Mayor Helena Moreno signed an on April 7 that creates a task force to improve the New Orleans Recreation Development Commission. One of the task force’s duties will be to “consider and make recommendations regarding the costs and practicalities of implementing a program to assess and remediate safety and environmental concerns at NORDC facilities and playgrounds, including the existence of lead in soil” and other environmental issues, according to the order.
About a week before Moreno signed that order, Deputy Mayor of Health and Human Services Jennifer Avegno announced that city officials were working with the state’s congressional delegation to request $5 million in federal funds for the federal fiscal year that starts in October. That money would go toward testing and the possible cleanup of playgrounds with elevated levels of lead. She said her office is also reviewing past city records, working with the city’s in-house experts in its Planning Commission’s Brownfield Program, and reviewing Verite’s soil test results.
“We’re trying to figure out, with whatever pots of money we can get, how can we make a more sustained and meaningful impact than we have been able to in the past?” Avegno said during an of Verite’s lead contamination investigation.
In the investigation published in February, Verite reporters tested more than 80 playgrounds for lead and documented unsafe levels of the toxic metal at just over half of them. Since then, parents across the city have called the New Orleans Recreation Development Commission, their elected officials, and other city offices seeking action.
But with the city in the midst of a budget crisis, parents and community groups in one neighborhood are taking action themselves. They are trying to raise $8,000 to hire a contractor to do extensive testing in the Bywater neighborhood’s Mickey Markey Playground, where Verite recorded lead samples that exceeded the federal hazard level of 200 parts per million — one sample registered at 403 parts per million.
“I’m aware of the city budget issues right now, and I’m also aware that fixing one playground in one neighborhood might not be a giant priority,” said Devin DeWulf, a father of two who lives in Bywater and founded the , a community organization helping with the fundraising.
Lead contamination persists in New Orleans soil, older buildings, and drinking water, posing a significant public health threat to children. Children under 6 can absorb the toxic metal more easily than adults, contaminating their blood and harming the long-term development of their brains and nervous systems.
There is no known safe exposure level for children or adults. In children, even trace amounts can result in behavioral problems and lower cognitive abilities. Chronic lead exposure for adults can increase the risk of heart problems and other health issues.
Beyond the effects on a single child or family, Avegno said, lead exposure has long-term implications, including its , which makes the issue even more critical.
“We knew we had to exhaust every avenue,” she said.
Due to low rates of testing, it’s unclear how many children across New Orleans are exposed to lead. In 2023, just 17% of children were tested for lead poisoning in New Orleans, despite a that requires medical providers to test all children by age 1 and again by 2. Currently, the state Department of Health doesn’t have a mechanism for enforcing the law.
Public health researchers recommend parents avoid playgrounds with lead contamination because it can be difficult to prevent young children from placing dirt in their mouths or breathing in dust kicked up during play.
Vann Joines, a Bywater neighborhood resident who often takes his 2-year-old daughter to Mickey Markey Playground, is part of the group raising money to independently test the playground.
“It’s really important for us to be exceedingly mindful at public playgrounds and at public parks,” Joines said.
DeWulf and Joines said they anticipate the work will take a few years and hope to create a playbook that other neighborhoods can follow for their own playgrounds.
“We could create a how-to guide on how we could effectively do this in partnerships in the city,” Joines said.
On top of the $5 million the city is requesting for soil testing and possible remediation, Avegno said the city planned to apply for a grant to help address lead at early childhood education centers.
“Your story was amazing timing,” she told a Verite reporter.
Ñî¹óåú´«Ã½Ò•îl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/public-health/lead-testing-new-orleans-playgrounds-investigation-cleanup/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2181905&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Researchers say the children at about a mile away pay the price. They discovered the students there and at other elementary schools near major pollution sites in Pennsylvania had than other children in the state.
Residents and environmental advocates saw reason for hope and relief in the form of a designed to tamp down on coke oven plant pollution. But even before it took effect, President Donald Trump granted in the U.S. — including the one in Clairton — a from the standards.
Trump and Republicans have sought to align themselves with the Make America Healthy Again movement’s populist ideals, such as improving Americans’ food choices and reducing corporate harm to the environment. But the administration is ratcheting up its attacks on the very environmental protections that MAHA followers hold dear.
Taken together, these anti-environmental initiatives will lead to more pollution-related illnesses and higher health care spending, health researchers say. They could also have political ramifications, eroding MAHA’s support for GOP candidates in the November midterm elections if followers believe the party is more beholden to industry than to the movement’s agenda.
, including about a quarter of Republicans, support rolling back environmental regulations, according to a poll by the Energy Policy Institute at the University of Chicago and The Associated Press-NORC Center for Public Affairs Research.
Some MAHA supporters believe voters will support Republicans because the Trump administration is delivering on other goals important to the movement.
“MAHA has a pretty diverse set of policy goals, ranging from medical freedom to food and the environment,” said David Mansdoerfer, who served in Health and Human Services leadership during Trump’s first term. “In totality, the Trump administration has strongly delivered on much of the MAHA agenda.”
While MAHA voters have been upset at some of the administration’s actions that promote industry, it’s hard to know how that may play out in the midterms, said Christopher Bosso, a professor of public policy and politics at Northeastern University. Many were disillusioned by a Trump they viewed as promoting glyphosate, which HHS Secretary Robert F. Kennedy Jr. has .
“The glyphosate thing really ticks off a lot of them; they’re really upset,” Bosso said. “Kennedy said it was poison. If it is a poison, why aren’t we regulating it? That’s where the tension plays out.”
The situation with the Clairton coke plant and the others granted exemptions from regulations underscores the potential public health risks. Six of the 11 factories had “high priority” violations of the Clean Air Act as of last May, according to a Ñî¹óåú´«Ã½Ò•îl Health News analysis. Five coke oven plants logged major violations every quarter for at least three years straight.
“Poisoning continues to some of the most vulnerable residents of Allegheny County,” , who had lived in nearby Glassport, Pennsylvania, said at a about the coke plant.
Environmental Protection Agency spokesperson Brigit Hirsch said the president gave companies extra time because the technology needed to meet a new standard isn’t ready yet.
“Forcing plants to comply before the tools exist doesn’t make the air cleaner, it just shuts down facilities and kills jobs with nothing to show for it,” Hirsch said.
But environmental groups disagree that the plants were unable to comply at a reasonable cost, and they say the exemption from the EPA requirements shows the Trump administration is prioritizing the coal industry at the expense of public health.
“The Trump administration’s relentless actions to dismantle lifesaving environmental protections are a gut punch to the administration’s own promise to Make America Healthy Again,” said Cathleen Kelly, a senior fellow at the Center for American Progress, a liberal think tank.
Hard Times in Clairton
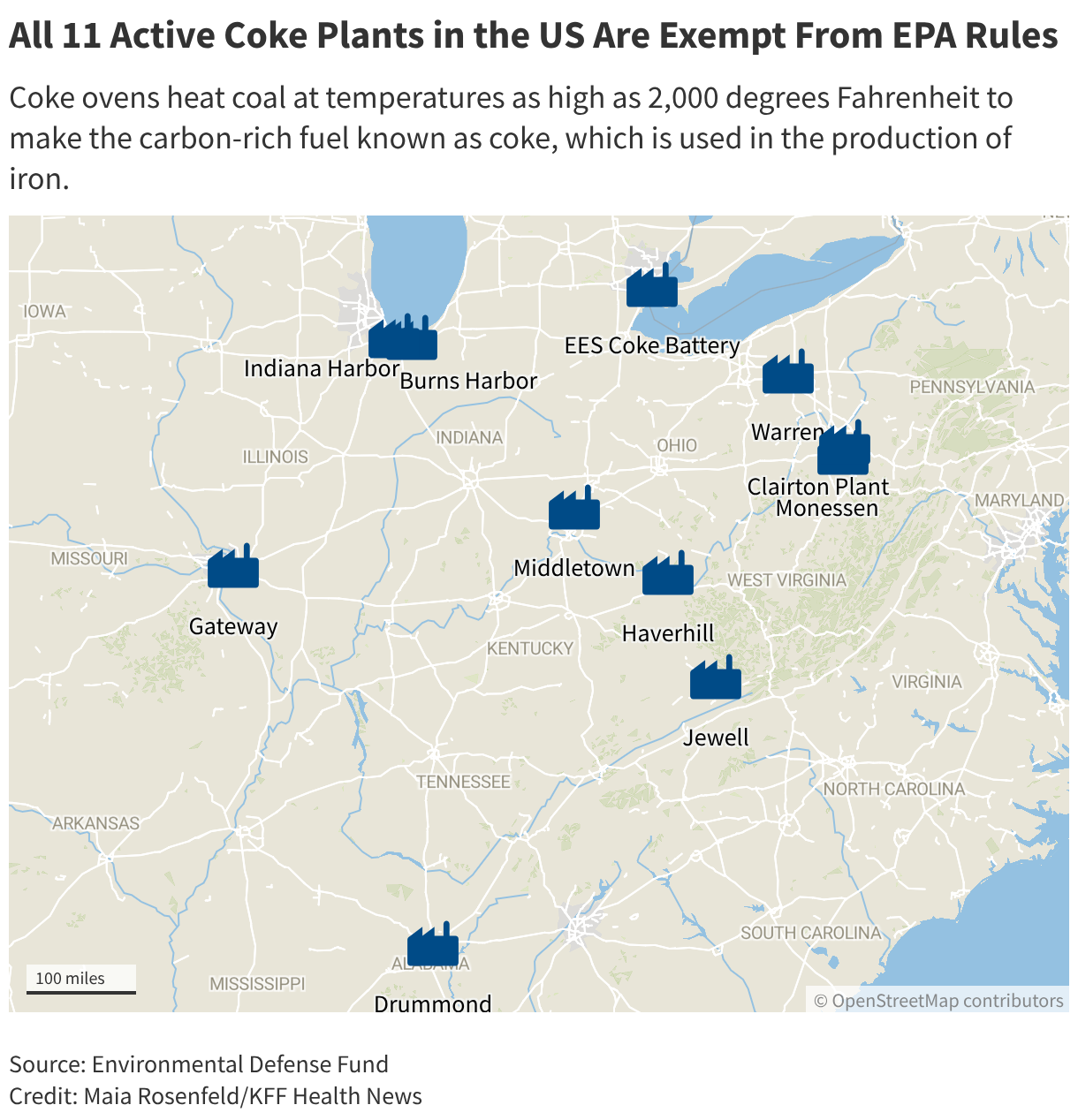
Sprawled across , the Clairton plant operates ovens in which coal is heated to as much as 2,000 degrees Fahrenheit to make up to 4.3 million tons annually of the carbon-rich fuel known as coke. The product is used in blast furnaces to produce iron.
It’s a dirty operation. The process leads to hazardous emissions of that the Centers for Disease Control and Prevention says can lead to anemia and leukemia, as well as , which can trigger severe asthma.
The Clairton operation has had repeated problems with its emissions and operations, including and of toxic chemicals. The plant has received more than from the Allegheny County Health Department since 2022, stemming largely from a fire in 2018 that led to high emissions, and violated the Clean Air Act in each of the last , with the last compliance monitoring in July 2025, according to the EPA.
Nippon Steel Corp. last year acquired U.S. Steel, which now operates as a subsidiary. The company didn’t respond to an email seeking comment. U.S. Steel said it spends $100 million annually on environmental compliance at Clairton.
“Environmental stewardship is a core value at U. S. Steel, and we remain committed to the safety of our communities,” spokesperson Andrew Fulton said in a written statement.
Clairton was once bustling with movie theaters, a mix of grocery stores, and riverside parks, with a dance pavilion and . But the decline of steel hit hard. The town’s population dwindled from more than in the mid-20th century to as of 2024. until they were razed and replaced with signs saying to keep out. The 1978 movie , which depicts a hardscrabble industrial town, is partly set there. Today, about 33% of residents live in poverty.

