gallagher worries about her coverage, because she recently was diagnosed with Hashimoto’s disease, an autoimmune disorder that attacks the thyroid gland. She said she had to search for her Medicaid card to fill the prescription that followed, having barely used it in the year in a half she’s been covered.
She also worries about her son’s Medicaid. A nursing home is not a realistic option, considering his needs. His coverage doubles as Gallagher’s only source of income and also pays for other caregivers, when she can find them, who give her breaks to tend to her own health and to her aging parents.
But nearly all like those Daniel receives are optional programs that states are not required to include in their Medicaid programs. And the magnitude of the cuts being proposed have that the optional programs could be chopped.
“It would destroy our lives,” Gallagher said. “The only income we would have would be Daniel’s Social Security.”
čŅ╣¾Õ·┤½├ĮęĢŅl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFŌĆöan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/medicaid/medicaid-work-requirements-missouri-mom-caregiver-son-expansion-bill/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2054969&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>
Céline Gounder, čŅ╣¾Õ·┤½├ĮęĢŅl Health News’ editor-at-large for public health, discussed on “CBS Mornings Plus” on June 10 how Health and Human Services Secretary Robert F. Kennedy Jr.’s removal of members of the CDC vaccine advisory committee could affect public health.
Freelance journalist and čŅ╣¾Õ·┤½├ĮęĢŅl Health News contributor Leah Fabel discussed child caregivers on Minnesota Public Radio’s “All Things Considered” on June 4.
- Read Fabel’s “Role Reversal: Millions of Kids Are Caregivers for Elders. Why Their Numbers Might Grow.“
čŅ╣¾Õ·┤½├ĮęĢŅl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFŌĆöan independent source of health policy research, polling, and journalism. Learn more about .
This <a target="_blank" href="/on-air/on-air-june-14-2025-cdc-acip-vaccine-committee-child-caregivers/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2049000&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>At 15, Yang, an aspiring baseball player and member of his school’s debate team, took on a new role: his mother’s caregiver.
Researchers estimate that Yang, now 18, counted among at least who provide care to an adult in their home. As state officials eye federal Medicaid funding cuts that could drastically reduce home care services for those who are disabled or have chronic health conditions, many predict that number will rise.
That’s bad news for kids: that when young people take on care for adults with medical conditions, their health and academic outcomes decline. At the same time, their loved ones receive untrained care.
“It all fell to me,” said Yang, whose sisters were 9 and 10 at the time of their mom’s accident, and whose stepdad worked nights. His grades fell and he quit after-school activities, he said, unable to spare the time.
Early on, Yang found reprieve from a personal care nurse who gave them supplies, such as adult diapers, and advice on items to purchase, such as a chair for the shower. And for about a year, Yang was able to work for a personal care agency and earn $1,000 a month caring for his mom ŌĆö money that went toward her medication and family needs.
But at the beginning of 11th grade, a change to his mom’s insurance ended her personal care benefit, sending him into a runaround with his county’s Medicaid office in Minnesota. “For a solid month I was on my phone, on hold, in the back of the class, waiting for the ŌĆśhello,’” he said. “I’d be in third period, saying, ŌĆśMr. Stepan, can I step out?’”
A in May by the U.S. Government Accountability Office reminded states that grants can be used to assist caregivers under 18. However, the future of those grants remains unclear: They are funded through the Older Americans Act, which is awaiting reauthorization; and the Administration for Community Living, which oversees the grants, was as part of the under President Donald Trump.
Additionally, if Congress approves proposed cuts to Medicaid, one of the first casualties likely will be states’ that provide critical financial relief to family caregivers, said , an economist at Lehigh University specializing in long-term health care.
Such programs, which differ by state but are paid for with federal dollars, are designed to ensure that Medicaid-eligible people in need of long-term care can continue living at home by covering in-home personal and nursing care. In 2021, they served of all Medicaid participants, costing about .
By law, Medicaid is required to cover necessary long-term care in a nursing home setting but not all home or community care programs. So, if states are forced to make cuts, those programs are vulnerable to being scaled back or eliminated.
If an aide who makes daily home visits, for example, is no longer an option, family caregivers could step in, Olenski said. But he pointed out that not all patients have adult children to care for them, and not all adult children can afford to step away from the workforce. And that could put more pressure on any kids at home.
“These things tend to roll downhill,” Olenski said.
Some studies show benefits to young people who step into caregiving roles, such as more self-confidence and improved family relationships. Yang said he feels more on top of things than his peers: “I have friends worrying about how to land a job interview, while I’ve already applied to seven or eight other jobs.”