While the plant brings jobs and revenue, residents of the town and the surrounding areas have long complained about health problems they attribute to its emissions.
“My parents are gone. My mom had cancer, my dad,” , a Clairton resident, said at a 2025 County Council meeting. “I lost a lot of loved ones and seen other ones pass because of this mill.”
Pediatric allergist looked into asthma rates among 1,200 children who attended school near major pollution sites in the area — including students at Clairton Elementary School. They had nearly triple the national rate of asthma, with the highest rate among African American youth, according to she led.
“We were shocked,” she said. “It was double or triple what we expected. The people are proud of their industrial background. We need steel, but they’re not running a good enough operation.”
A found children with asthma living near the coke plant had an 80% higher chance of missing school when sulfur dioxide pollution was elevated.
Allegheny County, which includes Clairton and Pittsburgh, is home to a number of industrial plants, and to increased deaths, chronic heart disease, and adverse birth outcomes. It was ranked in the top 1% of counties in the nation for cancer risk from stationary industrial air pollutants in a 2018 .
Clairton has an age-adjusted cancer death rate of 170 per 100,000 people, higher than the broader county’s rate of 150 deaths per 100,000 people, based on a Ñî¹óåú´«Ã½Ò•îl Health News analysis of .
The American Lung Association in 2025 gave the county an F rating for its particle pollution levels. PennEnvironment, an environmental group that was party to a settlement with U.S. Steel involving the Clairton plant, says the coke operation caused of toxic releases in 2021, which amounted to 60% of all such releases in the county that year.
From 2020 through 2025, the Clairton plant racked up more in fines from Clean Air Act penalties than any other coke oven facility nationwide, costing U.S. Steel over $10 million, according to EPA facility reports.
“We are deeply concerned with exemptions, which allow air toxics to affect public health,” Allegheny County Health Department spokesperson Ronnie Das said in a statement.
The Clairton plant provides and hundreds of millions of dollars in tax revenue to the area. The jobs help generate nearly $3 billion in annual economic output, according to estimates from the Pennsylvania Manufacturers’ Association.
Some community members and advocacy groups hoped air quality would improve after the coke plant was sold. has pledged to upgrade facilities in the Monongahela River Valley.
Politics, Waivers, and Environmental Concerns
Under the Biden-era rule, coke plants were supposed to start meeting from the lids and doors of ovens that heat coal. They would also have had to monitor for benzene at their property lines and take steps to lower emissions of the carcinogen if they exceeded certain levels. Compliance deadlines were set for July 2025.
The Trump administration, which has sought to revive the coal industry, intervened. Last year, it , including coke plants such as Clairton’s, to seek from issued in 2024 by the EPA.
Then Trump in November went further, granting all coke plants a two-year compliance break.
The reprieve was necessary, the EPA spokesperson Hirsch said, because the requirements would have meant extra costs for the industry when standards already in effect work “extremely well” at reducing pollution.
Hirsch also said the agency under Trump is protecting the environment, pointing to action the administration has taken to called PFAS, prevent lead poisoning, strengthen chemical safety, and protect Americans’ food and water supply.
“We are building a future where the next generation of Americans is the healthiest in our nation’s history, and they inherit the cleanest air, land and water in the world,” Hirsch said.
However, the administration has taken several steps that environmental advocates say weaken health protections.
The president’s executive order on glyphosate, an herbicide the World Health Organization has linked to cancer, which touched off a who said they felt betrayed. The EPA has decided to stop considering the of reducing pollution when making policy decisions, instead focusing on the cost to industry of complying with rules. The agency also rescinded the legal and scientific basis that had long established as dangerous to public health.
The actions have rankled some MAHA enthusiasts who counted on the administration to tackle chronic disease, especially among children. A petition to Trump on with more than 15,000 signatures called for the removal of EPA Administrator Lee Zeldin, it said supported corporations over MAHA goals.
Some MAHA enthusiasts have sounded off on social media.
“No one should believe that MAHA is being upheld at the EPA at this point,” , a leader of American Regeneration, which focuses on a conservation approach to farming, said Feb. 8 on X.
, host of a , also aired her concerns on X, saying “there is something really freaking spooky going on at the EPA and I refuse to let the American people be gaslit into thinking they’re upholding the MAHA agenda.”
“A significant number of people who supported Trump are worried these rollbacks are going to hurt their health,” said , a Democratic strategist and the founder of the communications firm Third Degree Strategies. “The MAHA voters, especially women, are very sensitive to this. Republicans have put themselves in a bind.”
MAHA supporters shouldn’t be surprised by a Trump administration that doesn’t prioritize environmental protections over industry, because the president has always championed fossil fuels, said Kyle Kondik, managing editor of Sabato’s Crystal Ball, a nonpartisan election forecasting newsletter published by the University of Virginia Center for Politics.
The coke plant exemptions have disappointed some community members, environmental groups, and regulators concerned about public health and emissions.
Nearly 300,000 people live within 3 miles of the 11 active coke plants across the U.S., according to EPA data compiled by the Environmental Defense Fund.
Weakening environmental rules has helped boost Trump with the U.S. coal industry. In February, mining industry executives and lobbyists gathered at the White House, .
Coal miners, including some in white hard hats bedecked with American flags, with a bronze-colored trophy emblazoned “The Undisputed Champion of Beautiful Clean Coal.”
At the event, Trump praised their work. “We love clean, beautiful coal,” he said.
Ñî¹óåú´«Ã½Ò•îl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/public-health/clairton-pennsylvania-us-steel-make-america-healthy-again-maha-coal-coke/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2178095&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>That’s the case in New Orleans, where an investigation by Verite News found high lead levels in about half of the playgrounds on city property and found in most homes that tested their drinking water in a voluntary program.
No level of lead exposure is safe, according to federal environmental officials, but undertaking a comprehensive cleanup can be financially prohibitive. New Orleans is facing a $220 million budget deficit that has led to city employee furloughs and layoffs.
Congress allocated $15 billion over five years to lead pipe replacement under the Bipartisan Infrastructure Law, a Biden-era measure set to expire at the end of this year. In 2024, the Environmental Protection Agency also tightened the standards for lead-contaminated soil for the first time in 30 years and mandated that water systems by late 2037.
But passed by Congress and signed by President Donald Trump in January redirected $125 million of that lead remediation money to wildfire prevention. And since October, the EPA has partially rolled back protections against soil contamination, raising the federal hazard level in urban areas and the threshold for removing contaminated soil.
Tom Neltner, the national director of the nonprofit advocacy group Unleaded Kids, said it was the first time an administration had loosened the limits on lead in soil.
“ We’ve seen the Trump administration say positive things about its commitment to lead but then take actions that undermine that,” Neltner said.
But, he added, progress is still being made in some communities.
EPA press secretary Brigit Hirsch said the changes made under the Trump administration have reduced confusion and uncertainty that could hamper cleanup efforts.
“The Trump EPA’s record on protecting Americans — especially American children — from lead is unmatched,” Hirsch said in an emailed statement. “In just the last year, the Trump EPA backed up its commitment to reducing lead exposure in children with BILLIONS of dollars and historic action.”
She cited a of $3 billion available to pay for water pipe replacement. That money is from the passed during the Biden administration.
Verite News spoke with people in Michigan, Indiana, and Rhode Island to learn how they addressed their lead pollution, with the aim of finding options that could be applied in New Orleans and other cities.
“ We don’t need to do research on lead anymore,” said Tulane University professor Felicia Rabito, an epidemiologist who researches the toxic metal and its sources. “What we need are policies to get the lead out of the environment.”

Benton Harbor, Michigan: Lead Pipes Begone
Benton Harbor, a predominantly Black beach town of about 9,000 people on the southeastern shore of Lake Michigan, spent three years out of compliance with federal drinking water standards. The concentration of lead in the water remained dangerously high until residents and organizations petitioned the EPA in 2021, drawing responses from state and federal officials.
“Nobody should be drinking lead in their water for this long,” said Elin Betanzo, an engineer who provided the petitioning residents with technical support.
That year, federal officials issued an for the Michigan city to bring its water supply into compliance, and the state required Benton Harbor to replace all its lead pipes within 18 months. Gov. Gretchen Whitmer, a Democrat, committed to securing funding in the state budget for the $35 million effort, which included bottled water distribution and paying outstanding water bills for low-income residents. The state, alongside the city, allocated money from its general fund, secured regional water loans, and cobbled together grants from several federal programs to cover the total.
By the end of 2023, city officials had completed the project. Now it’s one of 21 municipalities in Michigan that have replaced all their lead pipes. Benton Harbor had more than 4,500 pipes to replace.
The Trump administration has said it would defend the Biden-era mandate for lead pipe replacement by 2037 against a lawsuit challenging it.
Betanzo recommended that utilities in other cities reduce barriers to line replacement to increase efficiency, as Benton Harbor’s water system did.
City officials saved time after assuming most pipes would be lead. They decided to go street by street, digging up, inspecting, and replacing nearly every pipe. If the pipe wasn’t lead, it wasn’t replaced, but nearly all were, Betanzo said.
Concentrating the mass replacement in one zone at a time made the contracts more cost-effective, Betanzo added. Contractors bid on zones in the city, and multiple contractors worked in different neighborhoods simultaneously. For transparency, progress was published on a public database.
The city also passed a law requiring lead lines be replaced, including those on customers’ side of the water meter. All residents had to allow the contractors onto their property or face disconnection. The residents didn’t pay for the line replacements.
“ The health benefits of lead service line replacement are greatest the sooner you get it done,” Betanzo noted, referencing a she co-authored. “If you do it wrong, you can absolutely increase exposure to lead through a lead service line replacement.”
Completion of full pipe replacement is rare in the U.S., because of the cost, poor service line tracking, the time it takes, and the prioritization of other issues. In New Orleans, the process could require up to $1 billion of investment over 10 years, according to the city’s Sewerage and Water Board.

Indianapolis: Safe Dirt for Kids
It’s not just lead pipes that are problematic. In 2024, a in the academic journal GeoHealth estimated that nearly a quarter of homes in the U.S. have unsafe levels of lead in the soil on their properties.
To that end, Indianapolis has taken some actions that other cities can learn from, said Gabriel Filippelli, a professor at the Indiana University-Indianapolis School of Science who led the study and has researched the risk of lead exposure through soil for years.
The Indy Parks & Recreation department partnered with Filippelli’s team to test a dozen parks relatively close to the contaminated site of a shuttered lead smelter.
Out of all the parks tested, Filippelli’s team found only one hot spot, beneath an old bench from which lead-based paint had flaked off into the surrounding soil.
The parks department followed Filippelli’s suggestion to replace the bench and add concrete and a thick layer of mulch and plants on the ground, so kids wouldn’t be able to play directly in the contaminated dirt.
“It was a relatively low-cost intervention,” he said, estimating it cost a few thousand dollars. The ground wasn’t excavated, and new dirt wasn’t brought in. “If you deal with it by dilution and by capping, remove the source, you’re solving the problem for today and probably many, many years to come.”
The contaminated dirt may need to be removed in some cases and replaced with clean soil, such as after severe, widespread pollution from industrial sources. But Filippelli said such extensive remediation can be impractical and too expensive for cities to undertake on their own.
Where full remediation is cost-prohibitive, Filippelli said, there are more creative solutions, like landscaping, covering the area with new dirt, or mulching. These methods won’t eliminate the lead entirely, but they will significantly reduce exposure risk.
“You can eliminate the hazard at a fraction of the cost,” he said.
Cities could also look to New York City’s , which places uncontaminated soil left over from construction projects in neighborhood-level banks for volunteers to distribute, he said.
Rhode Island: Stopping Lead at the Source
New England, home to some of the nation’s oldest homes, has led the U.S. in mitigating one of the largest ongoing sources of lead contamination: paint.
In 2023, the state legislature in Rhode Island, where most of the homes were built before lead paint was banned in 1978, passed strengthening the state’s ability to enforce tenant protections.
Prior to 2023, the state had long required most landlords to have their property inspected to ensure it met “lead safe” guidelines, said DeeAnn Guo, a community organizer for the . Although no level of lead is considered safe, replacing windows and doors that have lead paint, painting over all interior and exterior walls, and mitigating contaminated soil significantly reduce the risk of exposure.
But for years “there was no incentive to do it,” Guo said, “aside from it being the right thing to do.”
Now, landlords can be fined if they don’t have an active lead certificate on file for homes built before 1978, and the property has to be inspected every two years to remain in compliance. Before the new law, less than 15% of rentals were certified. In late 2025, that had increased to 40%, Guo said.
The state has also seen a steady decline in the in children’s blood.
Guo said it helps that the state has federal funding from the Department of Housing and Urban Development to subsidize its If a homeowner or landlord owns an old house, they can apply for the state to send an inspector. If lead is found, the state will then send a certified contractor to address the problem at little to no cost to the property owner.
Rhode Island prioritizes low-income households and homes with pregnant women or children under 6 years old, because of the heightened health risk. It can also help pay to remediate homes if a child living there has elevated levels of lead in their blood.
States and communities looking to start a successful lead paint abatement program using HUD money should combine strong enforcement, public education, and offers of subsidies, Guo said. It also helps to include community members in the planning process, she said.
Under the Trump administration, however, it might become harder for more communities like New Orleans to receive money for a “lead safe” program. Last year, HUD asked Congress to eliminate new funding for its lead hazards program, stating it would be restored in 2027. But advocates for more lead protections argue that once funding is lost, it is unlikely to be approved again.
“It shows the White House’s hypocrisy, where they talk about lead as being important and then propose eliminating the funds that are essential to cleaning up affordable housing,” said Neltner, the Unleaded Kids director. “This administration talks about the importance of children and then seems to be careless about children’s brains.”
This article was produced in collaboration with . The four-month investigation was supported by a Kozik Environmental Justice Reporting grant funded by the National Press Foundation and the National Press Club Journalism Institute. It was also produced as a project for the USC Annenberg Center for Health Journalism’s National Fellowship fund and Dennis A. Hunt Fund for Health Journalism.
Ñî¹óåú´«Ã½Ò•îl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/public-health/lead-pipes-soil-cleanup-new-orleans-benton-harbor-michigan-indianapolis-rhode-island/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2162403&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>To ensure it tastes good and is safe to drink, a small team of scientists and technicians is constantly testing the water for pH, odors, heavy metals, and microbes.
But unlike many smaller municipal utilities in the U.S., regularly checks for PFAS — per- and polyfluoroalkyl substances.
That’s a class of chemicals used by manufacturers for decades to make things like nonstick pans, cosmetics, raincoats, food wrappers, and firefighting foam.
have linked PFAS to like cancer, reduced immune system functioning, high cholesterol, and developmental delays in children.
They’re also known as “forever chemicals” because their strong chemical structures make them degrade incredibly slowly in the environment.
Today, they litter and sources around the world and can be found of almost everyone in the U.S.
One type of PFAS that the Louisville water technicians are tracking is HFPO-DA, also known by a trade name, .
Just over a year ago, workers noticed an unexpected increase in the level of GenX detected in a sample of the raw, untreated water drawn from the Ohio River for filtering and processing.
The GenX levels Louisville found in December 2024 were 15 times the reading from the previous month: 52 parts per trillion versus 3.4 ppt.
“A part per trillion is like one second in 32,800 years. Put your head around that, right?” said , the city utility’s director of water quality and research.
He offered another way to think of it: One part per trillion would be a single drop of water in 20 Olympic swimming pools.
Goodmann told Ñî¹óåú´«Ã½Ò•îl Health News and NPR he wasn’t worried about local customers’ safety, because the increased levels were still pretty low.
Risks posed by low PFAS concentrations are measured over a lifetime of exposure, he said. And recent data from Louisville shows the fell back within planned federal safety limits.
Plus, water is just one way people can be exposed to PFAS, Goodmann added. “Because you get a lot more of these pollutants from packaging, from prefixed food, cake mixes, weird things, you know, popcorn boxes,” he said.
Louisville Water’s data showed that the elevated levels of GenX in the water sample drawn in December 2024 fell once the water underwent typical treatment and filtering.