But for many, the . Young caregivers report more depression, anxiety, and stress than their peers. Their physical health tends to be worse, too, related to diet and lack of attention to their own care. And caregiving often becomes a significant drag on their education: A found that 15- to 18-year-old caregivers spent, on average, 42 fewer minutes per day on educational activities and 31 fewer minutes in class than their peers.
Schools in several states are taking notice. In Colorado, a recently included its first question about caregiving and found that more than 12% of high schoolers provide care for someone in their home who is chronically ill, elderly, or disabled.
Rhode Island’s education department now requires every middle and high school to craft a policy to support caregiving students after a 29% of middle and high school students report caring for a younger or older family member for part of the day, and 7% said the role takes up most of their day. Rates were higher for Hispanic, Asian, and Black students than their white peers.
The results floored Lindsey Tavares, principal of , a charter high school in Cranston. Just under half her students identified as caregivers, she said. That awareness has changed conversations when students’ grades slip or the kids stop showing up on time or at all.
“We know now that this is a question we should be asking directly,” she said.
Students have shared stories of staying home to care for an ill sibling when a parent needs to work, missing school to translate doctors’ appointments, or working nights to pitch in financially, she said. Tavares and her team see it as their job to find an approach to help students persist. That might look like connecting the student to resources outside the school, offering mental health support, or working with a teacher to keep a student caught up.
“We can’t always solve their problem,” Tavares said. “But we can be really realistic about how we can get that student to finish high school.”
Rhode Island officials believe their state is the first to officially support caregiving students ŌĆö work they’re doing in partnership with the Florida-based . In 2006, the association formed the , which works with schools to provide eligible students with peer group support, medical care training, overnight summer camp, and specialists tuned in to each student’s specific needs. This school year, more than 700 middle and high school students took part.
“For kids, it’s important for them to know they’re not alone,” said , a pediatrician and an associate professor at the University of Miami who has . “And for the rest of us, it’s important, as we consider policies, to know who’s really doing this work.”
In St. Paul, Joshua Yang had hoped to study civil engineering at the University of Minnesota, but decided instead to attend community college in the fall, where his schedule will make it simpler to continue living at home and caring for his mom.
But he sees some respite on the horizon as his sisters, now 12 and 13, prepare to take on a greater share of the caregiving. They’re “actual people” now with personalities and a sense of responsibility, he said with a laugh.
“It’s like, we all know that we’re the most meaningful people in our mom’s life, so let’s all help out,” he said.
čŅ╣¾Õ·┤½├ĮęĢŅl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFŌĆöan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/aging/child-caregivers-increase-role-reversal-medicaid-cuts-trump-republicans/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2041612&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Sara Stewart was talking at the dining room table with her mother, Barbara Cole, 86 at the time, in Bar Harbor, Maine. Stewart, then 59, a lawyer, was making one of her extended visits from out of state.
Two or three years earlier, Cole had begun showing troubling signs of dementia, probably from a series of small strokes. “I didn’t want to yank her out of her home,” Stewart said.
So with a squadron of helpers ŌĆö a housekeeper, regular family visitors, a watchful neighbor, and a meal delivery service ŌĆö Cole remained in the house she and her late husband had built 30-odd years earlier.
She was managing, and she usually seemed cheerful and chatty. But this conversation in 2014 took a different turn.
“She said to me: ŌĆśNow, where is it we know each other from? Was it from school?’” her daughter and firstborn recalled. “I felt like I’d been kicked.”
Stewart remembers thinking, “In the natural course of things, you were supposed to die before me. But you were never supposed to forget who I am.” Later, alone, she wept.
People with advancing dementia do regularly fail to recognize beloved spouses, partners, children, and siblings. By the time Stewart and her youngest brother moved Cole into a memory-care facility a year later, she had almost completely lost the ability to remember their names or their relationship to her.
“It’s pretty universal at the later stages” of the disease, said Alison Lynn, director of social work at the Penn Memory Center, who has led support groups for dementia caregivers for a decade.
She has heard many variations of this account, a moment described with grief, anger, frustration, relief, or some combination thereof.
These caregivers “see a lot of losses, reverse milestones, and this is one of those benchmarks, a fundamental shift” in a close relationship, she said. “It can throw people into an existential crisis.”
It’s hard to determine what people with dementia ŌĆö a category that includes Alzheimer’s disease and many other cognitive disorders ŌĆö know or feel. “We don’t have a way of asking the person or looking at an MRI,” Lynn noted. “It’s all deductive.”