Federal Regulation Fight
The federal government has long regulated the levels of in drinking water, such as arsenic, E. coli, and lead.
But the Environmental Protection Agency didn’t issue regulations regarding PFAS until 2024, during the final year of the Biden administration. The new limits applied to in drinking water. Starting in 2029, utilities that exceeded the limits would have been required to treat the water to reduce the contamination.
But after Donald Trump’s reelection, new EPA administrator the agency will keep the rules for only two types of PFAS, called PFOA and PFOS, but drop the restrictions on the other four types, including GenX.
In addition, the EPA announced it will give water utilities two additional years, until 2031, to comply with the remaining rules, attributing the change in part to the financial burden on rural water plants.
Many utilities, large and small, may need to .
A estimated about 45% of U.S. tap water contains at least one type of PFAS.
When it announced the final PFAS limits, the Biden administration anticipated that of the estimated 66,000 U.S. public drinking water systems affected by these regulations might have PFAS levels high enough to require them to take action to reduce the contamination.
Finding the Source
Goodmann’s team traced the increased levels of PFAS up the Ohio River, past Cincinnati, and through Appalachian forests, all the way to a West Virginia factory about 400 miles upstream.
There, the uses GenX , a plastic critical to the semiconductors that power phones.
Its Washington Works facility near Parkersburg, West Virginia, has a .
A lawyer, , fought the plant’s previous owner, , in court, the company knew that a type of PFAS it was using, PFOA, was toxic but didn’t disclose that information.
DuPont went on to that claimed it contaminated local environments with forever chemicals. The company has repeatedly denied wrongdoing.
Chemours was from DuPont in 2015.
The Louisville Water team’s calculations eventually showed that the December 2024 spike in GenX levels corresponded to publicly available data from Chemours about its chemical discharges into the Ohio River.
In Chemours’ responses to filed by a West Virginia environmental group, the company denied its discharges were connected to Louisville’s GenX spike. (Louisville is not a party in the lawsuit.)
The company also contended that sampling data showed levels of GenX in the river and in downstream utilities’ treated drinking water are “indisputably safe.”
PFAS Removal Will Challenge Water Utilities
Under current federal environmental regulations, Chemours can release some chemicals into the Ohio River. But it has exceeded the legal limits repeatedly over several years, according to court filings and .
That’s why the filed its lawsuit in 2024.
The EPA in 2023, when it said it found Chemours’ West Virginia factory had repeatedly exceeded permit limits for two types of forever chemicals, GenX and PFOA.
But the West Virginia Rivers Coalition said in a court filing that the EPA’s consent order for Chemours “is not being diligently prosecuted.”
Chemours declined to answer questions from Ñî¹óåú´«Ã½Ò•îl Health News and NPR, citing ongoing litigation, except to point out that Louisville’s “finished drinking water is safe for consumption,” with PFAS levels below the EPA’s regulatory limits, as stated on and in the from Cincinnati, which also draws from the Ohio River.
As research into the health effects of PFAS exposure continues, environmental advocates say it’s imperative for companies to meet the limitations set by government permits.
“Environmental regulatory permitting is a license to pollute,” said , the water policy director for the .
“You’re permitting someone to put something into the atmosphere, into water, into soil that would not be there otherwise. And so when we talk about the safe levels,” he said, “stop using the word ‘safe,’ right? This is the maximum allowable limit.”
It is possible to remove PFAS from drinking water. For example, Louisville’s utility is spending about $23 million to redesign its powdered activated carbon system, which is one method used to take out PFAS.
But PFAS removal can get expensive, especially for small, rural towns, Hart said. Preventing contaminants such as PFAS from getting into a community’s drinking water supply is easier and less costly compared with removing it on the back end, he added.
In Chemours’ responses to the lawsuit, the company acknowledged that its violating its current permit but noted it’s working with government regulators on an eventual fix.
The federal judge in the case, , decided that wasn’t fast enough.
In August, he overpolluting. The company quickly filed an appeal.
The West Virginia Rivers Coalition declined to speak with Ñî¹óåú´«Ã½Ò•îl Health News and NPR but did point to its on the judge’s ruling.
“This is a victory for public health and the Ohio River,” Autumn Crowe, the organization’s deputy director, said in the statement. “The Court recognized what communities have known for years: Chemours has been polluting our water and ignoring its legal obligations.”
In a court filing for the case, Goodmann said that elevated levels of GenX could make it more challenging for water utilities such as Louisville’s to comply with federal rules for safe drinking water.
In regard to Chemours specifically, Goodmann told Ñî¹óåú´«Ã½Ò•îl Health News and NPR that when government regulators issue the company’s next permit, he wants them to take into account the water treatment plants downstream.
“So what we do is manage risk, and we start that at the river,” he said. “It sounds weird, but source water protection — keeping the stuff out of the river — is a big deal.”
This article is from a partnership that includes , , and Ñî¹óåú´«Ã½Ò•îl Health News.
Ñî¹óåú´«Ã½Ò•îl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/public-health/louisville-forever-chemicals-pfas-drinking-water-ohio-river-chemours-trump-epa/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2154214&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Ballad Health announced in January that it would spend about $44 million to rebuild the 10-bed Unicoi County Hospital in a field behind a Walmart in Unicoi, Tennessee, about 7 miles from the shuttered hospital that was the site of catastrophic flooding and a daring helicopter rescue on Sept. 27, 2024.
But the new location also faces significant flood risk, according to a Ñî¹óåú´«Ã½Ò•îl Health News review of information from and , two climate data companies whose flood modeling is considered more sophisticated than outdated flood maps published by the Federal Emergency Management Agency. Both Fathom and First Street estimate that a 100-year flood — a weather event more common and less intense than Helene — could cover much of the hospital site with more than 2 feet of water.
“The proposed site is so obviously a flood plain geomorphologically,” said Oliver Wing, chief scientific officer at Fathom. “You don’t need a model to see that.”
Ñî¹óåú´«Ã½Ò•îl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-industry/unicoi-county-hospital-tennessee-rebuild-flood-plain-risk-fema-ballad-health/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2152309&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>After a routine doctor visit revealed Josie had lead poisoning, Hess quickly traced the source to the crumbling paint in her family’s century-old home in the Bayou St. John neighborhood. While it underwent lead remediation, the family stayed in a newer, lead-free house near Markey.
“Everyone was telling us the safest place to play was outside at playgrounds, so that’s where we went,” Hess said. Josie became a Markey regular, playing on the swings and slides.
Josie’s next blood test was a shock. “It skyrocketed,” Hess said. Josie’s lead levels had leaped to nearly five times the national health standard. The likely culprit, according to scientists at the time, was Josie’s favorite park. Soil testing found it had dangerously high levels of lead.
City officials took no action to inform Markey’s users or make the park safe. But parents started posting warning signs at the park and flooded City Hall with calls and emails. With Josie on her hip, Hess made an impassioned speech at a City Council meeting.
In short order, the city hired a company to test Markey and other parks and pledged to fix the lead problem wherever it was found.
“My impression was they were going to make them all lead-free parks,” Hess said.
But a Verite News investigation conducted over four months in 2025 found that lead pollution in New Orleans parks not only persists — it is more widespread than previously known. Dozens of city parks with playgrounds remain unsafe, including Markey and other parks that underwent a city-sponsored lead remediation in 2011.
The findings indicate that city officials fell short in their cleanup efforts then, and that a very large number of New Orleans children are exposed to excessive amounts of lead, said Howard Mielke, a retired Tulane University toxicologist and one of the nation’s top experts on lead contamination.
“It’s a failed program,” he said. “They didn’t do what they needed to do to bring the lead levels down in a single park.”
Verite News reporters tested hundreds of soil samples from 84 city parks with playgrounds in fall 2025. Adrienne Katner, a lead-contamination researcher with Louisiana State University, verified the results. The testing found that about half the parks had lead concentrations that exceeded the established in 2024 for soil in urban areas.
“If there’s evidence of kids playing in soils that are as high as you described, that’s kind of horrifying,” Gabriel Filippelli, an Indiana University biochemist who studies lead exposure, told Verite News.

Public health researchers and doctors say that children under 6 absorb lead-laden dust more easily than adults, contaminating their blood and harming the long-term development of their brains and nervous systems. There is no known safe exposure level for children, and even trace amounts can result in behavioral problems and lower cognitive abilities.
Larry Barabino is the CEO of the New Orleans Recreation Development Commission, which oversees most of the city’s parks. He said the city doesn’t routinely test for lead in parks, and he confirmed that the last significant effort to do so was in 2011.
He called Verite’s results “definitely concerning” and pledged to work with city officials, local experts, and a city environmental consultant, Materials Management Group, to potentially remediate unsafe parks.
“It’s definitely concerning if it’s at the level that’s considered a true risk or threat, and we would get it to Capital Projects immediately to get MMG out there,” Barabino said, referring to the . “If there’s anything that’s a true environmental concern or risk, that’s something that we believe in definitely making sure we take action.”
But New Orleans is in financial straits, with a of about $220 million, and it’s unclear what resources new mayor Helena Moreno would be able to devote to restart lead remediation efforts. In response to the financial crisis, Moreno has already eliminated dozens of positions and plans to furlough 700 employees one day per pay period to save money. Moreno’s administration did not respond to requests for comment.
Andrea Young heard pledges similar to Barabino’s 15 years ago. Like Hess, Young had a child who frequented Markey and had high lead levels in her blood. Alongside other mothers, she helped push the city to take action. Young thought they had succeeded but said she now realizes that the city didn’t do enough.
“It makes me question the value” of the work the city did, Young said, “and the safety we felt in letting our kids play there again.”


Testing New Orleans Parks
Lead is typically found in very small amounts in natural soil. The average lead abundance in U.S. soils is , equivalent to less than an ounce of lead per ton of soil.
But New Orleans, like many other cities, has a long history of lead contamination in its soil, from sources including lead-based paint, leaded gasoline, and emissions from waste incinerators and other industrial facilities. Lead particles spread easily by wind, eventually settling in the topsoil.
The federal hazard level for lead in soil was 400 ppm , when the Environmental Protection Agency lowered it to 200 ppm for most residential areas and 100 ppm in urban areas like New Orleans with multiple sources of lead exposure. Last fall, the Trump administration , arguing it was confusing to have two thresholds. It didn’t argue that the 100-ppm level was safe.
More of a guide than a mandate, the EPA screening levels can steer federal cleanup actions and are often adopted by state and city governments to inform local responses to lead contamination. California has long had a much of 80 ppm.
Mielke said the Trump administration’s change doesn’t align with the science, which has long shown that children are harmed when exposed to soil with levels below 100 ppm. He was one of several scientists who had pushed for lower thresholds after the EPA established its first screening levels more than 30 years ago.
He said the 100-ppm level should still be applied in urban areas, especially New Orleans.
Verite conducted soil tests on the 84 city parks that property inventories and maps list as having play structures. Samples were taken from surface soil, which is most likely to come into contact with children’s hands and toys or be inhaled when kicked up during play or blown by the wind.
The average soil sample collected by Verite contained lead levels of about 121 ppm. Elevated lead levels tended to follow the age of the neighborhood. The city’s older neighborhoods, including the Irish Channel and Algiers Point, had some of the highest lead levels, while places like Gentilly and New Orleans East, developed mostly after the 1950s, tended to have lower levels, according to Verite’s findings.
The highest lead levels were found at Evans Park in the Freret neighborhood. Beside a low-hanging oak branch, on ground worn bare by children’s play, Verite recorded lead at 5,998 ppm, nearly 60 times the 100-ppm urban soils threshold.
Verite spoke to more than a dozen parents at playgrounds throughout the city, and most were surprised at the levels of lead in the parks.
In the Irish Channel, Meg Potts watched her son run around the dusty Brignac playground. All of Verite’s samples at that park surpassed the threshold the EPA deemed safe for urban areas, reaching nearly 600 ppm.
Potts knew high lead levels existed in the city but said she didn’t realize her neighborhood park could be a source of exposure for her son.
“ I’m just, like, thinking about all of this now because he’s had to go in and have his lead tested,” she said. “He’s like right on the cusp of having too-high lead.”
Katner, the LSU researcher, said Verite’s results can serve as a starting point for city officials to conduct more comprehensive testing in parks, noting that even a single lead hot spot in a park is concerning.
“The kid playing in that part of the park is going to get the highest dose,” she said.
A Legacy of Lead
Before the 1970s, lead was ubiquitous. A that most of the U.S. population born before the 1980s was poisoned by dangerously high levels of lead in early childhood, resulting in an average loss of at least one IQ point.
Lead pollution from cars spread into areas near roads, especially major thoroughfares, until leaded gasoline was phased out by 1996. Similarly, emissions from trash incinerators and industrial sites contaminated the surrounding soil in some New Orleans neighborhoods until they were closed in the 1970s and ’80s.
Today, the most pervasive source of lead in soil is degraded paint. Lead-based paint was used extensively for homes and buildings until it was banned in 1978. In New Orleans, most of the houses were built before 1980, according to the . As the paint deteriorates, Tulane University epidemiologist Felicia Rabito said, it can chip or turn into toxic dust.

“ The leaded paint goes straight into the dust and it goes straight into the soils, which is a major source of exposure for young children in the city,” said Rabito, who studies lead poisoning and other health conditions.
Children under 6 are especially vulnerable, in part because they like to stick their hands in their mouths. A child eating a dropped Cheerio or putting their thumb in their mouth after playing on a seesaw can be enough to cause harm. Rabito recommended that parents avoid contaminated playgrounds.
The only way to know whether a child has lead poisoning is a medical test. By , Louisiana health care providers to ensure every child between 6 months and 6 years of age receives at least two blood tests, recommended at age 1 and age 2.
But the law does not include a way to enforce those testing requirements, so many health care providers don’t test, according to a from the Louisiana Department of Health. In 2022, fewer than 1 in 10 children under 6 were screened for lead poisoning in the city, according to data from the Centers for Disease Control and Prevention.
“ There’s not anything that we can say about lead poisoning or lead levels in children in Orleans Parish with any scientific certainty,” Rabito said. “ Parents really need to get their children tested.”
Limited Soil Testing, Patchy Fixes
In 2011, the last time there was outcry over lead pollution in parks, the New Orleans health commissioner at the time, Karen DeSalvo, said the city should do “everything we can to understand what the risk might be and to remediate it.” But she also called it “not the greatest challenge, honestly,” .
Then-Mayor Mitch Landrieu promised a comprehensive response.
“The city will take all necessary measures to investigate possible lead contamination in other parks and playgrounds and remediate them as soon as possible,” he said .
Two months later, testing and remediation were completed at several parks. Parents brought their children back to the reopened playgrounds.
Despite city leaders’ assurances of a broad response, only 16 parks were tested in 2011 and the city’s piecemeal cleanup covered only patches of contaminated soil rather than entire parks, according to documents obtained through public records requests.
That stunned the vocal group of parents who had pushed for cleaning up the Markey playground. Young, one of the mothers, said the scope of the 2011 testing and remediation was much more limited than she thought.
“If the majority of the parks they tested were high, what would make them think all the others are fine?” she said.
Verite’s testing found high levels of lead at several playgrounds that were remediated in 2011, including Markey.

The results disturbed Mielke, the Tulane toxicologist.
In 2010, Mielke led an effort to reduce lead exposure at 10 private child care center playgrounds in New Orleans. He and his team covered the entire footprint of each playground with water-pervious plastic fabric and then 6 inches of Mississippi River sediment from the Bonnet Carré Spillway, a source of clean, cheap, and easily accessible soil. Lead levels fell, with most playgrounds testing below 10 ppm.
In contrast, the city’s remediation was mostly limited to areas with lead levels above 400 ppm, leaving many hazardous areas exposed. Testing and remediation reports obtained by Verite typically showed MMG focused on two or three spots in each park, with the rest going untreated.
At Easton Park in Bayou St. John, for instance, the 2011 remediation covered four areas totaling about 4,700 square feet, but the park’s playground was left untouched. Verite measured four samples around the playground that exceeded the 100-ppm threshold, including 1,060-ppm and 603-ppm readings near Easton’s swing set.
One park, Evans in the Freret neighborhood, wasn’t remediated despite lead levels as high as 610 ppm in 2011. The reason wasn’t clear in progress reports submitted by MMG. In Verite’s 2025 tests, Evans recorded the highest level, with 5,998 ppm in one location.
MMG did not respond to requests for comment.
Landrieu did not respond to a request for comment. DeSalvo, who retired last summer as Google’s chief health officer, said “extremely limited resources” forced the city to weigh its response to lead contamination in parks with the many other health threats residents faced.
“We worked to address the range of exposures whenever possible with the resources we could muster,” she said.

A Road Map for Cleanup?
Filippelli, of Indiana University, said the city should conduct comprehensive testing of every park and do regular checkups.
But because lead contamination in New Orleans parks is extensive and city leaders are struggling to close a large budget deficit, Filippelli recommends that the city remediate the worst parks first.
He and Mielke don’t believe the city must go the expensive route of full remediation, which involves digging up lead-tainted soil and trucking it to a hazardous waste landfill. It’s usually unnecessary if a park is properly capped with clean soil, Filippelli said.
Verite obtained cost estimates for 10 of the 13 parks targeted for remediation in 2011. The total cost was $83,000 in 2011, or about $120,000 today. The work covered just more than 1.3 acres across the 10 properties. Filippelli estimated that similar work could be done today for about $20,000 per acre — about a fifth of what was spent to remediate just over an acre at New Orleans parks.
Remediation should be coupled with efforts to reduce contamination from nearby sources, primarily old houses shedding lead-based paint, Rabito said.
“When you clean up soil, you’re not going to do it much good if you haven’t identified what’s contaminating the soil,” she said.
Cleaning up New Orleans parks is also likely to require sustained public pressure, said the parents involved with the lead issue in 2011.
“I was not intending to kick butts or make anybody look bad,” Claudia Copeland said of her efforts to alert parents about the dangers at Markey. “But nothing would have happened unless all these parents were calling in to the city.”
Methodology
Verite News reporters Tristan Baurick and Halle Parker were trained to use , or XRF, a handheld device that can detect the unique traits of lead at trace levels, down to 10 parts per million. The analyzer is widely used by government and university scientists.
The reporters tested 531 soil samples over a month in late 2025, following protocols developed by retired Tulane University toxicologist Howard Mielke and vetted by three other lead-contamination researchers. The reporters tested surface soil in and around play structures and other areas of parks that children use. Of the more than 110 parks in New Orleans, Verite concentrated on the 84 that city property inventories and maps list as having play structures. The reporters took between three and 11 samples at each park, depending on the size, site accessibility, and levels of contamination. A GPS device was used to record each sample’s location.
Verite’s results were reviewed by Adrienne Katner, a lead-contamination researcher at Louisiana State University. She verified the accuracy of the testing by comparing it with a smaller set of park soil samples collected by her team last summer.
While valid, the method did have limitations. The results can’t be used to determine the state of a whole park. But even one elevated soil sample can provide a starting point for city officials to conduct more comprehensive testing.
This article was produced in collaboration with . The four-month investigation was supported by a Kozik Environmental Justice Reporting grant funded by the National Press Foundation and the National Press Club Journalism Institute. It was also produced as a project for the USC Annenberg Center for Health Journalism’s National Fellowship fund and Dennis A. Hunt Fund for Health Journalism.
This <a target="_blank" href="/public-health/new-orleans-lead-contamination-parks-playgrounds-testing/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2151295&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>For those in or near Columbia Memorial, the city’s only hospital, there will soon be a different plan: Shelter in place. The hospital is building a new facility next door with an on-site tsunami shelter — an elevated refuge atop columns deeply anchored in the ground, where nearly 2,000 people can safely wait out a flood.
Oregon needs more shelters like the one that Columbia Memorial is building, emergency managers say. Hospitals in the region are likely to incur serious damage, if not ruin, and could take more than three years to fully recover in the event of a major earthquake and tsunami, according to .
Columbia Memorial’s current facility is a single-story building, a half-century ago, that would likely collapse and sink into the ground or be swallowed by a landslide after a major earthquake or a tsunami, said Erik Thorsen, the hospital’s chief executive.
“It is just not built to survive either one of those natural disaster events,” Thorsen said.
At least 10 other hospitals along the Oregon coast are in danger as well. So Columbia Memorial leaders proposed building a hospital capable of withstanding an earthquake and landslide, with a tsunami shelter, instead of relocating the facility to higher ground. Residents and state officials supported the plans, and the federal government awarded a $14 million grant from the Federal Emergency Management Agency to help pay for the tsunami shelter.
The project broke ground in October 2024. Within six months, the Trump administration had , known as Building Resilient Infrastructure and Communities, or BRIC, calling it “yet another example of a wasteful and ineffective FEMA program … more concerned with political agendas than helping Americans affected by natural disasters.”
Molly Wing, director of the expansion project, said losing the BRIC grant felt like “a punch to the gut.”
“We really didn’t see that coming,” she said.