But researchers are starting to investigate how family members respond when a loved one no longer appears to know them. A qualitative study in the journal Dementia analyzed in-depth interviews with adult children caring for mothers with dementia who, at least once, did not recognize them.
“It’s very destabilizing,” said Kristie Wood, a clinical research psychologist at the University of Colorado Anschutz Medical Campus and co-author of the study. “Recognition affirms identity, and when it’s gone, people feel like they’ve lost part of themselves.”
Although they understood that nonrecognition was not rejection but a symptom of their mothers’ disease, she added, some adult children nevertheless blamed themselves.
“They questioned their role. ŌĆśWas I not important enough to remember?’” Wood said. They might withdraw or visit less often.
Pauline Boss, the family therapist who developed the theory of “” decades ago, points out that it can involve physical absence ŌĆö as when a soldier is missing in action ŌĆö or psychological absence, including nonrecognition because of dementia.
Society has no way to acknowledge the transition when “a person is physically present but psychologically absent,” Boss said. There is “no death certificate, no ritual where friends and neighbors come sit with you and comfort you.”
“People feel guilty if they grieve for someone who’s still alive,” she continued. “But while it’s not the same as a verified death, it is a real loss and it just keeps coming.”
Nonrecognition takes different forms. Some relatives report that while a loved one with dementia can no longer retrieve a name or an exact relationship, they still seem happy to see them.
“She stopped knowing who I was in the narrative sense, that I was her daughter Janet,” Janet Keller, 69, an actress in Port Townsend, Washington, said in an email about her late mother, diagnosed with Alzheimer’s. “But she always knew that I was someone she liked and wanted to laugh with and hold hands with.”
It comforts caregivers to still feel a sense of connection. But one of the respondents in the Dementia study reported that her mother felt like a stranger and that the relationship no longer provided any emotional reward.
“I might as well be visiting the mailman,” she told the interviewer.
Larry Levine, 67, a retired health care administrator in Rockville, Maryland, watched his husband’s ability to recognize him shift unpredictably.
He and Arthur Windreich, a couple for 43 years, had married when Washington, D.C., legalized same-sex marriage in 2010. The following year, Windreich received a diagnosis of early-onset Alzheimer’s.
Levine became his caregiver until his death at 70, in late 2023.
“His condition sort of zigzagged,” Levine said. Windreich had moved into a memory-care unit. “One day, he’d call me ŌĆśthe nice man who comes to visit’,” Levine said. “The next day he’d call me by name.”
Even in his final years when, like many dementia patients, Windreich became largely nonverbal, “there was some acknowledgment,” his husband said. “Sometimes you could see it in his eyes, this sparkle instead of the blank expression he usually wore.”
At other times, however, “there was no affect at all.” Levine often left the facility in tears.
He sought help from his therapist and his sisters, and recently joined a support group for LGBTQ+ dementia caregivers even though his husband has died. Support groups, in person or online, “are medicine for the caregiver,” Boss said. “It’s important not to stay isolated.”
Lynn encourages participants in her groups to also find personal rituals to mark the loss of recognition and other reverse milestones. “Maybe they light a candle. Maybe they say a prayer,” she said.
Someone who would sit shiva, part of the Jewish mourning ritual, might gather a small group of friends or family to reminisce and share stories, even though the loved one with dementia hasn’t died.
“To have someone else participate can be very validating,” Lynn said. “It says, ŌĆśI see the pain you’re going through.’”
Once in a while, the fog of dementia seems to lift briefly.
Researchers at Penn and elsewhere have pointed to a startling phenomenon called “.” Someone with severe dementia, after being noncommunicative for months or years, suddenly regains alertness and may come up with a name, say a few appropriate words, crack a joke, make eye contact, or sing along with a radio.
Though common, these episodes generally last only seconds and don’t mark a real change in the person’s decline. Efforts to recreate the experiences tend to fail.
“It’s a blip,” Lynn said. But caregivers often respond with shock and joy; some interpret the episode as evidence that despite deepening dementia, they are not truly forgotten.
Stewart encountered such a blip a few months before her mother died. She was in her mother’s apartment when a nurse asked her to come down the hall.
“As I left the room, my mother called out my name,” she said. Though Cole usually seemed pleased to see her, “she hadn’t used my name for as long as I could remember.”
It didn’t happen again, but that didn’t matter. “It was wonderful,” Stewart said.
The New Old Age is produced through a partnership with .
čŅ╣¾Õ·┤½├ĮęĢŅl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFŌĆöan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/aging/new-old-age-paula-span-dementia-alzheimers-family-members-forget-recognize-grief/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2018664&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>