This summer, Oregon and 19 other states sued to restore the FEMA grants. On Dec. 11, a that the Trump administration had unlawfully ended the program without congressional approval.
The administration did not immediately indicate it would appeal the decision, but Department of Homeland Security spokesperson Tricia McLaughlin said by email: “DHS has not terminated BRIC. Any suggestion to the contrary is a lie. The Biden Administration abandoned true mitigation and used BRIC as a green new deal slush fund. It’s unfortunate that an activist judge either didn’t understand that or didn’t care.” FEMA is a subdivision of DHS.
Columbia Memorial was one of the few hospitals slated to receive grants from the BRIC program, which had announced more than $4.5 billion for nearly 2,000 building projects since 2022.
Hospital leaders have decided to keep building — with uncertain funding — because they say waiting is too dangerous. With the Trump administration reversing course on BRIC, fewer communities will receive help from FEMA to reduce their disaster risk, even places where catastrophes are likely.
More than three centuries have passed since a major earthquake caused the Pacific Northwest’s coastline to drop several feet and unleashed a tsunami that crashed onto the land in January 1700, according to scientists who study the evolution of the Oregon coast.
The greatest danger is an underwater fault line known as the , which lies 70 to 100 miles off the coast, from Northern California to British Columbia.
The Cascadia zone can produce a megathrust earthquake, with a magnitude of 9 or higher — the type capable of triggering a catastrophic tsunami — , according to the U.S. Geological Survey. Scientists predict a 10% to 15% chance of such an earthquake along the fault zone in the next 50 years.
“We can’t wait any longer,” Thorsen said. “The risk is high.”

Building for the Future
The BRIC program started in 2020, during the first Trump administration, to provide communities and institutions with funding and technical assistance to fortify their structures against natural disasters.
Joel Scata, a senior attorney with the environmental advocacy group Natural Resources Defense Council, said the program helped communities better prepare so they could reduce the cost of rebuilding after a flood, tornado, wildfire, or extreme weather event.
To qualify for a grant, a hospital had to show that the project’s benefits were greater than the future danger and cost. In some cases, that benefit might not be readily apparent.
“It prevents bad disasters from happening, and so you don’t necessarily see it in action,” Scata said.
Scata noted that the Trump administration has also stopped awarding grants through FEMA’s Hazard Mitigation Grant Program, which predates BRIC.
“There really is no money going out the door from the federal government to help communities reduce their disaster risk,” he said.
A recent Ñî¹óåú´«Ã½Ò•îl Health News investigation using proprietary data from Fathom, a global leader in flood modeling, found that at least 170 U.S. hospitals are at risk of significant and potentially dangerous flooding from more intense and frequent storms. That count did not include Columbia Memorial, as Fathom’s data did not account for tsunamis. It models flooding from rivers, sea level rise, and extreme rainfall.
In recent days, an atmospheric river — a narrow storm band carrying significant amounts of moisture — dumped more than 15 inches of rain on parts of Oregon and Washington, causing catastrophic flooding along rivers and the coast. In the Washington town of Sedro-Woolley, which sits along the Skagit River, the PeaceHealth evacuated nonemergency patients.
High winds battered Astoria, leaving the city with some minor landslides, according to news reports. But flooding on the road to the nearby beach town of Seaside made the drive nearly impassable.
The Trump administration is leaning on states to take greater responsibility for recovering from natural disasters, Scata said, but most states are not financially prepared to do so.
“The disasters are just going to keep on piling up,” he said, “and the federal government’s going to have to keep stepping in.”

A Hospital at Risk
Columbia Memorial is blocks from the southern shore of the Columbia River, near the Washington border, where the include earthquakes, tsunamis, landslides, and floods. A critical access hospital with 25 beds, it opened in 1977 — before state building codes addressed tsunami protections.
Thorsen said the new facility and shelter would be a “model design” for other hospitals. Design plans show a five-level hospital built atop a foundation anchored to the bedrock and surrounded by concrete columns to shield it from tsunami debris.
The shelter will be on the roof of the second floor, above the projected maximum tsunami inundation. It will be accessible via an outdoor staircase and interior staircases and elevators, with enough room for up to 1,900 people, plus food, water, tents, and other supplies to sustain them for five days.


With most patient care provided on the second and third levels, generators on the fourth level, and utility lines underground, the hospital is expected to remain operational after a natural disaster.
Thorsen said an earthquake and tsunami threaten not only vast flooding , in which the ground loosens and causes structures above it to collapse. Deep foundations, thick slabs, and other structural supports are expected to protect the new hospital and tsunami structure against such failure.
Through the years, hospital administrators and civic leaders in Astoria have sought other locations for Columbia Memorial. But relocation wasn’t economical. Columbia Memorial committed to invest in a new hospital and tsunami shelter to protect not only patients and staff but also nearby residents.
“Your community should count on your hospital to be a safe haven in a natural disaster,” Thorsen said.

Fighting To Restore Funds
The estimated construction budget for Columbia Memorial’s expansion is $300 million, mostly financed through new debt from the hospital. The tsunami shelter is budgeted at about $20 million, for which FEMA’s BRIC program , with a $6 million matching grant from the state, which has maintained its support.
The shelter and the building’s structural protections — featuring reinforced steel, deeper foundations, and thicker slabs — are integral to the design and cannot be removed without compromising the rest of the structure, said Michelle Checkis, the project architect.
“We can’t pull the TVERS [tsunami vertical evacuation refuge structure] out without pulling the hospital back apart again,” she said. “It’s kind of like, if I was going to stack it up with Legos, I would have to take all those Legos apart and stack it up completely differently.”

Columbia Memorial has sought help from Oregon’s congressional delegation. In to Department of Homeland Security Secretary Kristi Noem and former FEMA acting administrator David Richardson, the lawmakers demanded that the agencies restore the hospital’s grant.
The hospital’s leadership is seeking other grants and philanthropic donations to make up for the loss. As a last resort, Thorsen said, the board will consider removing “nonessential features” from the building, though he added that there is little fat to trim from the project.
The in July alleged that FEMA lacks the authority to cancel the BRIC program or redirect its funding for other purposes.
The states argued that canceling the program and undermined projects underway.
In their response to the lawsuit, the Trump administration said repeatedly that the defendants “deny that the BRIC program has been terminated.”
The lawsuit cites examples of projects at risk in each state due to FEMA’s termination of the grants. Oregon’s first example is Columbia Memorial’s tsunami shelter. “Neither the County nor the State can afford to resume the project without federal funding,” the lawsuit states.
In response to questions about the impact of canceling the grant on Astoria and the surrounding community, DHS spokesperson Tricia McLaughlin said BRIC had “deviated from its statutory intent.”
“BRIC was more focused on climate change initiatives like bicycle lanes, shaded bus stops, and planting trees, rather than disaster relief or mitigation,” McLaughlin said. DHS and FEMA provided no further comment about BRIC or the Astoria hospital.


Preparing for a Tsunami Disaster
Located near the end of the Lewis & Clark National Historic Trail, Astoria sits on a peninsula that juts into the Columbia River near the Pacific Ocean.
Much of the city is not in the tsunami inundation area. But Astoria’s downtown commercial district — where gift shops, hotels, and seafood restaurants line the streets — is nearly all an evacuation zone.
Two hospitals — Ocean Beach Health in nearby Washington, and Providence Seaside Hospital in Oregon — are about 20 miles from Columbia Memorial. Both are 25-bed hospitals, and neither is designed to withstand a tsunami.
Ocean Beach Health regularly conducts drills for mass-casualty and natural disasters, said Brenda Sharkey, its chief nursing officer.
“We focus our planning and investments on areas where we can make a real difference for our community before, during, and after an event — such as maintaining continuity of care, ensuring rapid triage, and coordinating with regional emergency partners,” Sharkey said in an email.

Gary Walker, a spokesperson for Providence Seaside, said in a statement that the hospital has a “comprehensive emergency plan for earthquakes and tsunamis, including alternative sites and mobile resources.”
Walker added that Providence Seaside has hired “a team of consultants and experts to conduct a conceptual resilience study” that would evaluate the hospital’s vulnerabilities and recommend ways to address them.
Oregon’s emergency managers advise residents and visitors in coastal communities to immediately seek higher ground after a major earthquake — and not to rely on tsunami sirens, social media, or most technology.
“There may not even be cellphone towers operating after an event like this,” said Jonathan Allan, a coastal geomorphologist with the Oregon Department of Geology and Mineral Industries. “The earthquake shaking, its intensity, and particularly the length of time in which the shaking persists, is the warning message.”
The stronger the earthquake and the longer the shaking, he said, the more likely a tsunami will head to shore.
A tsunami triggered by a Cascadia zone earthquake could strike land in , according to state estimates.
Many of Oregon’s seaside communities are near high-enough ground to seek safety from a tsunami in a relatively short time, Allan said. But he estimated that, to save lives, Oregon would need about a dozen vertical tsunami evacuation shelters along the coast, including in seaside towns that attract tourists and where the nearest high ground is a mile or more away.
Willis Van Dusen’s family has lived in Astoria since the mid-19th century. A former mayor of Astoria, Van Dusen stressed that tsunamis are not a hypothetical danger. He recalled seeing one in Seaside in 1964. The wave was only about 18 inches high, he said, but it flooded a road and destroyed a bridge and some homes. The memory has stayed with him.
“It’s not like … ‘Oh, that’ll never happen,’” he said. “We have to be prepared for it.”


Ñî¹óåú´«Ã½Ò•îl Health News correspondent Brett Kelman contributed to this report.
This <a target="_blank" href="/health-industry/tsunami-shelter-oregon-hospital-fema-funding-cut-lawsuit/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2130169&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>How To Excise Politics From Health Care
More than a decade after the Affordable Care Act took effect, we’re still trapped in a confusing and costly health care maze (“Readers Take Congress to Task and Offer Their Own Health Policy Fixes,” Nov. 12). The ACA expanded coverage and protected people with preexisting conditions, but it also layered subsidies, narrow networks, and rising premiums on top of an already fragmented system. Millions still face deductibles so high that “coverage” often means financial anxiety instead of security.
The problem isn’t our doctors or hospitals — it’s the structure. America spends nearly twice as much per person on health care as other developed countries, yet our life expectancy is shorter and our outcomes worse. We’ve allowed a tangle of private insurers, billing rules, and monopoly pricing to replace coordination with chaos.
We don’t need “socialized medicine.” We need organized medicine that guarantees coverage, controls costs, and cuts red tape. Other nations have done it — efficiently, fairly, and without eliminating private choice.
Here’s what would work (with a little help from my friend ChatGPT):
1. Universal, automatic coverage. Everyone should be enrolled from birth or residency, independent of job or income. Basic care would be guaranteed, while private insurance could supplement it.
2. Rational pricing. Hospitals, doctors, and drugmakers should follow transparent, regulated price schedules — like the all-payer systems used abroad — ending the markups and cost-shifting that drive U.S. prices sky-high.
3. Streamlined administration. We spend five times as much on billing and insurance overhead as our peers. A single set of rules and electronic standards would save billions and free doctors from paperwork.
4. Invest in primary and mental health care. Paying for outcomes instead of volume would improve health and reduce preventable hospitalizations.
5. Protect families from financial ruin. National catastrophic and long-term care coverage would stop medical bills from destroying lives.
These reforms aren’t radical — they’re what nearly every successful country already does. The obstacle isn’t feasibility; it’s politics. Every dollar saved is a dollar someone currently earns, and entrenched lobbyists fight to preserve that status quo.
The ACA was a step forward, but it left us with a patchwork of subsidies, mandates, and unaffordable premiums. America already spends enough to cover everyone. The challenge now is to spend it wisely — through a rational, universal, and efficient system that works for people, not paperwork.
— Luis Albisu, Warrenton, Virginia
Beating Back Mold
There are only three ingredients to mold: spores, cellulose, and water (“A Hidden Health Crisis Following Natural Disasters: Mold Growth in Homes,” Nov. 19). The spores are floating in the air when construction is taking place. No exceptions. Cellulose is in paper and wood. Its most damaging use is in drywall or gypsum board (gyp board). A single drop of water, from a roof leak or plumbing/sewer pipe, is all that’s needed to start the mold process.
The use of drywall after World War II to build housing quickly is a primary culprit. USG and similar manufacturers make an alternative product without paper sheathing that will not react with water. USG calls it “Mold Tough,” and it uses fiberglass mat instead of paper.
As an architect, I have a simple solution: Stop the use of drywall with paper sheathing.
— Marc Brewster, Bastrop, Texas
Help Is Still Wanted
I am writing in response to the article “Help Wanted: California Looked to Them To Close Health Disparities, Then It Backpedaled” (July 28), in which Vanessa G. Sánchez explained the issues regarding health disparities among immigrant populations — such as chronic diseases, a high uninsured rate, and the more dire fact that the community health workers who do their best to support these people are paid very little for a crucial job. They offer assistance and trust to those who may not be as comfortable asking for it or are unaware that it exists because they are not from here.
She also wrote about a path opening up with the professionalization of these community health workers — how certification programs were opening up, and funding was going to increase. But it has been cut because of the budget cuts going on during this Trump administration, and programs have been slashed or abandoned.
I want to thank you for shedding light on this issue. These community health workers serve as the middle stop for health care for so many people who face immigration and language barriers. This is the workforce they appeal to and go to, and that in and of itself is honorable work that needs to be done and should be paid at a higher rate than it currently is. One could even argue it’s as important as a doctor’s visit, because even to go to the doctor, you need insurance. And who helps you with that and then sends you to the doctor? The community health workers, exactly!
I am part of the Hispanic community and care about the health disparities that exist within it, such as diabetes, and am also very aware of the language barrier that exists in the hospital field. Working together, is there a way to reinstate some certifications or training to promote higher wages and improve health for all Hispanics/immigrants?
— Avelino Cortes, San Leandro, California
Where To Draw the Line on ‘Urgent’ Care?
As a pediatric emergency medicine physician who regularly works shifts in a community hospital, I read the article on a short “nonurgent” but expensive ambulance ride for a child with interest and horror (“Bill of the Month: Not Serious Enough To Turn on the Siren, Toddler’s 39-Mile Ambulance Ride Still Cost Over $9,000,” Nov. 25). I would not have come close to guessing that an Advanced Life Support, or ALS, ambulance would cost over $9,000. Often, patients’ costs vary based on which ambulance company arrives, their insurance plan, whether they are uninsured, etc. We, at least as doctors, rarely have that information at our disposal.
I try to have parents drive their children to the referral hospital when it is safe and feasible, but this is not always possible. What risk of your child dying would you accept if you went by car? 10%? 1%? 0.1%? 0.01%? Just because no treatment was administered during this ambulance ride does not mean that the ambulance was not needed.
What makes us good at our jobs in medicine is worrying about the worst-case scenarios. Do providers sometimes overreact and send kids by ambulance who don’t need it? Absolutely. But there are also too many cases in which children die or become critically ill because someone didn’t recognize how sick the child was or the risks. If we send you in an ambulance, or admit you to the intensive care unit, because we are worried you are at risk of something like shock or respiratory failure, it doesn’t mean you will definitely need intensive care. But, if you go into shock or stop breathing while in your parents’ car, you are much less likely to survive than if we are watching for it and treat it right away. The same way that when we tell you it is a virus, after doing lots of tests, it doesn’t mean we didn’t need to do those tests. The absence of needing treatment doesn’t mean the admission or testing we recommend was unnecessary.
Perpetuating the impression that it is wasteful treatment just because everything works out well is a luxury you have when you don’t regularly see how quickly kids can go from looking relatively well to critically ill and at risk of dying. Those of us who are good at what we do know when to worry and when not to worry. Please don’t disparage our caution or treatment without even asking for our rationale. Ask this doctor why he said the baby absolutely had to go by ambulance. Maybe he didn’t have a good reason. But maybe he did. Maybe if a similar child had been sent by car and the child had gone into shock, this article would instead be talking about how incompetent he was in missing the risk of sepsis and causing the child’s death by letting the parents drive him to the hospital.
We are doing our best to provide good care in a broken, overloaded system. If we are going to work together to fix it, we all must work to understand one another’s points of view. Thank you for helping us understand these unexpected and incredibly burdensome costs our patients face. Please try to understand that caution may not be us dismissing the burden or cost but knowing the risks.
— Samantha Rosman, Boston
Investing in Your Own Health Care
About 20 years ago, I switched to a high-deductible health plan and a health savings account. It was the best decision I ever made for health care for my family (“Trump’s Idea for Health Accounts Has Been Tried. Millions of Patients Have Ended Up in Debt,” Dec. 9).
Today, after years of contributions (compounded with investment gains), the dividends and gains return a higher amount than our health care withdrawals. We’re also still contributing the max family amount per year.
We’re in the process of retiring now, and we’ll continue to select an HDHP and max out our HSA contributions. Once on Medicare, our premium payments can be made with our HSA account. Also, it’s another form of IRA once we reach age 65. It’s a double-tax-advantage account.
I don’t understand the resistance to switching to an HDHP and an HSA. The more you insure yourself, the more money you save. Long-term, it compounds into serious money. At my workplace, I try to talk as many people as possible into choosing an HDHP. They’re all so thankful years later.
I believe people are just afraid of change — not realizing it can seriously be the best health care decision they ever made.
— Tim Eckel, Toledo, Ohio
Ñî¹óåú´«Ã½Ò•îl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/letter-to-the-editor/letters-to-editor-december-2025-readers-aca-universal-health-care-mold-risks/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2127609&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>“There was mold in my bedroom, on my bed, mold in my expensive purse,” Daniels said. “Mold in my closet, my bathroom — literally everywhere.”
During her absence, a series of severe natural disasters had swept through the Tallahassee area, leaving widespread damage. According to the National Centers for Environmental Information, those storms in summer 2024 caused in destruction, displacing families and leaving businesses in ruin.
It caused more than just property damage. While the community worked to recover, mold took hold in homes and other buildings across the city, turning the natural disaster into a prolonged crisis with public health implications.
“If any part of a home is exposed to flooding or leaks and is not fully dried within 24 to 48 hours, mold growth is almost certain,” said , a research associate at Harvard T.H. Chan School of Public Health, who studies the link between mold exposure and respiratory health, particularly in the wake of natural disasters. “After major storms, we often see spikes in respiratory illnesses, particularly in homes that were affected by flooding.”
A Foundation for Trouble
An estimated in the United States contain mold or dampness. So even as the latest hurricane season winds down, the threat of mold-related health risks lingers.
And with living in flood-prone coastal counties, the risk of exposure to mold spores and allergens that can trigger respiratory illnesses is immense, leaving some 95 million people vulnerable when extreme weather strikes. That doesn’t count people in inland areas that flood, like in the North Carolina and Tennessee mountains that experienced massive flooding from Hurricane Helene last year — or those whose homes were drenched from the this summer.
The health consequences of mold exposure range from mild allergic reactions to severe respiratory conditions. Common symptoms include , according to the Centers for Disease Control and Prevention. Prolonged exposure can lead to more serious complications, such as — a rare lung inflammation — and , which can cause neurological damage, liver disease, and kidney dysfunction.
Now, a key that helps repair housing after disasters and are amid President Donald Trump’s cutbacks and policy changes.
One of the greatest dangers of mold is that it often goes undetected for months or years, leaving people unknowingly exposed.
Lauren Lowenstein in Houston knows that all too well. “For five years, my family’s health kept declining, and we had no idea why,” she said.
After conducting an test, Lowenstein said, she discovered that toxic mold spores had been growing inside the walls of her home due to excessive condensation in the HVAC system. She, her husband, and their two children vacated immediately and had to start over again.
“The mold wasn’t visible, and we had no indication that it was growing,” Lowenstein said.
Even when mold is detected, removing it is an expensive challenge. On average, mold remediation , according to the home service clearinghouse Angi, but in severe cases, the price can reach $30,000 or more. Even with home insurance coverage for mold, people may bear some cost.
Daniels, for example, was forced to leave her Tallahassee apartment and get a hotel for a month while waiting to be moved into a newly renovated unit. She had to replace all her belongings.
The cost of remediation remains out of reach for many households, Azimi said, and alternative yet affordable housing can be hard to find, which means continued mold exposure.
“For low-income and marginalized communities, the risks are even greater,” Azimi said.
For those seeking government assistance, the wait times can be extensive, according to the Rev. Mac Legerton, founder of the in North Carolina. “In many cases, families are left to choose between living in unsafe conditions or homelessness.”
A funded by the U.S. Department of Housing and Urban Development of 88 disaster grants found that its Community Development Block Grant Disaster Recovery program began distributing funds to applicants on after the initial disaster, with disbursements taking two years or longer.
“When it comes to our disaster response system, mold remediation is one of the most neglected areas at the local, state, and national levels,” Legerton said.
Legerton’s organization runs a “mold busters” program, a hands-on training and education initiative that helps give people in Robeson County the tools and knowledge they need to safely remove mold from homes, churches, and businesses following natural disasters. The program also provides free mold remediation services to vulnerable communities. He said it was created in response to the lack of timely aid in the central North Carolina community.
Waiting Takes Its Toll
Tanya Locklear faced this reality after Hurricanes Matthew and Florence severely damaged her home in Pembroke, North Carolina, in 2016 and 2018, respectively, ultimately leaving it contaminated with mold.
She applied for assistance through North Carolina’s governmental program in August 2021 but said she did not receive approval until November 2023. She said repairs finally began in February 2024 — more than two years after her application.
It was only after local advocacy efforts — including pressure from community leaders and Legerton’s organization — that her case moved forward, Locklear said.
However, she said, the initial delays had already taken a toll on her family’s health and well-being. While waiting for aid, Locklear and her children remained in the hazardous conditions of the moldy home. She said she and her family suffered health complications such as headaches, nose bleeds, and difficulty breathing.
Even today, Locklear said, she has various respiratory issues, showing the long-term risks of remaining in mold-infested homes.
Legerton, working with his group on the ground in North Carolina, believes that lawmakers and policymakers must focus on streamlining disaster relief programs to ensure effective and timely aid distribution for affected families and communities nationwide.
Government officials should also increase funding for mold remediation to help prevent displacement and long-term health consequences, and implement stronger building codes and flood-resistant housing designs to mitigate mold risk in disaster-prone areas, according to Legerton and public health experts. Without proactive policies, Azimi said, millions more will face prolonged exposure to unhealthy living conditions.
“As climate change intensifies, hurricanes and severe storms will become more frequent and destructive, increasing the risk of mold-related illnesses,” Azimi said.
Ñî¹óåú´«Ã½Ò•îl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/public-health/mold-health-crisis-natural-disasters-public-health/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2117279&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Both patients, a man and a woman, had agreed to donate their brains after they died for further research. “An amazing gift,” said Edward Lee, the neuropathologist who directs the at the university’s Perelman School of Medicine. “They were both very dedicated to helping us understand Alzheimer’s disease.”
The man, who died at 83 with dementia, had lived in the Center City neighborhood of Philadelphia with hired caregivers. The autopsy showed large amounts of amyloid plaques and tau tangles, the proteins associated with Alzheimer’s disease, spreading through his brain.
Researchers also found infarcts, small spots of damaged tissue, indicating that he had suffered several strokes.
By contrast, the woman, who was 84 when she died of brain cancer, “had barely any Alzheimer’s pathology,” Lee said. “We had tested her year after year, and she had no cognitive issues at all.”
The man had lived a few blocks from Interstate 676, which slices through downtown Philadelphia. The woman had lived a few miles away in the suburb of Gladwyne, Pennsylvania, surrounded by woods and a country club.
The amount of air pollution she was exposed to — specifically, the level of fine particulate matter called PM2.5 — was less than half that of his exposure. Was it a coincidence that he had developed severe Alzheimer’s while she had remained cognitively normal?
With increasing evidence that chronic exposure to PM2.5, a neurotoxin, not only damages lungs and hearts but is also associated with dementia, probably not.
“The quality of the air you live in affects your cognition,” said Lee, the senior author of a recent , one of several large studies in the past few months to demonstrate an association between PM2.5 and dementia.
Scientists have been tracking the connection for at least a decade. In 2020, the influential Lancet Commission to its list of modifiable risk factors for dementia, along with common problems like hearing loss, diabetes, smoking, and high blood pressure.
Yet such findings are emerging when the federal government is dismantling efforts by previous administrations to continue reducing air pollution by shifting from fossil fuels to renewable energy sources.
“‘Drill, baby, drill’ is totally the wrong approach,” said John Balmes, a spokesperson for the American Lung Association who researches the effects of air pollution on health at the University of California-San Francisco.
“All these actions are going to decrease air quality and lead to increasing mortality and illness, dementia being one of those outcomes,” Balmes said, referring to recent environmental moves by the White House.
Many factors contribute to dementia, of course. But the role of particulates — microscopic solids or droplets in the air — is drawing closer scrutiny.
Particulates arise from many sources: emissions from power plants and home heating, factory fumes, motor vehicle exhaust, and, increasingly, wildfire smoke.
Of the several particulate sizes, PM2.5 “seems to be the most damaging to human health,” Lee said, because it is among the smallest. Easily inhaled, the particles enter the bloodstream and circulate through the body; they can also travel directly from the nose to the brain.
The research at the University of Pennsylvania, the largest autopsy study to date of people with dementia, included more than 600 brains donated over two decades.
Previous research on pollution and dementia mostly relied on epidemiological studies to establish an association. Now, “we’re linking what we actually see in the brain with exposure to pollutants,” Lee said, adding, “We’re able to do a deeper dive.”
The study participants had undergone years of cognitive testing at Penn Memory. With an environmental database, the researchers were able to calculate their PM2.5 exposure based on their home addresses.
The scientists also devised a matrix to measure how severely Alzheimer’s and other dementias had damaged donors’ brains.
Lee’s team concluded that “the higher the exposure to PM2.5, the greater the extent of Alzheimer’s disease,” he said. The odds of more severe Alzheimer’s pathology at autopsy were almost 20% greater among donors who had lived where PM2.5 levels were high.
Another research team recently between PM2.5 exposure and Lewy body dementia, which includes dementia related to Parkinson’s disease. Generally considered the second most common type after Alzheimer’s, Lewy body accounts for an estimated 5% to 15% of dementia cases.
In what the researchers believe is the largest epidemiological study to date of pollution and dementia, they analyzed records from more than 56 million beneficiaries with traditional Medicare from 2000 to 2014, comparing their initial hospitalizations for neurodegenerative diseases with their exposure to PM2.5 by ZIP codes.
“Chronic PM2.5 exposure was linked to hospitalization for Lewy body dementia,” said Xiao Wu, an author of the study and a biostatistician at the Mailman School of Public Health at Columbia University.
After controlling for socioeconomic and other differences, the researchers found that the rate of Lewy body hospitalizations was 12% higher in U.S. counties with the worst concentrations of PM2.5 than in those with the lowest.
To help verify their findings, the researchers nasally administered PM2.5 to laboratory mice, which after 10 months showed “clear dementia-like deficits,” senior author Xiaobo Mao, a neuroscientist at the Johns Hopkins School of Medicine, wrote in an email.
The mice got lost in mazes that they had previously dashed through. They had earlier built nests quickly and compactly; now their efforts were sloppy, disorganized. At autopsy, Mao said, their brains had atrophied and contained accumulations of the protein associated with Lewy bodies in human brains, called alpha-synuclein.
A , published this summer in The Lancet, included 32 studies conducted in Europe, North America, Asia, and Australia. It also found “a dementia diagnosis to be significantly associated with long-term exposure to PM2.5” and to certain other pollutants.
Whether so-called ambient air pollution — the outdoor kind — increases dementia because of inflammation or other physiological causes awaits the next round of research.
Although air pollution has declined in the United States over two decades, scientists are calling for still stronger policies to promote cleaner air. “People argue that air quality is expensive,” Lee said. “So is dementia care.”
President Donald Trump, however, reentered office vowing to increase and to block the transition to renewable energy. His administration for solar installations and electric vehicles, Balmes noted, adding, “They’re encouraging continuing to burn coal for power generation.”
The administration has , announced in the Arctic National Wildlife Refuge in Alaska, and moved to stop to transition to electric cars by 2035. (The state has challenged that action in court.)
“If policy goes in the opposite direction, with more air pollution, that’s a big health risk for older adults,” Wu said.
Last year, under the Biden administration, the Environmental Protection Agency for PM2.5, noting that “the available scientific evidence and technical information indicate that the current standards may not be adequate to protect public health and welfare, as required by the Clean Air Act.”
In March, the EPA’s that the agency would be “revisiting” those stricter standards.
The New Old Age is produced through a partnership with .
Ñî¹óåú´«Ã½Ò•îl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/aging/dementia-alzheimers-air-pollution-pm2-5-particulate-matter-pennsylvania/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2110737&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>